Health & Medicine
The evolution of schizophrenia
Brain markers of sensory and motor function reflect disturbances in early development that can increase the risk of later psychosis
Published 3 May 2022
When a mental health professional uses the term psychosis, it describes a person’s loss of contact with reality.
Although only around three per cent of people will develop a psychotic episode at some point in their lives, it’s distressing, with so-called positive symptoms, including hallucinations, delusions (or false beliefs) and disorganised thinking (or illogical flow of thoughts).

More severe forms of psychosis, like schizophrenia, are also associated with so-called negative symptoms, including apathy, poverty of speech and blunted emotional responses.
These symptoms are called ‘positive’ and ‘negative’ because the ‘positive’ ones are changes in thoughts and feelings that are ‘added on’ to a person’s experiences – like paranoia – while the negative are those things that are ‘taken away’, like motivation.
These psychotic conditions can also be associated with abnormalities of motor function – catatonia being the most extreme.

Health & Medicine
The evolution of schizophrenia
Psychotic disorders are most common in young people during late adolescence and early adulthood. And if left untreated, psychosis can be persistent, impacting a person’s ability to function in everyday life.
Because of the potential for psychosis to cause life-long problems, it’s important to identify who could develop psychosis as early as possible and to understand its causes. While it’s still not well understood, researchers believe psychosis likely involves a combination of genetic and environmental factors that disrupt the development of the brain in early life and during adolescence.
This is called the neurodevelopmental hypothesis. So markers that indicate a possible deviation from normal brain development may help to provide important early signs of later psychosis.

Our recently published study examines this possibility by assessing subtle abnormalities of motor and sensory function in a group of young people at high risk for psychosis, in order to explore if they might indicate abnormal neural development in early life.
The Clinical High-Risk (CHR) state is a term that describes the clinical features and symptoms that increase an individual’s risk of developing psychosis.
Health & Medicine
Grasping COVID-19’s long neurological tail
A person can be classified as at risk if they meet certain criteria – like having mild psychotic symptoms that are distressing, as well as a decline in their day-to-day functioning.
While this does not mean that a person will definitely develop a psychotic episode, the risk is increased so that between 10 and 35 per cent of these people will develop a psychotic condition.
The CHR framework is valuable for providing insight into pre-existing factors of psychosis or factors associated with the lead up to psychosis. The lead up to psychosis is known as the prodrome – the early signs or symptoms of an illness or health problem that appear before the major signs or symptoms start.
The sensorimotor system is part of our body’s motor control system, involved in processing sensory and motor information.
Dysfunctions in the sensorimotor system include subtle neurological abnormalities called neurological soft signs, or NSS. These can include diverse and subtle abnormalities in sensory integration, motor coordination, the sequencing of complex motor tasks and basic reflexes.
Abnormalities like this are thought to have their basis in early development when the motor system is maturing most rapidly compared with other systems (like our cognitive or thinking systems).
Previous studies have found higher NSS in people who have schizophrenia, as well as relatives of people with schizophrenia but who do not have the condition themselves.
Health & Medicine
Brain development is altered in people at high risk of psychosis
However, less is known about people identified to be at CHR.
It’s important to know if NSS are present at the CHR stage, and, if so, whether it’s in all people who are at risk of psychosis or only those who later go on to develop a fully-fledged psychotic illness, like schizophrenia.
Our study aims to do just this.
Our research consisted of 56 young people meeting CHR who had never been treated with antipsychotic medication alongside 35 healthy controls. All participants were assessed for the presence and intensity of NSS and underwent a brain scan for measurement of their brain volume.

What’s unique about our study is that the CHR participants had been followed up for an average of five years to determine their health status. Twenty-five of these young people at CHR later transitioned to psychosis (CHR-T) in the follow-up period and 31 did not (CHR-NT).
We found higher NSS in the CHR group overall, irrespective of whether they later developed psychosis. NSS were higher in nearly all areas of sensory and motor function except motor coordination.
When we compared the two groups of CHR to controls, we also found higher NSS in the group that later transitioned to psychosis (CHR-T), but not in those who didn’t (CHR-NT).
Health & Medicine
Schizophrenia: Mapping how the brain changes
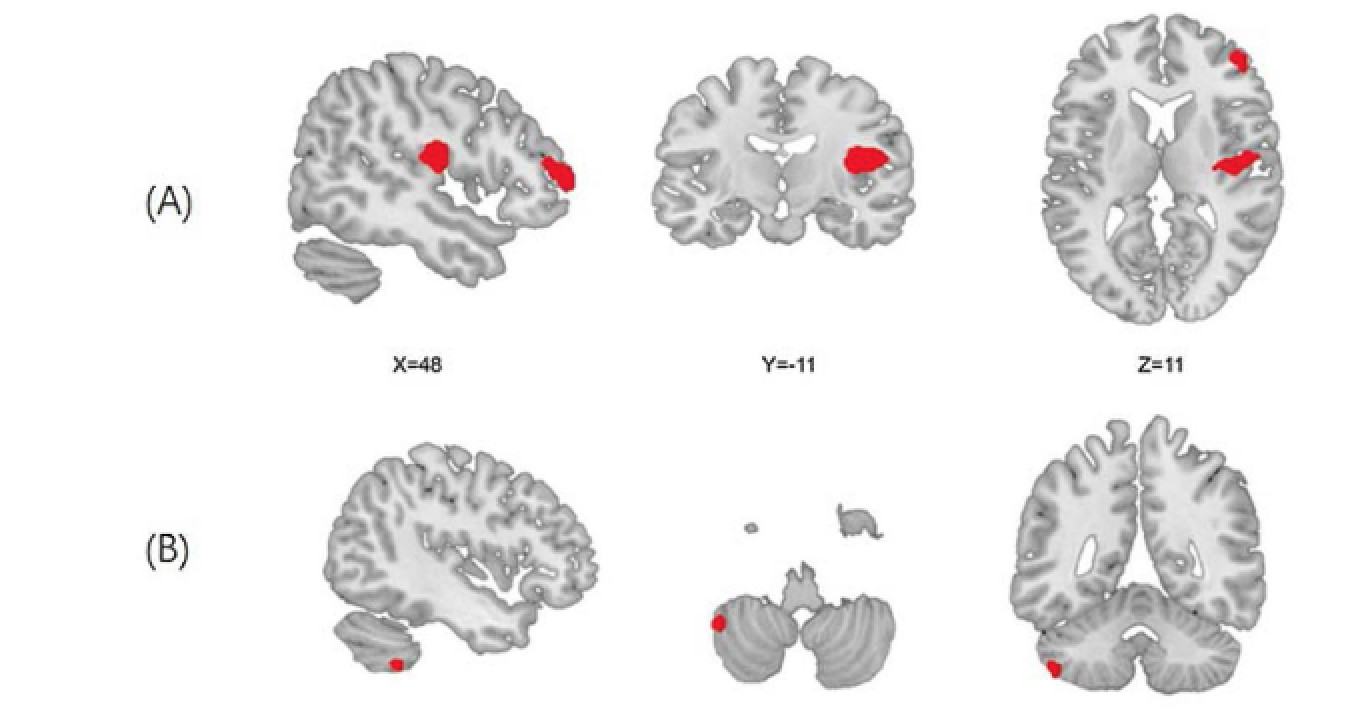
When looking at the brain scans, deficits in processing and interpreting sensory information (like touch) in people who developed psychosis were linked to lower grey matter volume in parts of the cerebellum, insula and frontal gyrus; these are the brain regions involved in our motor, sensory and cognitive processes.
Our findings indicate that minor sensorimotor abnormalities and corresponding brain changes are apparent prior to the development of full-threshold psychosis.
Importantly, because all of the CHR individuals were examined before any one of them developed psychosis, these findings cannot be simply explained by factors that may influence these results after diagnosis of a psychotic disorder – including antipsychotic treatments that have been shown to affect motor function.
It’s not clear yet whether the assessment of NSS could assist clinicians in identifying who will more likely develop a fully-fledged psychotic illness; our results need to be replicated in a larger study.

But what is clear from our study is that formal assessment of sensorimotor disturbances can help a clinician evaluate young people who may be at risk of psychosis. Information like this becomes valuable in helping a young person find appropriate clinical services and when considering strategies to reduce other potential risk factors for psychosis.
Early recognition might also open up alternative treatment options.
Novel ways of measuring motor and sensory disturbances with wearable technology and treatment with brain stimulation are also being developed and trialled in people with established schizophrenia.
Health & Medicine
Mapping how schizophrenia changes brains
Our findings do not indicate that NSS are exclusive to the development of psychosis. NSS did not differ between those who did and did not transition to psychosis, meaning that there’s a lot of variability in these signs in people at risk of psychosis.
Because studies have also found minor neurological disturbances in other disorders including autism, the presence of NSS might be an indicator of increased vulnerability for mental illnesses including psychotic disorders but, by themselves, might not predict transition.
Our findings are consistent – but do not prove – the neurodevelopmental theory that links disturbances of normal brain development in psychosis. It also suggests that we should be looking for sensorimotor disturbances earlier than CHR – potentially in childhood.
Our group is now comprehensively mapping sensorimotor processes over time in children with psychotic-like experiences.
This will help us to understand the developmental trajectory of sensorimotor function in children and adolescents – and as potential vulnerability markers for those at risk of psychosis.
Banner: Getty Images