
Health & Medicine
Why you should go on a clinical trial
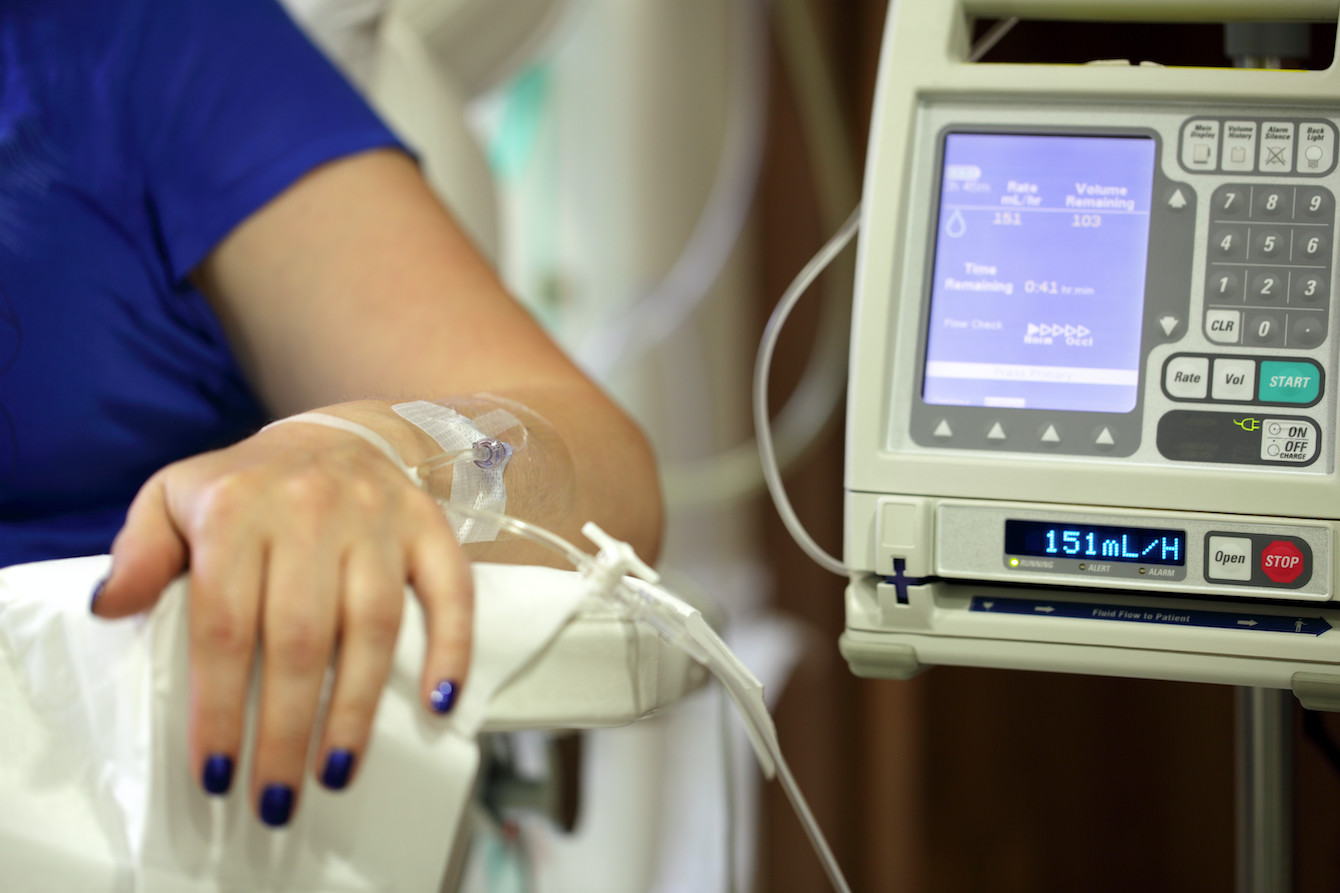
Traditional clinical trials have been vital for improving cancer treatments for the last 70 years, but new data-driven approaches can enhance treatment for individuals and better allocate healthcare resources for everyone
Published 8 April 2020
Since the 1950s, the evidence for most cancer breakthroughs has been generated using traditional randomised clinical trials.
These trials involve recruiting patients onto an often large clinical trial, randomly assigning trial participants to one of a number of treatments, following each patient until the trial is over, and then analysing that data to clearly understand what does and does not work in the broader population.
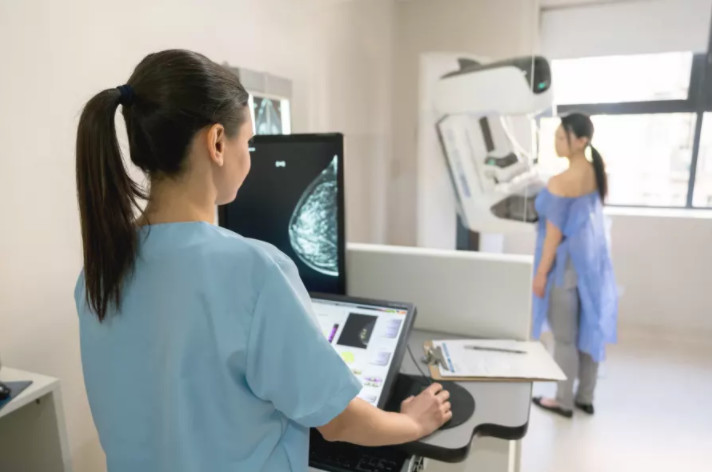
However, as we learn more about cancer, we can develop better ways to target treatments to the person and their individual cancer, rather than the trial population.
But in this dawning age of personalised cancer treatment, traditional clinical trials are often too slow, too simple or too costly to help discover what treatments work for different people.
For example, innovative treatments that target patients’ immune systems can potentially cure some cancers. But many traditional clinical trials take too long, often several years, to keep up with treatment innovation while at the same time are too short to learn about long-term outcomes.

Health & Medicine
Why you should go on a clinical trial
To personalise a treatment, many small and different groups of individuals need to be studied, so large traditional trials of some personalised cancer treatments may never be possible. Meanwhile, the dollar cost of traditional trials for drug approval is also often in the tens of millions, further limiting their use in a world with limited healthcare resources.
New approaches to cancer research can overcome some of these challenges, either by designing trials around the patient rather than the population or by leveraging existing clinical registries.
These registries are databases that track how patients interact with the health system and often contain a wealth of information on what treatments each patient received and how they responded, alongside other important clinical data.
They provide valuable information on routine clinical practice since none of the patient interactions are controlled by strict trial rules and patients are not excluded based on their clinical characteristics.
What this means is that these registries provide a more representative snapshot of the real-world compared with traditional trials – as a result, they are often referred to as ‘real-world registries’.
Clinical registries can be used to answer different types of research questions. For example, registries can be used to obtain insights into real-world treatment practices and their corresponding health outcomes.

Indeed, when a registry contains sufficiently rich clinical information it can be used to compare the real-world effectiveness of certain treatments, which is not possible using traditional trials.
Data from clinical registries can also be used to produce ‘real-world’ control groups to serve as a benchmark for single-arm trials, which are non-randomised trials where everyone receives the same trial treatment.
Single-arm trials only capture data for an experimental treatment, but these trials are increasingly used to approve new treatments in place of traditional randomised controlled trials.
By matching single-arm trials with real-world control arms, experimental treatment efficacy can be better assessed.

Health & Medicine
Health data saves lives: We need to be using it better
Registry-based randomised controlled trials, also known as ‘registry trials’, combine the strengths of traditional randomised trials with real-world registries.
Clinical registries can be used for both trial recruitment and data collection, meaning that participants are representative of the real-world population and can be enrolled quickly. Additionally, large trial costs can be reduced substantially by leveraging existing infrastructure.
Incorporating a randomised trial design also provides confidence in results of comparative studies.
Following the initial landmark registry trial published in 2013 by a Swedish cardiology team, registry trials are being adopted across multiple disease types in Australia and internationally.
These trials typically investigate the best use of standard treatments rather than new therapies, where intensive monitoring is required to ensure the treatments are safe.
Registry trials have a unique role within a learning health system, where evidence can be generated from routine care to inform best practice.
Bayesian adaptive trials or sequential multiple assignment randomised trials (SMARTs) are two types of trials that are designed around patients. Bayesian adaptive trials are exciting because they can allow trials to be modified in-progress as new information becomes available.

By doing so, they can randomise a greater proportion of new trial participants to whatever treatment seems the most promising or completely drop treatments that are likely to be futile.
Importantly, it means participants have a much better chance of receiving the best treatment before the trial is even over.
In contrast, traditional trials simply randomise a fixed and unchanging proportion of patients to each treatment, so many patients may end up receiving less efficacious treatments that don’t achieve the desired outcome. Adaptive trials are often smaller, faster, and less expensive than traditional trials, and so are increasingly more attractive to researchers, funders and society in general.

Health & Medicine
Science, society and drug design
SMARTs are relatively underutilised but show great promise, particularly for cancers that often require extended and complicated treatment regimens.
These trials work by continually monitoring trial participants and randomising them to different treatments if the one they currently are on stops working.
Not only are these trials attractive to patients, because all trial patients have an opportunity to switch from treatments that do not work for them, but they also uniquely allow researchers to learn about the optimal sequencing of treatments which is of real clinical and economic importance.
Beyond trials, the methods that have been designed to analyse SMART data also have great potential to be applied to existing clinical cancer registries to better understand how to optimally sequence treatments in routine care.
Continued improvement in outcomes for people dealing with the consequences of cancer requires continual innovation.
Traditional trials have been crucial to improving cancer treatments for the last 70 years, but the time has come for new data-driven approaches to take the fore.
By using the best tools for the job, we can enhance how each patients is treated and better allocate scarce healthcare resources to the ultimate benefit of everyone.
Banner: Shutterstock