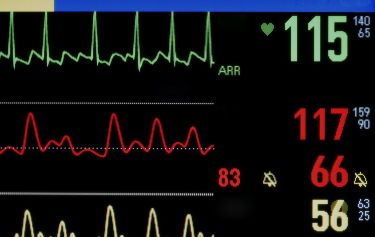
Health & Medicine
World-first test could predict your risk of a heart attack

Since the 1970s, the number of people dying because of heart disease and stroke has fallen. But there are worrying signs that this decline is slowing in countries like Australia
Published 5 August 2019
Since the 1970s, some countries have seen the number of deaths from cardiovascular disease – mostly heart disease and stroke – fall by 40 to 80 per cent.
This was a major yet often unheralded global public health achievement that underpinned substantial increases in life expectancy.
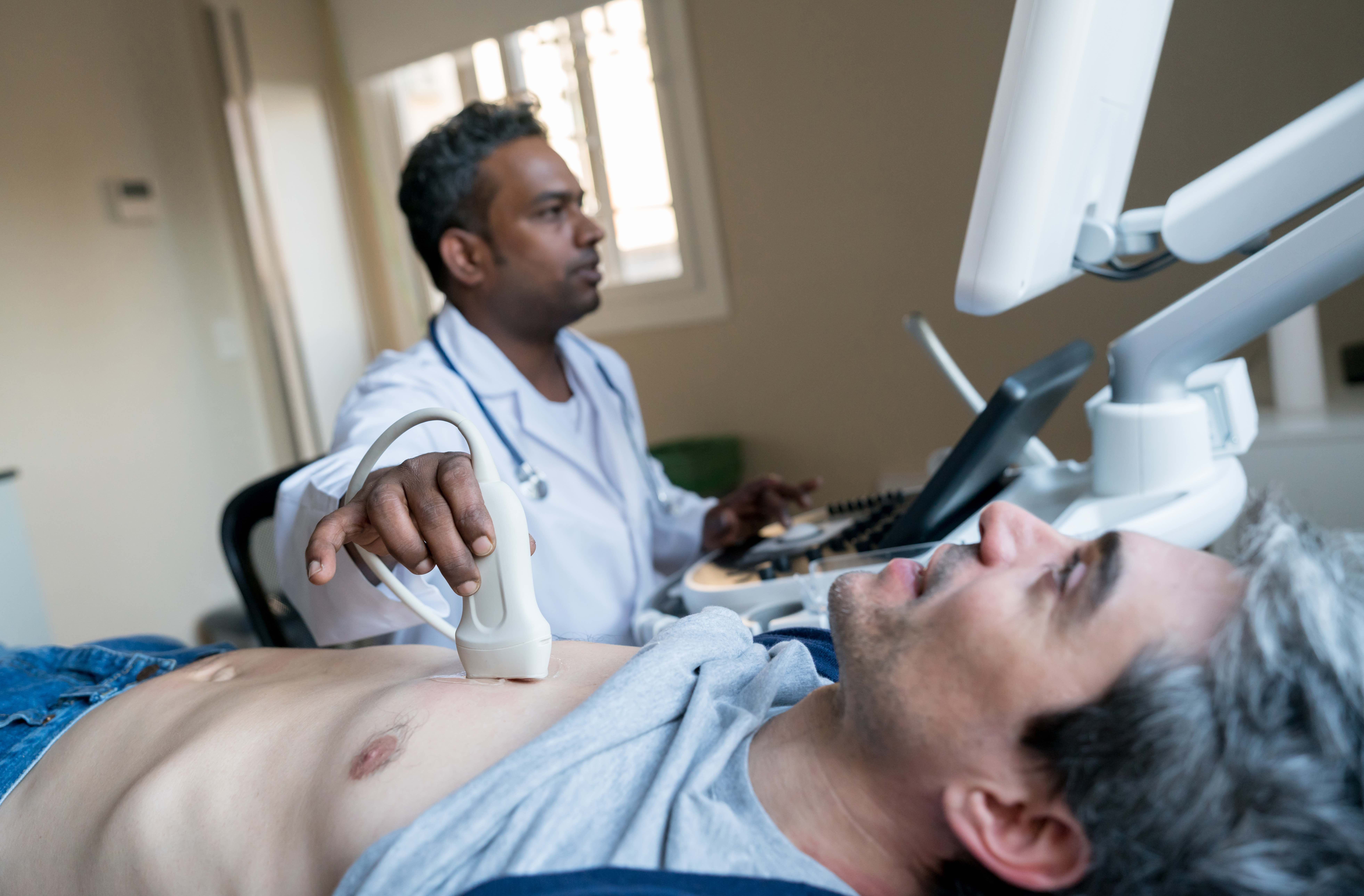
Major drivers of these decades-long falls were reductions in smoking prevalence due to anti-tobacco campaigns, reduced fat in our diets, lower alcohol intake and improved screening, emergency care and treatment of these diseases.
Australia was a leader in these kinds of public health interventions and also helped lead the worldwide decline in cardiovascular disease mortality and an increase in life expectancy.
But our study, published in the International Journal of Epidemiology, has found cardiovascular disease mortality rates have almost stopped declining in many high-income countries, including Australia.

Health & Medicine
World-first test could predict your risk of a heart attack
In fact, we found that in some parts of the world, rates have even started to rise.
This trend is concerning given the widespread high prevalence of risk factors such as obesity, and it has potential implications for future trends in life expectancy.
We analysed trends in cardiovascular disease mortality, which is mainly comprised of heart disease and stroke, in 23 high-income countries since the year 2000; and found that cardiovascular disease mortality rates in people aged 35 to 74-years-old are now barely declining, or are increasing, in 12 of the 23 countries.
The recent slowdown in cardiovascular disease mortality is happening across high-income countries with diverse epidemiological environments – that is, incidence, distribution, and control of diseases – and it’s English-speaking countries that appear to be worst affected.
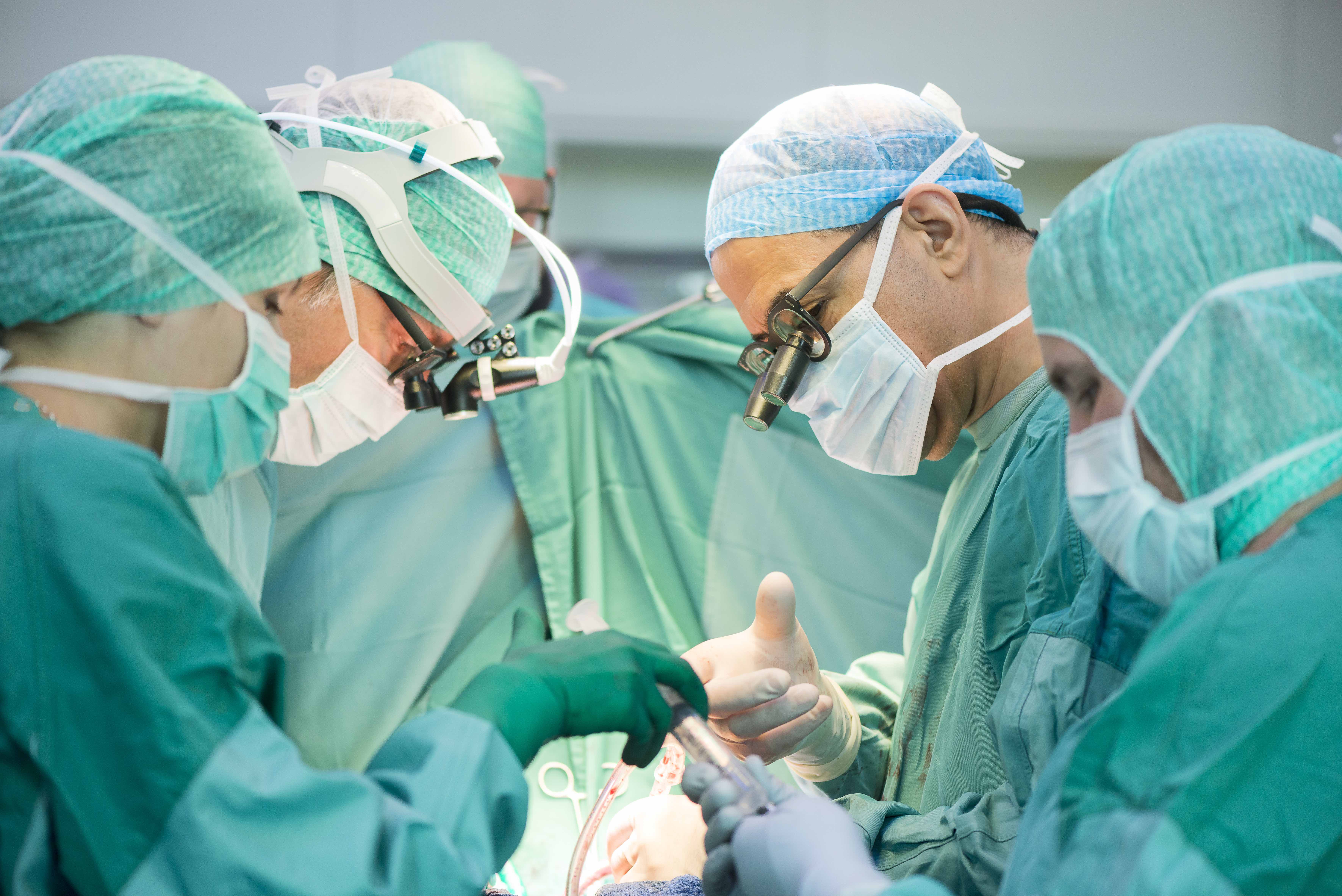
Cardiovascular disease mortality rates in both the USA and for Canadian females have increased in the most recent year, while in Australia, the United Kingdom and New Zealand annual declines in deaths from cardiovascular disease are now only 20 to 50 per cent of what they were in the 2000s.
Each of these countries has very high levels of obesity. In Australia, close to one-third of adults are obese.
These increases in obesity levels mean that a significant portion of the population has been exposed to the cardiovascular disease risks associated with being overweight for several decades.

Health & Medicine
How Australia is losing the health fight
Evidence shows a clear increase in cardiovascular disease mortality risks with increasing obesity. One study shows the risks for people who are extremely obese are similar to those for smokers.
This suggests that obesity, or at least poor diet, may have been a significant contributor to the slowdown in the decline of cardiovascular disease deaths.
But obesity is only one of many risk factors for cardiovascular disease mortality. Others include high blood pressure, high cholesterol and diabetes.
Obesity levels are low in Italy and France where the slowdown in cardiovascular disease mortality in recent years is among the most notable of all countries.
Another possible explanation for the recent slowdown in mortality decline is that tobacco smoking rates have already fallen so low that additional declines in countries, like Australia, will be harder to achieve and have much less impact on mortality than in previous years.

Cardiovascular disease is still the leading cause of death in Australia, so this slowing decline in the reduction of deaths from the disease has major implications for life expectancy.
Recent research shows that life expectancy increases in Australia are slower than in most high-income countries, and have stagnated over the past few years.
The Australian Bureau of Statistics has significantly revised down its projections of future life expectancy increases, and Australia’s life expectancy increases to 2040 will be among the lowest of all high-income countries, according to a multi-country forecast.

Health & Medicine
Heart plumbing: The pipes matter
Our research shows that the effect of successful public health interventions on cardiovascular disease mortality over the past 50 years is diminishing.
In order to combat this, significant investment in preventive health measures is needed, particularly those aimed at increasing physical activity, improving diet and reducing obesity.
We also need to continue efforts to reduce rising inequalities in cardiovascular disease risk factors and to improve access to health care across the population.
Failure to address these issues could confirm the end of the long-term decline in cardiovascular disease deaths and threaten future gains in life expectancy.
Banner: Shutterstock