
Health & Medicine
We need to keep talking about miscarriage

Pre-eclampsia and eclampsia are complications of pregnancy that can endanger a woman and her newborn, yet a key treatment isn’t being used in many parts of the world
Published 14 October 2021
Pre-eclampsia and eclampsia are dangerous disorders causing high blood pressure during pregnancy.
After haemorrhage, they are the second leading direct cause of death among pregnant or recently pregnant women – accounting for about 14 per cent of maternal deaths worldwide.
When pre-eclampsia worsens to eclamptic seizures, it can be fatal to both women and babies. Women in low and middle-income countries are disproportionately at greater risk of dying from pre-eclampsia and eclampsia, which is indicative of a lack of access to appropriate and life-saving care.
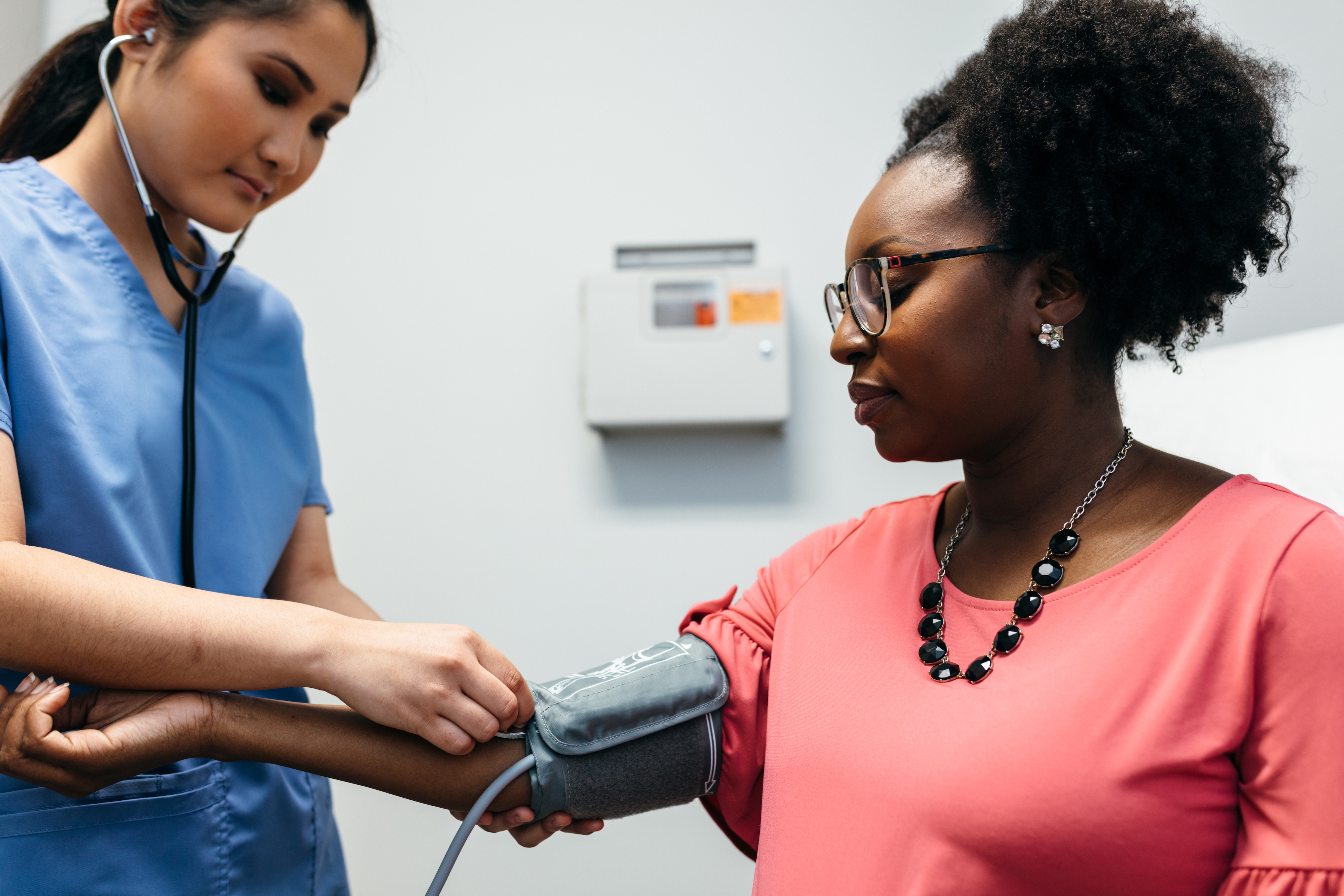
In some cases pre-eclampsia and eclampsia can be safely cured by birth, but for others there is a medication to prevent or treat eclamptic seizures.
Magnesium sulphate is the most effective anticonvulsant for women with eclampsia, reducing the risk of death by more than 50 per cent. In 2002, the Magpie trial showed that it can also prevent seizures in women with severe pre-eclampsia, halving their risk of developing eclampsia.
Magnesium sulphate is safe, relatively cheap, cost effective and recommended by the World Health Organization.

Health & Medicine
We need to keep talking about miscarriage
The problem is that this life-saving treatment isn’t universally or correctly used – particularly in lower resource settings. Understanding why is essential if we are to improve health outcomes for women and babies.
We conducted a systematic review of all available qualitative evidence to explore the factors affecting the appropriate use of magnesium sulphate globally. We identified 22 studies that explored the perspectives of healthcare providers, administrators and policy makers, almost all in low and middle-income countries.
Their perspectives highlighted the complexity of the issue, showing that a broad range of factors can affect the uptake of magnesium sulphate.
For providers to use magnesium sulphate they must be both competent and confident in administering it. Many providers are aware of its effectiveness and acknowledge it is the preferred treatment.
However, our review highlights that fears of complications or adverse events from magnesium sulphate can undermine confidence in its safety.

Serious side effects from excessive magnesium sulphate occur rarely, especially in women with good kidney function. These side effects are generally related to the level of magnesium in the blood becoming too high, which can lead to respiratory depression, altered consciousness or heart problems.
Delaying the next dose is usually sufficient to resolve them or administering calcium gluconate is an effective antidote.
Studies found that some providers felt fearful, cautious or concerned when using magnesium sulphate. Providers may also be less familiar with it compared to other, less effective treatments (like diazepam or phenytoin) and may prefer these alternatives due to their training or previous clinical experience.

Health & Medicine
Midwives on the COVID-19 frontline in Indonesia
Our review found that providers are less likely to use magnesium sulphate or may use it incorrectly, when they are unsure about how to appropriately administer it.
For example, many reported difficulties identifying and preparing a correct dosage, which can undermine their willingness to use it.
Moreover, providers believed that they needed to more closely monitor women after administering magnesium sulphate, which was challenging in resource-constrained environments.
Sometimes the packaging size of magnesium sulphate differs from the locally recommended dose – a problem that could be mitigated through more consistent clinical protocols and ready-to-use doses.
Knowledge about magnesium sulphate and how to use it, as well as practical first-hand experience, are important for ensuring it is used appropriately. Both can be improved through practical in-service training and clearer clinical management protocols.

Another issue is that healthcare facilities can often run out of stock due to supply chain problems. These include individual drug suppliers having a monopoly over local supply, a lack of incentives to produce and market magnesium sulphate, and shortcomings in procurement systems.
We also found mixed messages about the affordability of magnesium sulphate.
While it is often said to be “inexpensive” and “cheap’” studies show that costs can still be ‘prohibitive’ for some women and their families. Sometimes families must purchase magnesium sulphate independently from local pharmacies at higher prices that can discourage use.

Health & Medicine
The facts of vaccinating our kids against COVID-19
These problems in ensuring adequate supplies and monitoring equipment can undermine the confidence of healthcare facilities and practitioners in administering magnesium sulphate.
For example, beyond supplies of magnesium sulphate, healthcare facilities also need sufficient blood pressure monitors, urine dipstick tests, laboratory and diagnostic equipment, as well as medications to manage side effects, not to mention sufficient beds for monitoring women.
Insufficient staffing for monitoring is also a problem given women can experience eclampsia at any time including after hours.
Treatment can be made more timely if an initial dose of magnesium sulphate can be delivered at a local healthcare facility before a woman is transferred to a better equipped facility for subsequent monitoring and doses.
But this depends on a timely diagnosis of the condition and having effective referral systems to an appropriately equipped higher level provider, which does not always happen in practice.

These collective perspectives and experiences of healthcare providers, administrators and policy makers confirm that improving uptake of magnesium sulphate is a complex task. However, they also reveal a range of opportunities to take practical action.
Based on our research we have developed a set of questions to assist health system administrators and policy makers to develop policies and procedures.
These are aimed at increasing provider competence and confidence, improving health system capability and ensuring effective knowledge translation. Priority issues may vary between different local contexts and these should be explored during intervention design.

Health & Medicine
Supporting kids with cerebral palsy go for gold with cycling
For example, in practice policies and guidelines are sometimes inconsistent, ambiguous or unavailable, and they aren’t always followed. Improving the availability and use of facility policies and clinical practice guidelines is essential to encourage providers to use magnesium sulphate appropriately.
These guidelines must be evidence-based, consistent with national and international guidelines, and adapted for local context.
Policy makers, clinicians and organisations should also act as ‘champions’ of magnesium sulphate by raising awareness of its effectiveness and encouraging uptake.
Targeted, evidence-based interventions to improve magnesium sulphate uptake can be implemented readily – preventing further unnecessary maternal and neonatal deaths from pre-eclampsia and eclampsia.
This would be a huge step towards ensuring that all women everywhere are receiving the appropriate care for what are dangerous, but manageable, complications of pregnancy.
Banner: Getty Images