
Health & Medicine
Chronic fatigue syndrome a kick in the guts

Using health factors and blood markers, researchers can now distinguish Chronic Fatigue Syndrome from other conditions for the first time – a giant step closer to formal diagnosis
Published 2 April 2025
As we come in to cold and flu season, many of us will be hit by a virus once, twice or even more.
But imagine if one of these ailments dragged on for weeks, leaving you with that lingering sick feeling and fatigue.
Now, envision those symptoms persisting for months.

As the months stretched on, you would likely visit your doctor multiple times, and they might even mention long COVID – a term we’ve become familiar with through widespread media coverage.
But the concept of prolonged fatigue and ongoing symptoms after an illness is not exclusive to COVID-19.
Chronic fatigue syndrome, also called myalgic encephalomyelitis (ME/CFS), can occur following many types of infections – whether bacterial, viral, parasitic or fungal – or even after stress, surgery or pregnancy.
Regardless of the initial trigger, some individuals develop a long-term illness characterised by fatigue, brain fog, unrefreshing sleep and symptom flare-ups after exertion.
This illness isn’t rare, with the Australian Government citing up to 250,000 suffering in Australia and recent lifetime prevalence projections suggesting that 1 in 30 people will suffer.

Health & Medicine
Chronic fatigue syndrome a kick in the guts
Decades before the emergence of COVID-19 and long COVID, ME/CFS was a recognised condition.
While it is often associated with young people who experience prolonged symptoms after glandular fever, ME/CFS affects individuals of all ages and can occur at any time. The term ‘chronic fatigue syndrome’ fails to give a true impression of the condition’s severity.
Approximately one quarter of those with ME/CFS are unable to leave their homes, and only about 13 per cent can maintain full-time employment.
The disease’s fluctuating severity poses a significant challenge to everyday life.
When individuals with ME/CFS feel relatively well, they can engage in daily activities. However, during symptom flare-ups, they often suffer in isolation and can become bed-bound.

One of the most troubling aspects of ME/CFS is the lack of clear answers for patients. Treatment options are limited, and none are currently approved for use in Australia.
The complexity of the disease adds to the challenge – patients experience varied symptoms, triggers and comorbidities (the simultaneous presence of two or more diseases or medical conditions in one patient), resulting in diverse responses to medication.
Obtaining a formal diagnosis is a major hurdle, as there is no diagnostic ‘biological marker’ or biomarker, for example, a molecule found in blood that can be linked to ME/CFS symptoms.
The current diagnostic process requires ruling out other similar conditions, further complicated by the presence of multiple comorbidities for ME/CFS patients.
Health & Medicine
What we now know about long COVID and our brains
Our research published in the Nature journal Communications Medicine, is a large-scale data study that highlights the development of a differential diagnostic marker.
These markers help to distinguish one condition from others that share similar symptoms and, in this case, enable a faster diagnosis for ME/CFS patients.

In the study, we used the UK Biobank to identify biological markers significant to ME/CFS in this large cohort, which includes hundreds of thousands of individuals.
UK Biobank is a large-scale biomedical database and research resource containing de-identified genetic, lifestyle and health information and biological samples from half a million UK participants.
Traditional disease diagnostic markers depend on understanding what causes the disease, for example a DNA mutation in certain types of cancers, but the cause remains unknown in ME/CFS.
However, we recognised that the current complicated diagnosis process for ME/CFS could be rapidly sped up by providing clinicians with the confidence to rule out similar conditions.

Health & Medicine
What is Post-COVID-19 Neurological Syndrome?
We looked for a pattern or signature of clinical and metabolite markers (products of metabolism) in over 1000 ME/CFS patients that distinguished them from over 80,000 people with other similar or common comorbid diseases.
Our research identified a set of 19 basic health factors and nine blood markers that could differentiate ME/CFS from seven common comorbid conditions correctly 83 per cent of the time.
The data revealed inflammation and abnormalities in cholesterol and triglycerides when comparing ME/CFS to other diseases. These findings could have significant implications for understanding the biological mechanisms underlying ME/CFS.
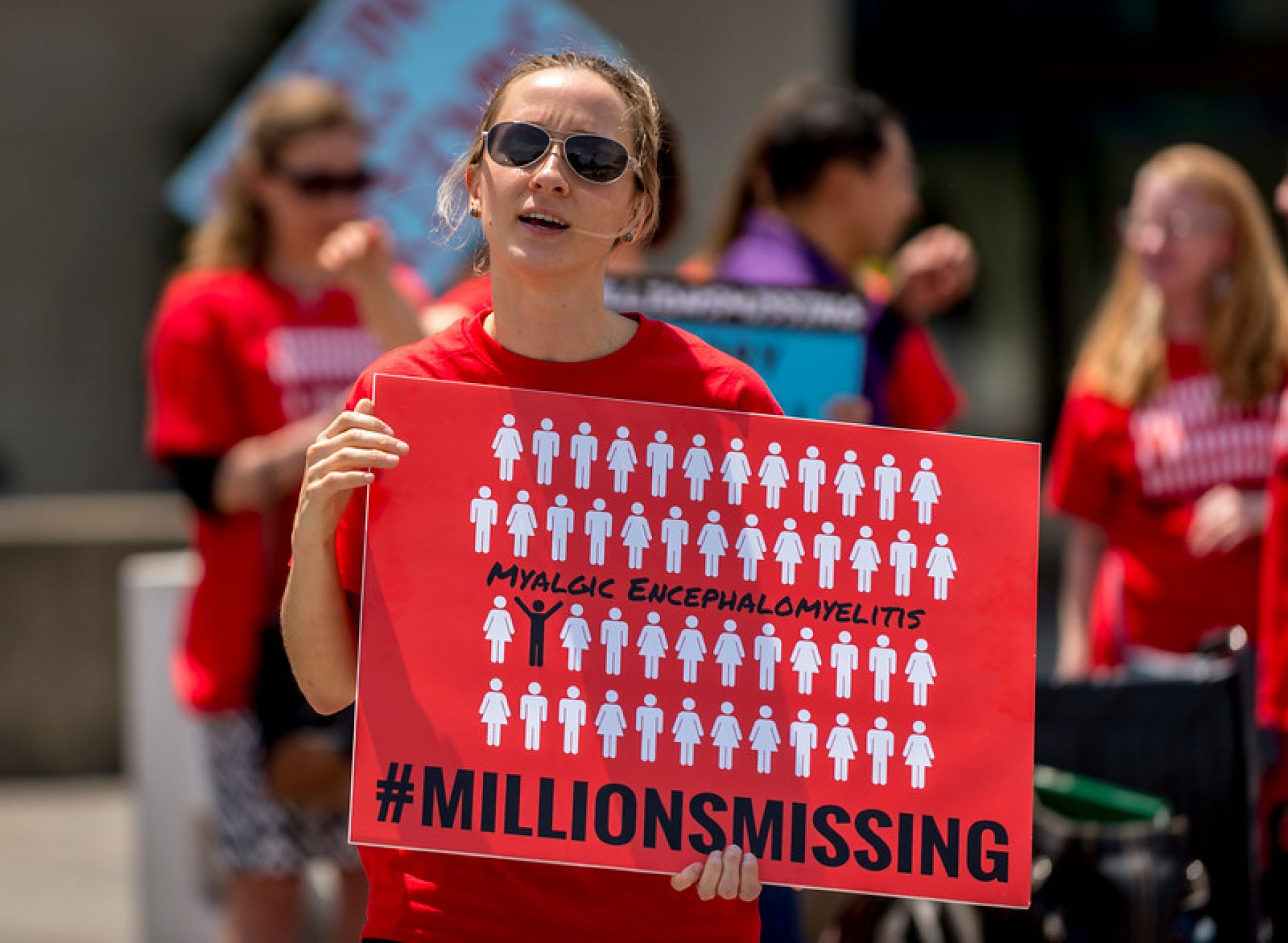
While the accuracy of this marker set is not perfect, this result is better than we expected, given that none of the UK Biobank data we identified was collected with ME/CFS in mind.
We are hopeful that this study provides a new path to being able to rapidly diagnose ME/CFS and to assess severity for treatment trial outcomes.
The next challenge we are working on is to translate this research to clinical use in the community.
This work was funded by OMF Australia, through the Melbourne ME/CFS Collaboration, and the Mason Foundation.