
Health & Medicine
Caring for India’s elderly during COVID-19

An international study has helped to quantify China’s multiple chronic disease burden as COVID-19 places even more pressure on the country’s health system
Published 22 May 2020
When it comes to public health, China is a complicated case study.
The government, via its Healthy China 2030 Plan and a series of far-reaching health reforms, has set a bold vision for achieving universal health coverage and important advances have been made in achieving increased access to primary healthcare and financial protection for Chinese citizens.

However, while some city dwellers live a modern lifestyle with access to quality medical care, many people reside in villages and rural areas that may not. With a population nudging 1.4 billion, this presents many health challenges – some more obvious than others.
University of Melbourne researchers investigating the extent of chronic health problems in China have found that in some cases, those with higher socioeconomic and education levels have poorer health outcomes.
The findings are part of a major study with Harvard University and Imperial College London that produced the first national longitudinal data set of its kind to quantify China’s burden of multiple chronic disease.

Health & Medicine
Caring for India’s elderly during COVID-19
Until now, the impact of people having more than one non-communicable disease wasn’t fully quantified, making it more difficult to identify those at risk and target health programs.
Published in The Lancet Global Health, the new research could have significant implications for China’s economic and health systems. It is also timely as COVID-19 places further pressure on the public health emergency management system in China.
The study focused on multimorbidity – that is, when a person has two or more mental or physical chronic non-communicable diseases (NCDs). In this case, they included diagnosed hypertension and self-reported diabetes, dyslipidaemia, heart disease, stroke, cancer, chronic lung disease, digestive disease, liver disease, kidney disease and arthritis.
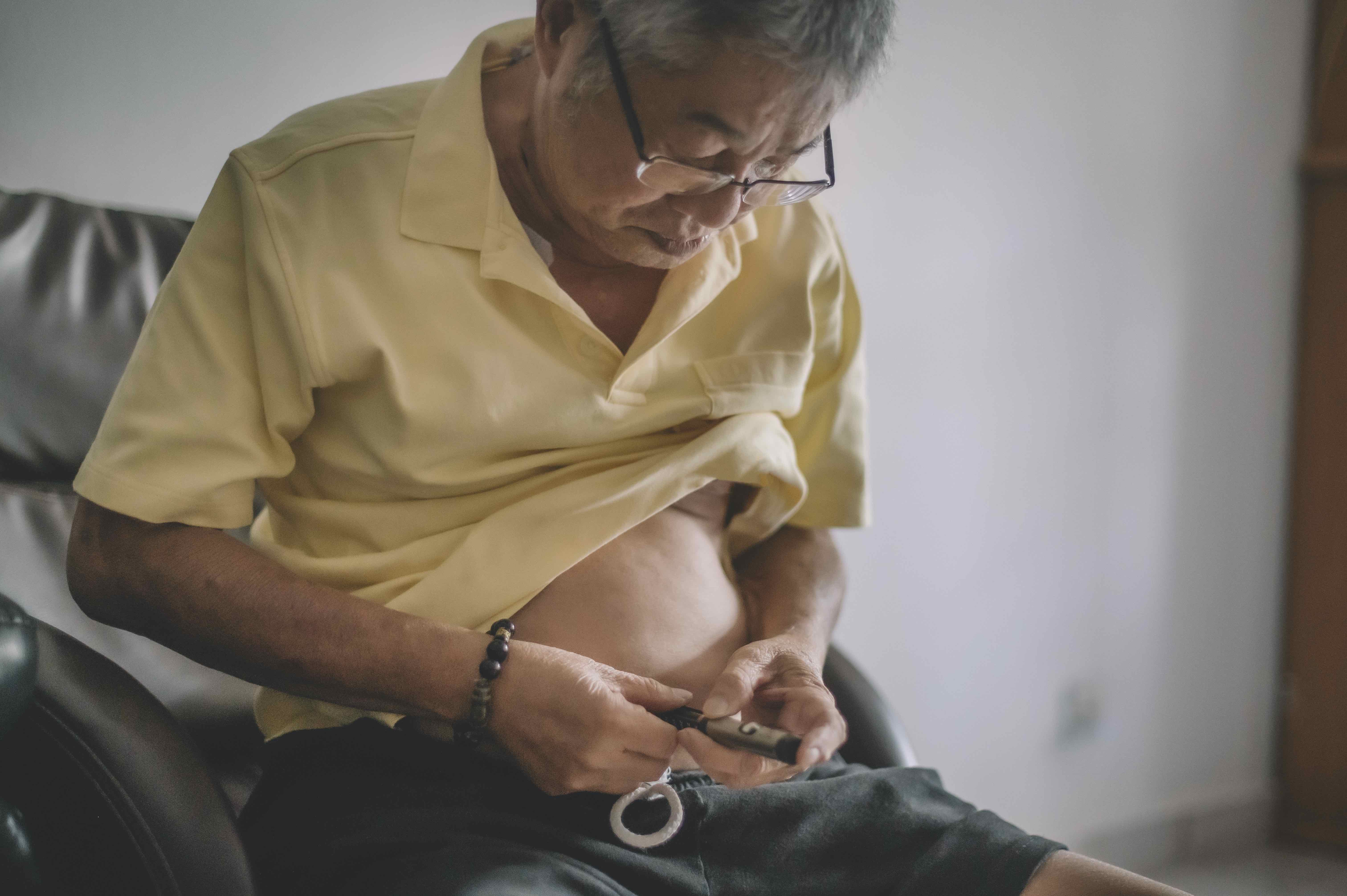
The study analysed data from 11,817 respondents from the three waves of the China Health and Retirement Longitudinal Study (CHARLS) conducted in 2011, 2013 and 2015. CHARLS uses a nationally representative sample of Chinese residents aged 45 and older.
Overall, 62 per cent of people had physical multimorbidity.
The burden increased with age, being female, higher per capita household expenditure and higher educational level. However, it was more common in poorer regions compared with the most affluent regions.
Health & Medicine
Is a delayed cancer diagnosis a consequence of COVID-19?
Lead author Dr Yang Zhao, a research scholar at University of Melbourne’s Nossal Institute for Global Health, says the cost of multimorbidity is difficult to quantify but is associated with higher health service use and greater financial burden for individuals and health systems.
“It is relatively difficult to precisely estimate the cost … particularly the indirect cost, like work productivity loss,” Dr Zhao says. “But there is no doubt that multimorbidity is costly to individuals, households and health systems.
“Among middle aged and older Chinese, patients with multimorbidity experienced higher incidence of catastrophic health expenditure than those individuals with a single disease (25.7 per cent vs 16.2 per cent) in 2015.”
The Chinese government is working towards universal health coverage by 2030. Around 1.2 billion people are covered by one of three social health insurance programs and community health centres are being developed with mixed results.

Low levels of service coverage for some and high out-of-pocket costs have raised concerns about the lack of adequate financial protection for patients with NCDs.
“Our findings provide new evidence to inform the development of targeted policies and interventions,” Dr Zhao says.
“Health systems in China need to shift from single-disease models to new modes of financing and service delivery to more effectively manage multimorbidity.”
Part of the challenge is reducing health inequity in a country with the world’s largest ageing population. Dr Zhao says reforms should reduce those inequalities and include targeted policies, lower out of pocket costs and new multimorbidity treatment guidelines.

Health & Medicine
Lessons for a future pandemic
“Strong primary health care, underpinned by multidisciplinary teams, is essential for cost-effective management of multimorbidity,” he says.
COVID-19 further complicates the situation. Dr Zhao says a national effort coordinated by the Chinese government has helped to contain its spread.
He says some evidence suggests that those with multimorbidity are more susceptible to COVID-19 and more likely to be at risk of severe cases and poor outcomes.
However, the impact is temporary.
“The Chinese government has made unprecedented efforts and invested enormous resources and these containment efforts have stemmed the spread of the disease,” he says. “During the lockdown of Hubei province, the central government’s coordination and joint efforts ensured ample supplies of major daily necessities.”

Meanwhile, there is much work to be done on public health in China generally.
Co-author and Harvard University Professor of Global Health Systems, Professor Rifat Atun, says the magnitude of multimorbidity in those aged 50 and over is striking.
“The rapid rise in multimorbidity is as a result of a combination of factors – rapid demographic and epidemiological transition along with changes in lifestyles and nutrition that has swiftly led to a large burden of chronic illness,” he says.

Politics & Society
Efficacy, ideology and COVIDSafe
“The economic impact is higher in lower income groups and those living in poorer rural areas who risk impoverishment as they aren’t financially well protected against illness and multimorbidity.
“This poses major challenges to China’s health system as multimorbidity leads to higher use of health services, longer hospital stays and greater likelihood of catastrophic health expenditures forcing citizens into impoverishment.”
University of Melbourne Nossal Institute for Global Health senior lecturer and senior author, Dr John Tayu Lee, says regardless of how COVID-19 plays out, chronic conditions will remain a major contributor to China’s health burden, health inequalities and its economic burden.
And this, he says, is likely to increase rapidly with an ageing population and high levels of NCD risk factors.
“Disease-specific guidelines are inadequate for the effective management of individuals with multimorbidity and new clinical guidelines for multimorbidity are needed.”
The study involved the Nossal Institute for Global Health, the University of Melbourne, WHO Collaborating Centre on Implementation Research for Prevention and Control of Noncommunicable Diseases, the George Institute for Global Health at Peking University Health Science Center, Harvard University, Duke University, University of Edinburgh, London School of Hygiene and Tropical Medicine, National University of Singapore and Imperial College London.
Banner: Getty Images