Health & Medicine
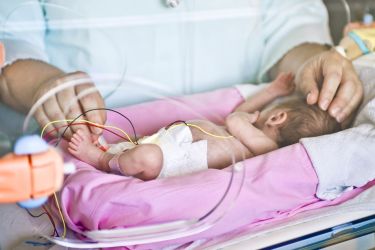
How every day counts for pre-term babies

Iron supplements may be the answer to tackling anaemia in poorer countries. Now major trials, including new intravenous treatments, will test the evidence
Published 8 January 2019
The World Health Organization (WHO) estimates that about four in every 10 young children around the world – that’s about 300 million kids – are anaemic.
In addition, three in 10 women – around half a billion – have anaemia, and this includes about 40 million pregnant women.

Anaemia is a critical public health problem, particularly in the developing world. WHO have set an ambitious target of halving the prevalence of anaemia in women by the year 2025, however, there has been almost no progress towards achieving this target.
Researchers from the Walter and Eliza Hall Institute and the University of Melbourne have partnered with the International Centre for Diarrhoeal Diseases Research (icddr,b) in Bangladesh and the University of Malawi College of Medicine to launch three large trials.
They will test the benefits and risks of iron interventions for young children in low income countries and test the impact of a single intravenous iron treatment for anaemic pregnant women.

Health & Medicine
How every day counts for pre-term babies
TREATING ANAEMIA GLOBALLY
A person is anaemic when levels of haemoglobin, the protein that turns our blood red, drop.
Since haemoglobin is the molecule that transports oxygen around our body, anaemia can leave people feeling weak or lethargic, and it has been said to contribute to reduced brain development in children.
The complications of anaemia seem to be most severe in pregnancy, having potential consequences for both mother and baby. Anaemic women are more likely to die in pregnancy, and their babies are more likely to be small or premature.
Preventing anaemia in babies is considered a critical intervention for improving child development and health outcomes. In order to tackle this, the WHO has recommended all children aged between the ages of six months to five years, living where the prevalence of anaemia is high, should receive iron supplementation or a newer form of iron called multiple micronutrient powders.

While these interventions are clearly effective in increasing blood haemoglobin concentrations, our systematic reviews and those of other researchers have found surprisingly little evidence that they improve critical functional child outcomes, such as cognitive development, wellbeing or growth.
WHAT WORKS AND WHAT DOESN’T
Importantly, several trials have generally been of questionable value. They may not have used a placebo in the control arm, which raises the concern that participants and people testing them knew which intervention they were receiving.
Trials may have had a small sample size, been conducted in populations that didn’t reflect the groups where the burden of illness lies, and children may have been pre-selected with baseline characteristics that don’t reflect the overall population; and they also may not have used the highest quality measures for health outcomes.

Health & Medicine
The vaccine saving the lives of Pacific children
Worryingly, some clinical trials in developing countries have found that iron, as supplements or micronutrient powders, may exacerbate the risk of infection.
A large trial in Tanzania where malaria is endemic, showed iron in young children increased the risk of hospitalisation or death, as well as malaria and infection-related outcomes.
Trials of iron containing micronutrient powders in Pakistan found they increased diarrhoea and in Ghana, a trial showed iron increased hospitalisation. Studies using cutting edge analysis of children’s intestinal microbiome to assess gut bacteria also suggest iron can re-profile bacterial make-up towards more dangerous and potentially pathogenic species.
IRON AND A CHILD’S HEALTH
In this context, the wisdom of giving universal iron interventions to children living in low-income countries where the prevalence of anaemia and infection is high is unclear.
It’s also hard to know whether to recommend micronutrient powders that are easy to give in food and allow other nutrients to be provided but are relatively expensive, or iron drops that are cheaper but perhaps less palatable.

Our Bangladesh trial opened in 2017 and has already recruited almost 3000 children. It allows us to understand the effects of iron on child health in a South Asian, non-malarious setting.
The Malawi trial, beginning in late 2018, will examine the effects of iron interventions in a malaria setting, and will also allow us to assess whether we can make iron interventions safe by co-administering malaria preventive medications.
These two Australian National Health and Medical Research Council (NHMRC) supported trials will collectively recruit over 5400 children and tell us whether giving iron interventions to young children can safely provide genuine benefits to their health and development.

Health & Medicine
How can heartburn end up as anaemia?
Further funding from NHMRC awarded in 2018 will enable us to undertake large-scale analysis of the intestinal microbiome in children enrolled in the trials, allowing us to use cutting-edge techniques (including deep sequencing) to understand the effects of the iron interventions on infant’s intestinal health.
IRON AND A MOTHER’S HEALTH
We know that iron supplementation in pregnancy improves maternal anaemia.
A recent trial in Kenya shows it increases neonatal birth weight by about 150 grams and reduces risk of prematurity. Two trials have also confirmed that during pregnancy, unlike in infants, iron doesn’t exacerbate the risk of clinical malaria.
But the main problem in sub-Saharan Africa is ensuring women receive a full course of iron.
Treatment programs in poorer settings are ineffective because they require multiple interactions between the woman and the health service over an extended period of time; finding ways to ensure pregnant women receive a full course of iron remains a critical challenge in global health.
With support from The Bill & Melinda Gates Foundation, we are trying an innovative approach to combat anaemia in pregnancy using new formulations of iron that can be given intravenously.
One such drug enables up to 1000 milligrams of iron to be given in a single 15-minute infusion. Compare this to a standard iron tablet containing 60-100 milligrams of elemental iron that is only 10 to 20 per cent absorbed.
This third trial, also in Malawi, tests the impact of a single intravenous iron treatment compared with oral iron tablets in 862 anaemic pregnant women. The trial will compare the mother’s anaemia at term, gestation duration, and baby birth weight.
The trial will also test for malaria in the mother and placenta. Additional funding from the Gates Foundation will allow us to follow up the babies for six months to see if there are long-term benefits from providing intravenous iron in pregnancy.
If we see benefits from intravenous iron compared with routine care, our trial will include detailed health economic analyses to establish the economic case for introducing this intervention to a low-income setting.
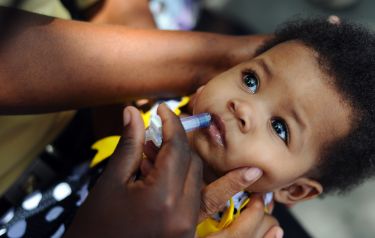
Health & Medicine
Vaccinating newborns against the deadly rotavirus
Our research program will recruit over 6000 children and mothers across Asia and Africa and will be one of the largest global efforts to address anaemia in pregnancy and understand the impact of iron on infant development.
Our trials are backed by almost A$11 million in government and international philanthropic funding. With collaborators from across WEHI; University of Melbourne; Monash University; University of Sydney, the ICDDR in Bangladesh; Malawi College of Medicine; Queen Mary University in the UK and the University of Bergen in Norway, our network aims to make an important contribution to addressing one of the biggest challenges facing women and children in under-served populations the world over.
Banner image: Shutterstock