Finance + Psychology: Finding a way to fight obesity

Researchers have used methods from finance and psychology to study the decision-making processes of lean and obese people
Published 25 July 2016
Obesity has long been regarded as a consequence of an individual’s poor decision-making in health, mainly the ones concerning dietary choices and physical activity.
It is a disease that has, since 1997, been recognised as a global epidemic by the World Health Organisation, and is a major health concern for many Australians, resulting in tremendous costs for the health care system and the economy each year.
Recently, research conducted at the Max Planck Institute for Human Cognitive and Brain Sciences (MPI CBS) in Leipzig, Germany, has highlighted that such altered dietary choices and exercise behaviours in obese people are directly related to differences in brain structure and function in regions critical for the control of eating behaviour, which are also responsible for reward-processing and decision-making in other domains of life.

Differences in decision-making
Could this imply that the differences in decision-making between obese people and healthy people are of a more general nature? To answer this question, we teamed up with biologist Dr Annette Horstmann at the MPI CBS in Leipzig. Together with medical doctorate student, Jakob Simmank, we conducted an experiment in which one group of obese participants (who were otherwise healthy) and a second group of healthy, lean control participants were asked to make a series of financial decisions.
These decisions involved trading off a small but immediately available reward against a larger reward that was only available in the future. This task is often used in decision-making research to probe a person’s level of impulsivity. When analysing the participants’ decision behaviours, we found that the obese participants showed a stronger preference for immediate rewards, implying a higher degree of impulsivity. Moreover, this higher rate of discounting of future rewards observed in the obese participants was directly related to their self-stated tendency towards opportunistic eating.
Having established these general differences in financial decision-making between the two groups, we then investigated whether the decision environment might also have a stronger influence on decision-making in obese people, compared to healthy people.
Economical impacts
If obesity was associated with individuals being more likely to be nudged into unhealthy lifestyle decisions, could this effect also be found when making financial choices? To answer this question, we added another layer to our financial decision-making task.
This time, both obese and lean participants were shown very positive, rewarding images before being asked to make the same financial decisions. Some of these images displayed desirable food, while others showed money, fancy boats and sports cars, positive social scenes, or romantic interactions, such as people kissing.
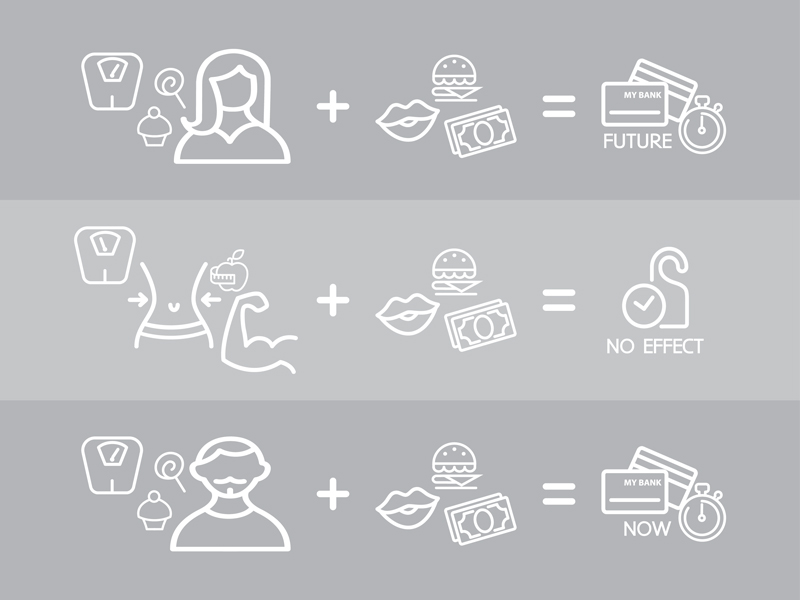
We found that after exposure to images of food and positive social scenes, obese women’s financial choices tended to be more future-oriented – that is, less impulsive – while obese men’s financial choices were more present-oriented.
No such effects were found in the lean, healthy control participants. Taken together, our study demonstrated that the specific decision environment did have an impact on obese people’s financial decision-making – this is particularly remarkable because the images were topically unrelated to the decisions our participants were asked to make.
This means that people who are obese were observed to be more susceptible to environmental cues. Consequently, these findings demonstrate that a research focus on food-related decisions in obesity might be too narrow, and differences in health decisions could simply be just one aspect of more fundamental differences in decision-making processes in the brain.
An interdisciplinary approach

Many of the major problems that contemporary societies face require solutions that are results of combined, multiple academic disciplines. An interdisciplinary approach to research is therefore integral to understanding and tackling these problems, and researchers from different disciplines are increasingly working together to address these issues. In finance, research has already begun to utilise methods from neuroscience and psychology to study brain processes to better understand aspects of financial decision-making, such as risk-taking.
This interdisciplinary alliance can be equally productive when applied to gain a better understanding of health disorders that present abnormal decision-making processes as a core feature, such as obesity.
However, our study is the first of its type investigating the influence of environmental cues on financial decision-making in obese people, and requires replication and follow-up experiments to clarify the exact circumstances under which such effects can be expected.
Just as importantly, our results also do not imply causality: at this stage, we are reticent about whether the specific differences in decision-making that we observed play any role in developing or maintaining the disease, or whether they are a consequence of having lived with obesity for a long time.
If our results are confirmed in the future, then this knowledge could potentially be used to design specific, positive decision environments, which could help obese people, or people at risk of obesity, to make better and healthier decisions.
In our view, the most important implication arising from our study – as well as from other researchers’ work using similar approaches – is that combining tools from different disciplines, each of which appear to be so distinctive of the other, can provide us with novel perspectives on problems that the single disciplines alone might be inadequately equipped to solve.
Banner image: Shutterstock

