
Politics & Society
Is this the end of the “American Century”?

Preeclampsia is one of the most serious complications a mother-to-be can face – new research aims to develop an early-warning blood test for pregnant women at risk
Published 7 March 2021
Pregnancy is usually an exciting time in a woman’s life as she awaits the arrival of her baby. But there are a number of pregnancy complications that can occur throughout those nine months and can have serious consequences for both mother and baby.
Preeclampsia is one of the most serious complications a woman can face during pregnancy. Worldwide it affects three to eight per cent of all pregnancies, and sadly claims the lives of thousands of mothers and countless more babies each and every year.

Preeclampsia is not a new disease. In fact, it has been hypothesised about and investigated for more than two and half millennia.
In ancient Greece, Hypocrites first made the astute observation “...that in pregnancy, drowsiness and headache accompanied by convulsions is generally bad”.
Thankfully, since then, our understanding and capacity to diagnose preeclampsia has improved significantly.

Politics & Society
Is this the end of the “American Century”?
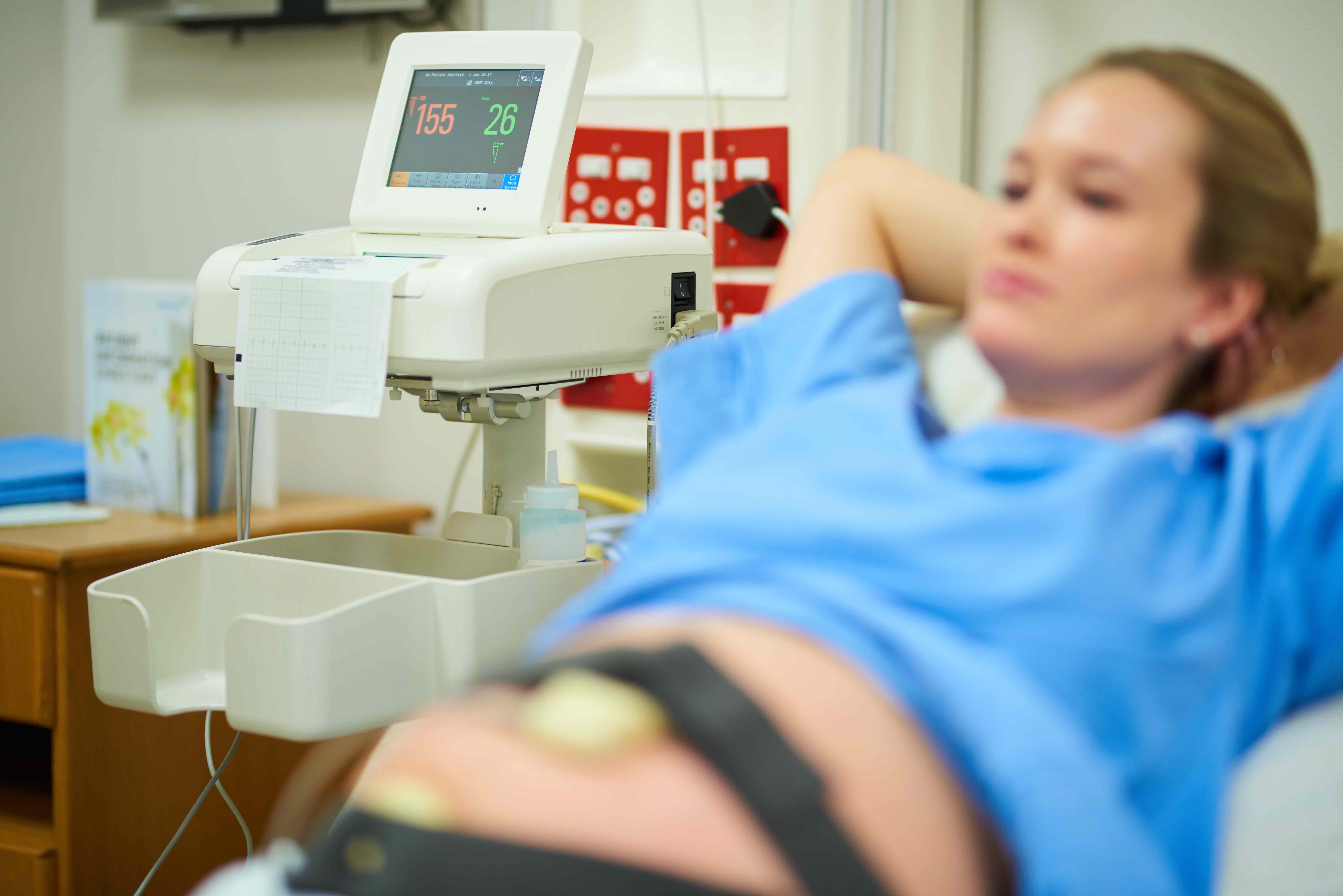
As any woman who has been pregnant will know, blood pressure checks are now standard practice at every pregnancy appointment. The reason is that elevated blood pressure is one of the tell-tale signs of preeclampsia.
Symptoms may include severe headaches or eyesight disturbances, increased fluid retention or swelling of the face or hands. It’s extremely important a pregnant woman seeks medical advice as soon as possible if she experiences these symptoms.
Over the last 20 years, the field has begun to clarify why preeclampsia occurs.
We know that it originates from the placenta; which in a healthy pregnancy represents the life-support system for a growing baby, transferring oxygen and nutrients. In preeclampsia, the placenta doesn’t set itself up properly, and so blood supply and oxygen to the baby is reduced.

As a result, the preeclamptic placenta releases toxins into the mother’s blood stream that cause damage to her blood vessels and organs – ultimately culminating in the clinical symptoms.
Unfortunately, to date, there are still no cures or treatments for preeclampsia. This means that when preeclampsia strikes, doctors and midwives must closely monitor women. Often they may need to deliver her baby very quickly (and sometimes early) to prevent any worsening of the disease.
But in the absence of any treatments or cures, research from around the world has shown us that identifying those at high risk and offering them personalised care can improve outcomes for both mothers and their babies.

Sciences & Technology
The importance of teaching boys about brilliant women
My team based in the Department of Obstetrics and Gynaecology at the Mercy Hospital for Women have recently received $A1.1 million grant from the NHMRC to develop new blood tests to better identify women at risk of preeclampsia.
Working with leading clinical scientists Professor Sue Walker, Dr Teresa MacDonald and Professor Stephen Tong, our goal is to develop a blood test that could be offered at the same time as the gestational diabetes test (at around 28 weeks of a pregnancy), to identify which women are at the greatest risk of developing preeclampsia.
If successful, this blood test could be offered universally to all pregnant women.
It would identify those at greatest risk before their symptoms occur. This would mean that doctors and midwives could increase surveillance in women identified as high risk, while reassuring low-risk women.
We are particularly focussed on identifying novel molecules that spill from the placenta into the mother’s bloodstream where we can measure them.
We have deliberately focused on placental molecules given prior research has already shown us that this is where the disease originates. We believe we are most likely to identify big changes in molecules spilling out of the preeclamptic placenta.
Our team also hopes that identifying novel molecules that are changed in women destined to develop preeclampsia will help further our understanding of exactly why preeclampsia develops.
This may help us to develop novel treatments for this disease and save the lives of more women around the world.
Banner: Getty Images