
Health & Medicine
The flu-hunters
New software based on statistical probability principles is helping forecast our flu season, and could also identify the level of threat of a bioterrorist attack
Published 13 February 2018
A forecasting tool that uses data routinely collected by state health departments could be used to forecast disease in the event of a bioterrorist attack or new influenza pandemic.
EpiFX, which was co-developed by researchers at the University of Melbourne and the Defence Science Technology (DST) Group, is already predicting the start and extent of the winter influenza season, sometimes up to weeks in advance. In the event of a pandemic, it can also be used to identify an appropriate response.

The collaboration has drawn the attention of the US Government’s Department of Defence, which is now working with researchers to develop a new tool to identify the level of threat from a bioterrorism attack and recommend appropriate response options.
James McCaw, Professor in Mathematical Biology at the University of Melbourne, has been at the forefront of infectious diseases modelling since its early days in Australia about 12 years ago, and leads the University’s EpiFX team.
“We have to start with what we know about these pathogens and how they might spread,” he says.

Health & Medicine
The flu-hunters
“When an outbreak occurs, either naturally or through an act of bioterrorism, the forecasting tool provides the crucial link between scenario planning, which has been conducted in preparation for future events, and real-time data analysis.
“That kicks in when people affected by the virus start to arrive at emergency departments, or when in a particular environment, such as a barracks, soldiers start displaying symptoms.
“Analysis of that data shows us how quickly a virus is spreading, and initiates an appropriate and proportionate response.”
In extreme cases, this could mean recommending the closure of schools or shutting down public transport to minimise opportunities for a virus to spread.
Dr Tony Lau, who leads DST Group’s epidemic detection and forecasting program, says the tool combines the concept of probability inference – which updates the probability of a hypothesis as more information becomes available – with susceptible, exposed, infected and recovered (SEIR) compartmental disease models.
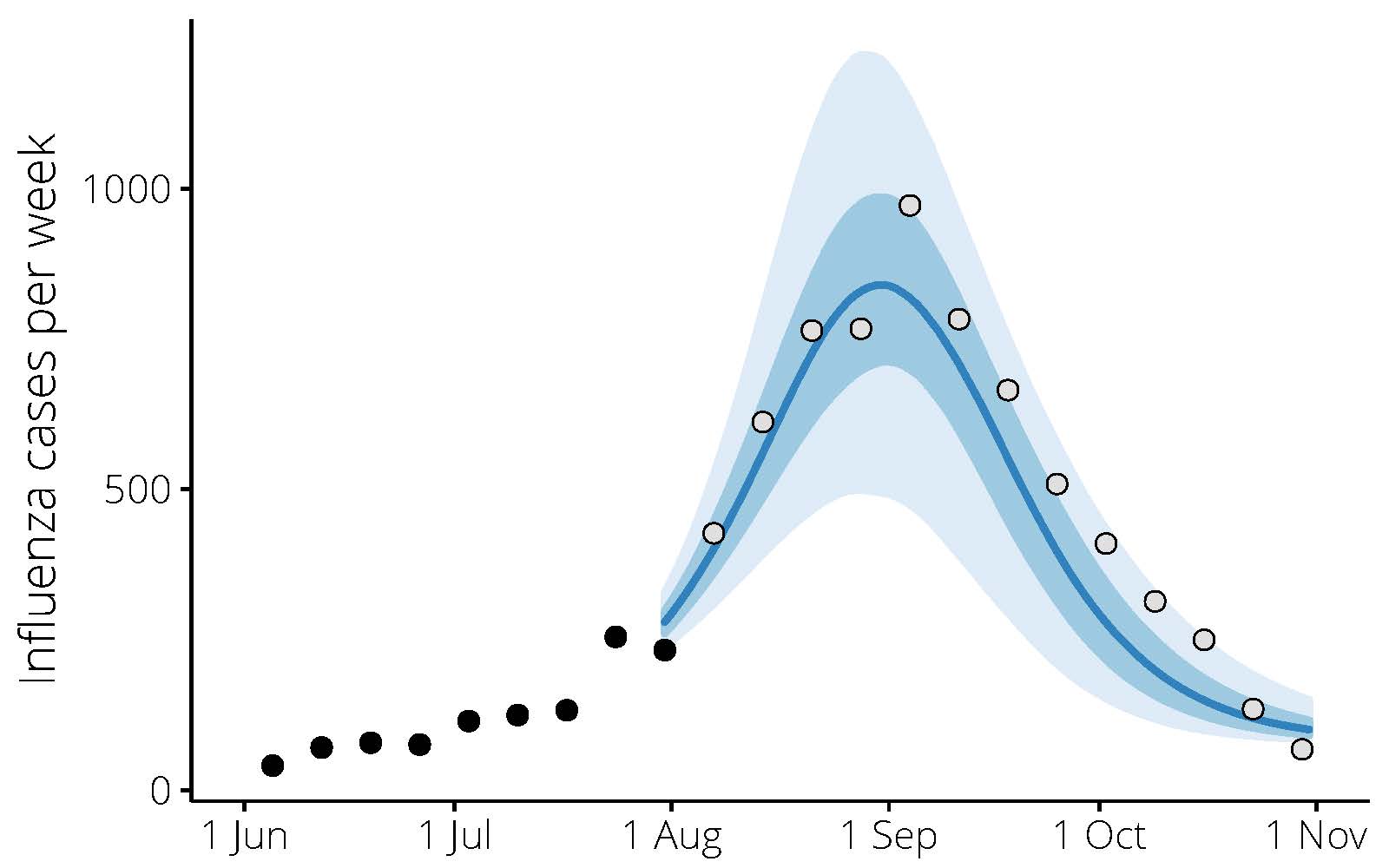
“This provides a mathematical framework for understanding the establishment and spread of infectious diseases,” he says.
This modelling can potentially predict how quickly an epidemic will spread, and identify those most at risk so preventive action can be taken through measures like targeted vaccination.
“In general, it is the young, the old and the weak who are most at risk from viruses like influenza,” says Dr Lau. “Better forecasting means we can use state or national resources more efficiently, with those people in mind.”
In Victoria, EpiFX has accurately predicted flu outbreaks up to five weeks in advance. Weekly forecasts of the incidence of flu are shared with the health sector to gain further insight into the influenza season and continue its refinement.
Health & Medicine
Vaccination: A numbers game that adds up
Despite early success, challenges remain.
The 2017 influenza season in Australia was severe, with an extreme case count recorded in many jurisdictions.
Dr Rob Moss, mathematical biologist at the University of Melbourne and EpiFX technical project lead, says the underlying causes for this increase are not yet understood but may stem in part from behavioural changes. “Our statistical tools are similar to those used to predict the weather, but we face the additional challenge of having to account for changes in human behaviours,” says Dr Moss.
“Individuals may change their health seeking behaviour based on media attention and general practitioners could have also changed their testing practices. We’ve only just started to scratch the surface in unpacking these complex interactions.”
This new tool being worked on with the US Government’s Department of Defence is a partnership between the DST Group, the University of Melbourne and the University of Adelaide.
Highly contagious diseases and viruses, like Ebola and influenza, as well as emerging diseases such as Zika, are being investigated as part of its development.

DST Group began working with the University of Melbourne research team on disease modelling in 2014. “We are still developing and refining our forecasting, but in the event of a health emergency, we are in a better position to respond than we have ever been, as we improve our ability to integrate forecasting with our scenario analyses,” says Professor McCaw.
The success of these forecasting tools involves a huge amount of collaboration from researchers and public servants working in fields including computer science, physics, mathematics, electronic and software engineering, epidemiology and medicine.
Health & Medicine
Stopping the flu virus at the nose
Other countries including the United Kingdom, South Korea and Singapore are interested in using the tool’s epidemic modelling capabilities.
This collaborative project between the DST Group and the University of Melbourne is made possible by ongoing assistance from, and engagement with, data custodians and public health staff. The active participation of three government branches – the Victorian Department of Health and Human Service’s Health Protection Branch, Health Protection NSW, and the Queensland Department of Health’s Communicable Diseases Branch – has been an essential part of this. We also thank the National influenza Surveillance Committee (NISC), a sub-committee of the Communicable Diseases Network Australia, and the NISC Secretariat of the Australian Government Department of Health for their input to this project.
Banner image: An influenza virus (orthomyxoviridae) seen through an electronic microscope/ Alain Grillet and Sanofi Pasteur, Flickr