
Breathing easy: Treating steroid resistant asthmatics
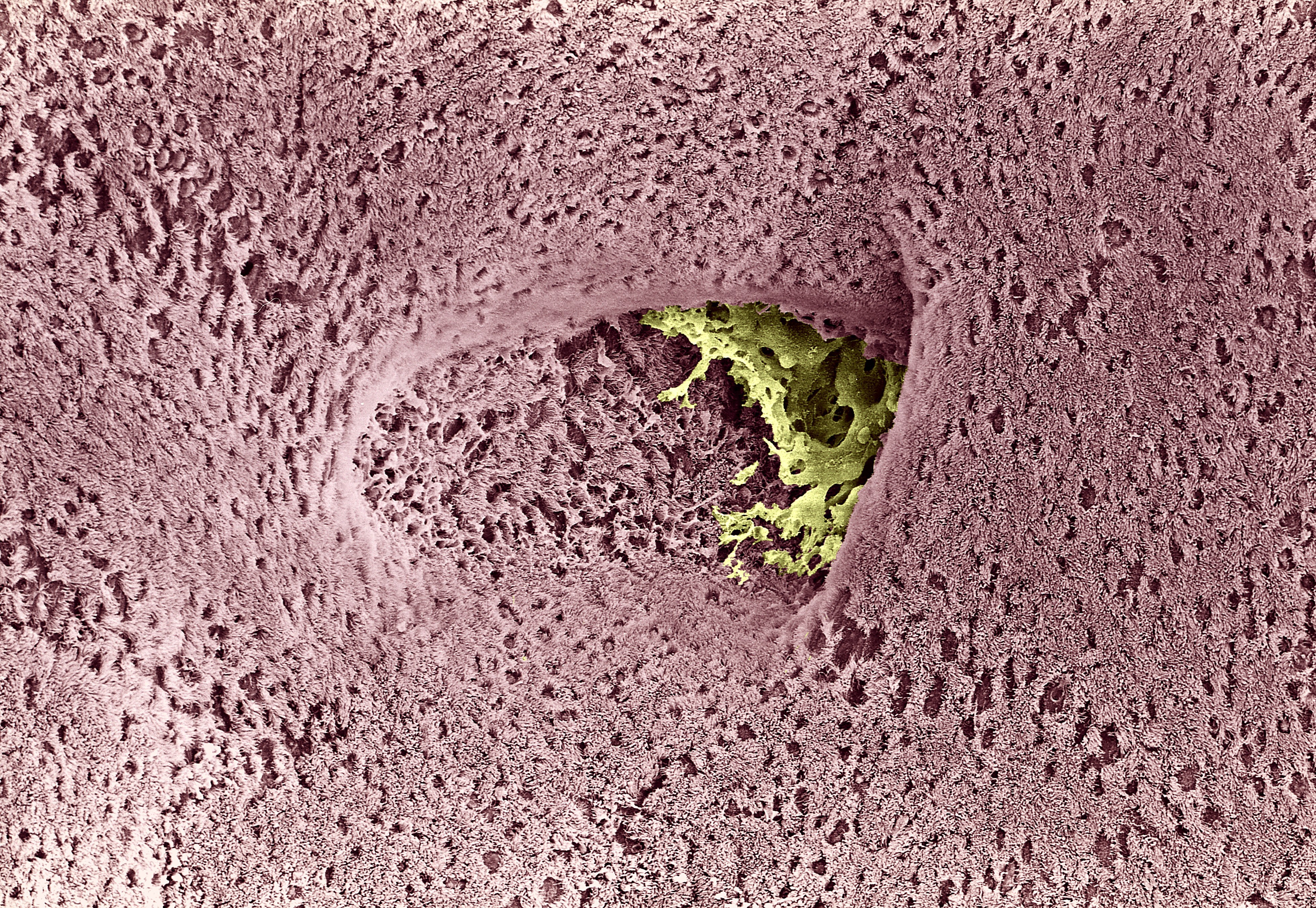
Steroid resistance in the lungs is a critical problem for severe asthmatics, but researchers have tracked down the molecular cause and a new inhaled treatment is on the way
Published 16 July 2018
Asthma is a readily controllable condition for most asthmatics, but not all of them.
For people with severe asthma – about five per cent of the 300 million sufferers worldwide – controlling a suffocating attack is difficult and scary because the steroids delivered by their inhalers simply don’t work well enough.
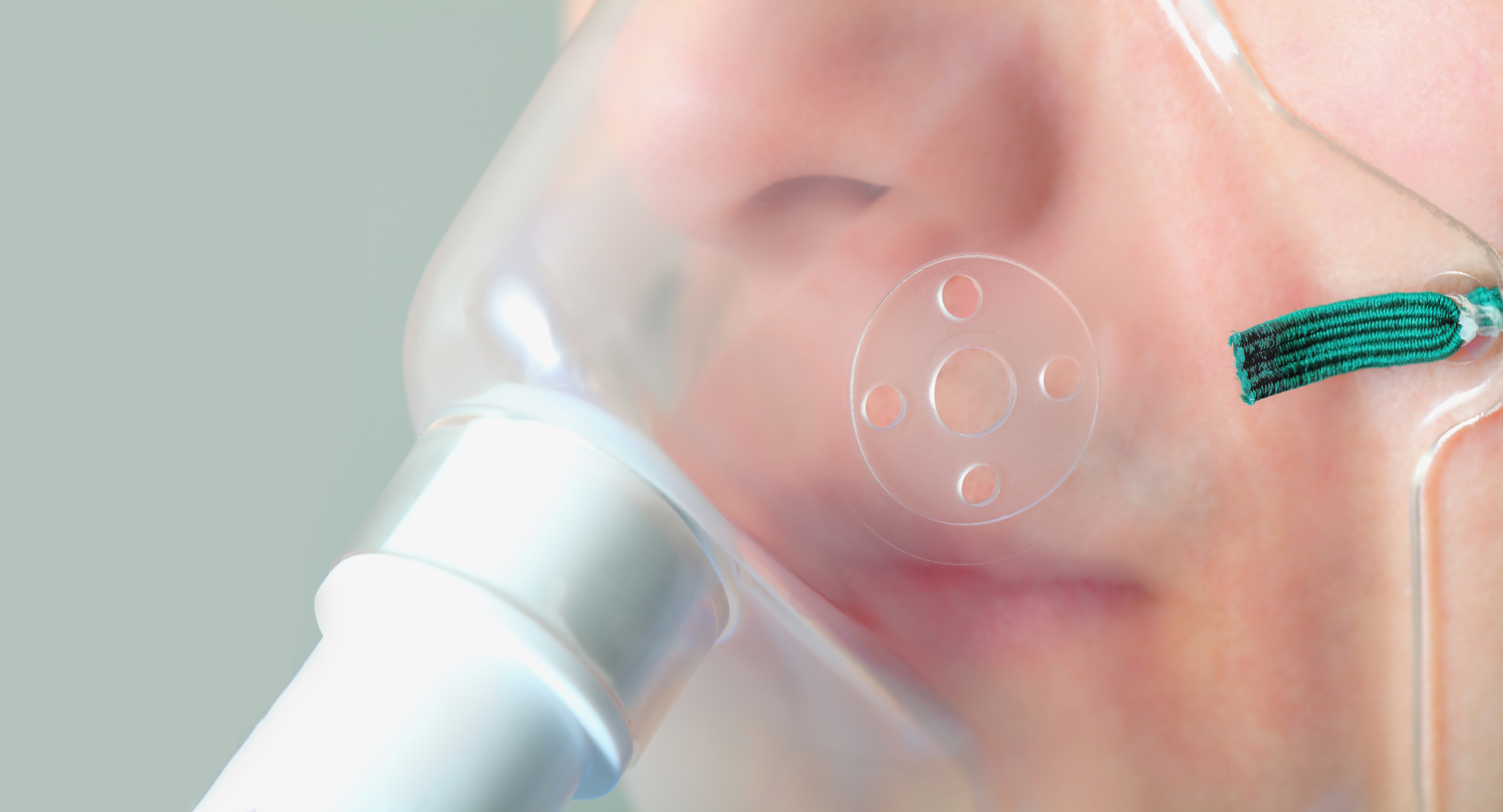
A viral infection like influenza or a cold can trigger inflammation in the lungs that in some severe asthmatics isn’t eased by steroids. Even worse, some asthmatics develop chronic steroid resistance.
It means frequent visits to the hospital for treatment and in some cases even mechanical ventilation is needed to aid oxygen delivery. This involves sending oxygen into the lungs through a tube passed into the airway from the throat.
But now researchers have discovered the molecular process that triggers steroid resistance in an unlikely place – our body clocks. And they’ve found a way to stop it in an even unlikelier place, a compound that was being developed in an attempt to treat people with drug and alcohol addictions.

New inhaled treatment
“The happenstance we see in biology is continually amazing, but this vulnerable group of asthmatics really need some happenstance,” says lead researcher Professor Alastair Stewart at the University of Melbourne. “These severe asthmatics, are four times more likely to end up in hospital when their symptoms worsen than other asthmatics.”
A therapy is now under development that may turn out to be the first really new inhaled asthma treatment since inhaled steroids were first introduced in 1972. Once the researchers establish the safety of the therapy they can start extensive clinical trials in a process that can take between six-to-eight years.
It was more than ten years ago that Professor Stewart’s lab team first discovered that a key protein involved in regulating our immune systems – TGF-Beta – was part of the mechanism by which steroid resistance emerges in the lungs. The protein triggers a tissue repair response that can become chronic and, over time, scar and stiffen the lung tissue in a process call fibrosis.
“We actually made this discovery by accident,” says Professor Stewart. “We’d been investigating how steroids influence the ability of TGF-Beta to turn surface lining cells into tissue cells. But when our lab experiments unexpectedly revealed that TGF-Beta could blunt the anti-inflammatory effects of steroids we refocused on that area.”
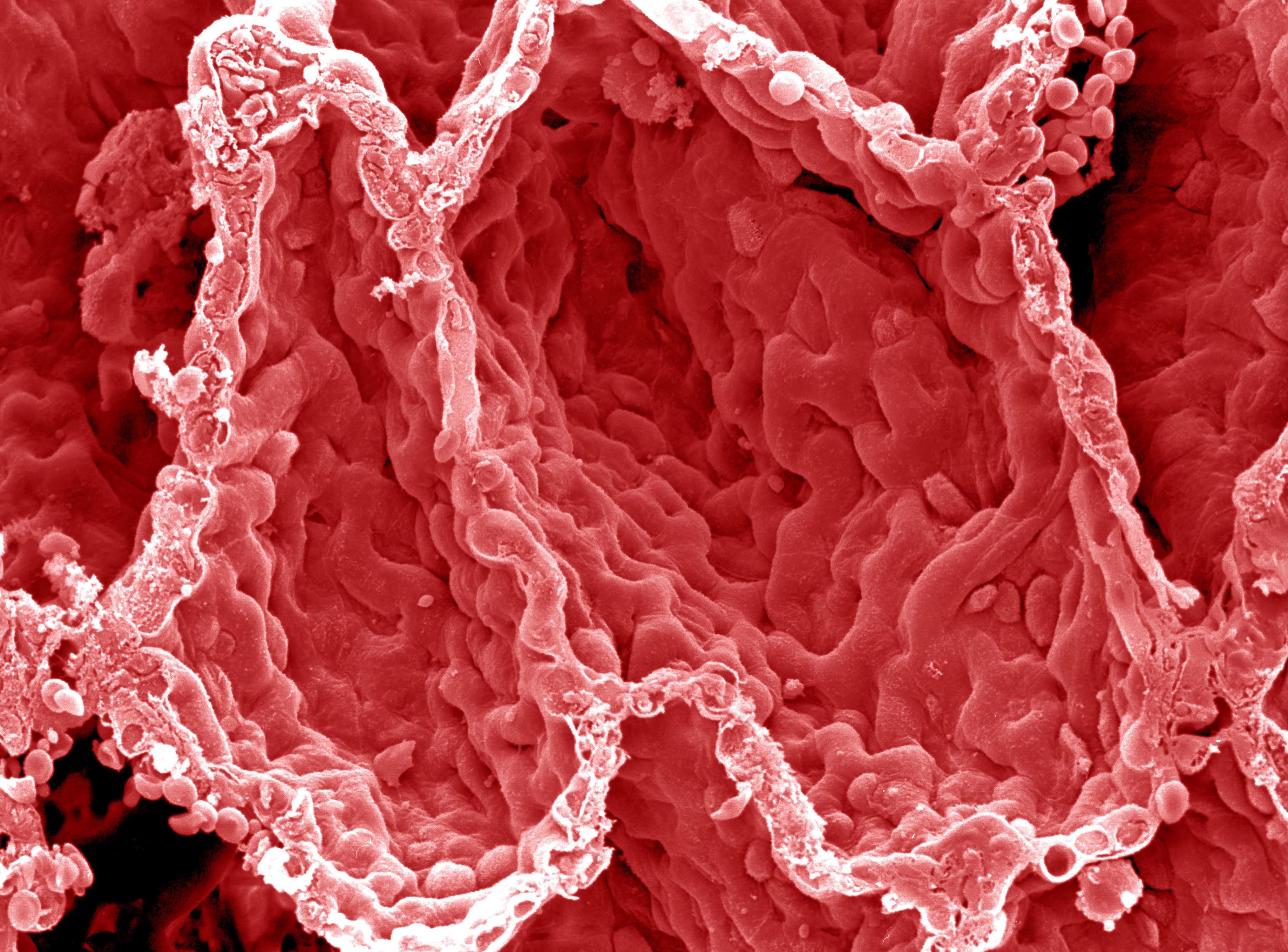
“It was an exciting discovery because it meant that if we could understand the mechanisms involved at a molecular level, we stood a good chance of unpicking this molecular machinery to restore steroid responsiveness.”
Following the pathways
TGF-Beta uses about 20 known different “pathways” or sequenced actions when it is activated by different mechanical and chemical signals sensed outside the lung cell. These pathways dictate which of TGF-Beta’s many functions the cell will perform.
“We now had a laundry list of different mechanisms that we simply had to go through.”
Health & Medicine
Putting the brakes on lung disease
But seven years later they were up a blind alley.
After meticulously testing all the pathways they still had no idea how TGF-Beta triggered steroid resistance. It was a huge anticlimax, but secretly Professor Stewart was relieved.
He knew that if a pathway involving many of the important actions of TGF-Beta had been found as the cause, it would have been incredibly difficult to safely block, as TGF-Beta is critical to our immune system and wound healing. Simply “turning off” the TGF-Beta protein could be extremely toxic, putting people at risk of cancer and a host of autoimmune gut diseases like colitis.
“The students were all disappointed, but I was quietly pleased. I knew that we didn’t want to be interfering with TGF-Beta too broadly because it is just too valuable to our immune surveillance,” says Professor Stewart.
It was then that PhD student Meina Li began to probe whether the key could be found further down one of the molecular signal pathways that connect TGF-Beta to different cell actions. She began searching previous research on TGF-Beta, reviewing about a hundred papers going back over 20 years.

“I decided to look downstream along the signalling pathways, but there are many enzymes involved and there was a lot of research to go through,” says Dr Li. “But I eventually found two papers with research results that suggested to me that an enzyme called Casein Kinase-1 (CK1) may be involved.”
Hidden in the body clock
This literature finding aligned with on-going experiments being conducted by team members Dr Christine Keenan and Ms Trudi Harris on a chemical called D4776 that has many enzyme targets, including CK1.

Sciences & Technology
Thunderstorm asthma: Counting pollen to save lives
CK1 is a major chemical regulator of our biological clocks, otherwise known as our circadian rhythms. These rhythms regulate our various states from alertness to sleep. Our eyes sense light and darkness and feed this information into the clock so that we feel sleepier when it’s dark.
The primary biological clock responding to light is located in our brains, but the clock enzymes like CK1 are spread throughout the body. It wasn’t an obvious target for research on the immune system or wound healing.
The team began hunting around for a better way to interfere with CK1’s interaction with TGF-Beta. They came across an existing drug-like chemical, prosaically named PF670462. The drug had originally been developed to explore whether CK1 could be manipulated to treat sleep disorders and counter cravings – there is evidence that disruptions to the body clock may make people more prone to addiction.
But when they experimented with PF670462 on human lung tissue in the laboratory they discovered it blocked CK1 from carrying the TGF-Beta signal, and it restored steroid sensitivity in the airway cells.
“It is a good example of the importance of a very diligent researcher not relying on derivative studies, but going back to the original work,” says Professor Stewart.
“Many thousands of papers on TGF-Beta are published every year, and the work on CK1 and TGF-Beta had effectively been lost in this morass, but we have been able to exhume it and it is now at the centre of our work to develop this new therapy.”
Drug development
The main challenge now is in finalising the development of new compounds that more precisely target steroid resistance in the lungs. And because they are targeting CK1 only in the lungs, the researchers are hopeful that testing will show that inhibiting CK1 won’t affect our central body clock.
This process of testing will benefit from separate work by Professor Stewart to develop multi-cell three-dimensional “models” of human tissue called organoids that can be grown in laboratory dishes and made to mimic the reactions of human organs.
Health & Medicine
Putting cells through their paces
He is leading an Australian Research Council funded Centre for Personalised Therapeutics Technologies that aims to develop and use organoids to better test the efficacy and safety of experimental drugs like PF670462.
“Our goal is to develop a formulation of this drug compound that could be delivered into the lungs through a simple nebuliser (vaporiser) without having any significant effects on our circadian rhythms or immune defences,” says Professor Stewart.
And, once it’s on the market, it means steroid-resistant asthmatics will be able to breathe a whole lot easier.
Professor Stewart and his School of Chemistry colleague Professor Spencer Williams, are progressing toward drug development with the financial assistance of the University of Melbourne, The National Health and Medical Research Council, Asthma Australia, and the Victorian Government.
Banner Image: Scanning electron micrograph of a bronchus, or airway, of a human lung. Picture: David Gregory & Debbie Marshall/Wellcome Collection



