
Business & Economics
What’s keeping women out of work?
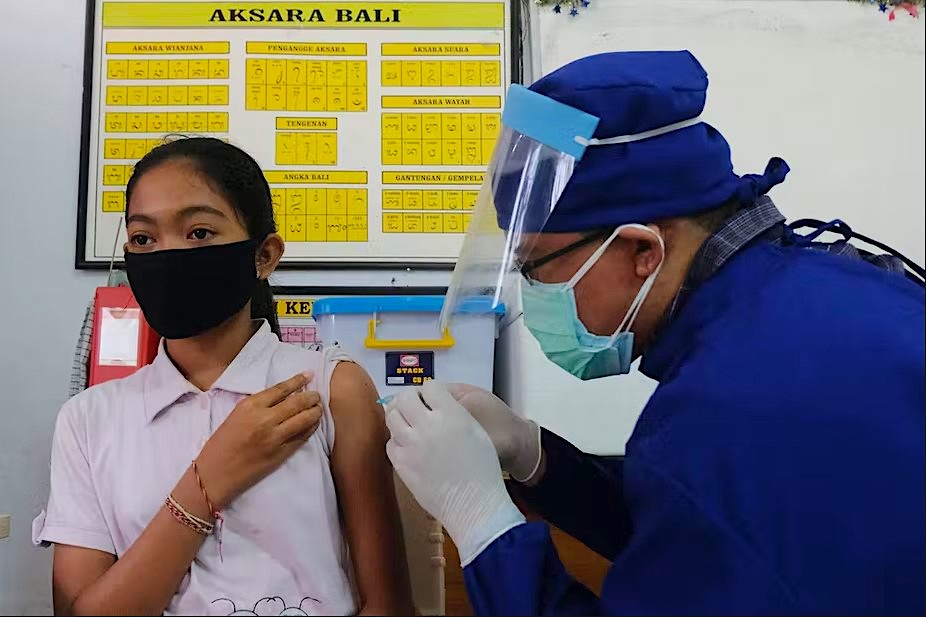
Indonesia is rolling out a free Human Papillomavirus (HPV) vaccine nationwide to protect women and girls from cervical cancer
Published 29 April 2022
In April, Indonesian Health Minister Budi Gunadi Sadikin announced that his ministry was adding the Human Papillomavirus (HPV) vaccine to the list of routine free immunisations administered nationwide.
This represents a huge leap forward for Indonesia’s commitment to cancer control and the sexual and reproductive health of women and girls.

The plan to roll out free HPV vaccination for girls enrolled in grades 5 and 6 of secondary school follows the success of a national HPV demonstration program first introduced in 2017.
HPV is understood as a “necessary cause” of cervical cancer – the virus is present in more than 90 per cent of cases. There is very high prevalence of HPV among sexually active individuals both globally and in Indonesia.
In fact, Indonesia has experienced a rise in the number of women developing cervical cancer over the past decade, with about 32,000 new diagnoses annually.

Business & Economics
What’s keeping women out of work?
The mortality rate for Indonesian women affected by cervical cancer is now exceedingly high, mainly because low screening rates mean that diagnosis typically occurs in the later stages of disease.
At least 50 Indonesian women are estimated to die each day from cervical cancer, representing more than half of all Indonesian women diagnosed.
Because cervical cancer is preventable by HPV vaccination prior to sexual debut, Indonesia’s commitment to the free provision of this vaccine for girls will inevitably save millions of lives.
The HPV vaccination demonstration program was initiated in five of Indonesia’s 34 provinces, with funding from Gavi (previously known as the Global Alliance for Vaccines and Immunisation). The program provided two free doses of the HPV vaccine to girls enrolled in secondary school, typically aged between 10 and 12 years old.

Program evaluations and independent research, including by Nossal Institute for Global Health PhD candidate Setiyanti Marta Dewi, have been promising.
The HPV vaccine received high public acceptance in all participating regions. Vaccine uptake and completion rates were more than 90 per cent, and no severe adverse reactions were recorded among vaccine recipients, confirming the safety of the HPV vaccine for adolescents.
Independent research by non-Indonesian government researchers has also looked into the experiences of girls who have been vaccinated in the program and their mothers or female guardians.

Arts & Culture
How women are changing Indonesia
Dewi’s PhD research, for example, found high rates of satisfaction, as indicated by a willingness to recommend HPV vaccination to other mothers or adolescent peers.
There will always be some degree of vaccine hesitancy in any society, and there will always be missed doses in school-based programs because of interruptions to school attendance. However, an uptake and completion rate of 90 per cent makes the program an undoubted success.
Since the pilot program began, cancer and sexual and reproductive health advocates have campaigned for its expansion and inclusion of the HPV vaccine in the National Immunisation Program.

Advocates have made official submissions to the Ministry of Health detailing the need to expand the scale of the program. They have also held public events, and engaged in widespread advocacy on social and traditional media, like radio and television.
Leading this advocacy has been the Indonesian Coalition for Cervical Cancer Prevention (KICKS), established by the Indonesian Society of Gynaecologic Oncology (INASGO) in 2017.
Other organisations involved in this nation-wide coalition include: the Indonesian Working Group on HPV (IWG-HPV), the Indonesian Cancer Foundation (YKI), the Cervical Cancer Care Foundation (YPKS), the Women’s Health Foundation (YKP), the Miss Indonesia Foundation, women’s rights organisation Kalyanamitra, and Islamic organisations that advocate for women’s rights, such as Fatayat Nahdlatul Ulama.

Politics & Society
Reversing Indonesia’s child marriage laws
The diversity of organisational support and expertise represented within the KICKS coalition highlights how widely the cause of cervical cancer control has been taken up. It also demonstrates how effective sustained civil society action can be in forcing the hand of governments towards action.
Advocacy has been particularly important during the COVID-19 pandemic, which led to widespread reallocation of funds and medical personnel away from preventative services toward the pandemic response.
Since 2020, KICKS has sustained pressure on the Ministry of Health to ensure that disruptions to cancer control programs caused by the COVID-19 pandemic did not result in long-term delays in returning cervical cancer screening services to normal operating conditions, or prevent the expansion of the HPV vaccination program across the country.

Research on the readiness of Indonesian communities for the uptake of the HPV vaccine suggests a range of strategies will enhance the success of the program.
First, it will be key to educate parents, both women and men, on the benefits of the vaccine for their daughters, as young adolescents are unable to give independent legal consent to participate. This makes parental consent paramount to the program’s success.

Health & Medicine
Midwives on the COVID-19 frontline in Indonesia
Second, education materials need to deal directly with myths surrounding HPV, the vaccine and cervical cancer, and provide correct information.
Myths can include false beliefs such as: the vaccine is haram; it may cause promiscuity; it has severe side effects; or that only promiscuous women can develop cervical cancer. Such myths could compromise the public’s confidence in the program and need to refuted with sound scientific evidence.
Third, it will be important to ensure that the vaccine remains free and is available through schools, which are trusted social institutions. Prior studies have shown reluctance to pay for the vaccine among low-income families.
Fourth, there needs to be clear messaging that two doses are required to fully protect girls from contracting HPV.

A dedicated program to reach adolescent girls who have missed doses, and those who don’t attend school, also needs to be rolled out nationally to ensure equity of access. Catch-up services are already available in some highly resourced puskesmas (primary health clinics) in urban areas – but rollout of catch-up doses needs to reach regional areas and hard-to-reach groups.
Finally, the administration of the vaccine through schools represents an excellent opportunity for cancer prevention education to be integrated into the school health curriculum.
It should be expanded to include prevention and a lifelong approach to sexual and reproductive health that begins in childhood/early adolescence.
Health & Medicine
Vaccinating newborns against the deadly rotavirus
Indonesia’s commitment to upscaling free HPV vaccination for girls enrolled in secondary school is a major milestone for young Indonesian women, and will have lifelong benefits for them.
However, the lack of access to high quality, free cervical cancer screening for older women (who are sexually active and likely to have already been exposed to HPV) remains of great concern.
It too will require continued advocacy and greater investment from the government in the years ahead.
This article was republished from the Indonesia at Melbourne blog.
Banner: A student receives an HPV vaccination in Bali in 2020/ Photo by Nyoman Hendra Wibowo for Antara.