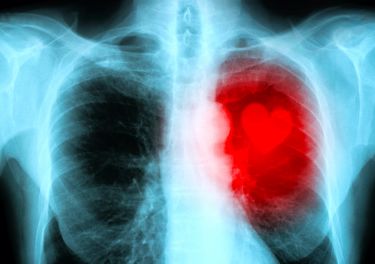
More than a high BMI, an ‘obese heart’ is a silent risk

New research shows that fat tissue around the heart releases molecules that alter heart rhythm, identifying potential new targets for preventative therapies for heart disease
Published 24 September 2020
More than two thirds of Australians are now overweight or obese.
More than just a statistic, this figure is concerning because obesity is associated with a number of long-term health issues including diabetes, cardiovascular disease, some cancers, musculoskeletal disease, disability and has recently emerged as a risk factor in COVID-19 morbidity.

Of these, heart disease is Australia’s biggest killer. And irregular heart rhythms, known as atrial fibrillation (AF), are an early phase of heart disease, which can lead to stroke, heart failure and, eventually, death.
AF is also associated with accelerated dementia and depression.

In Australia, one in 11 deaths are linked to atrial fibrillation with an economic cost of more than $A1.25 billion per year. Described as a ‘silent killer’, many people with AF have no symptoms and it is often difficult to diagnose.
It has been known for some time that obesity is a critical risk factor for AF. Each unit increase in body mass index (BMI) increases AF risk by four to five per cent.
So, developing new preventative therapies for treating AF is crucial to reducing the public health and economic burden of this disease.
Our latest study published in the Journal of the American College of Cardiology has highlighted that the build-up of fat around the heart is especially dangerous for heart health – showing a link between the fat deposit on the surface of the heart muscle with atrial fibrillation.
Silent progression to heart failure
The Framingham Heart Study first identified an important, but poorly understood link between accumulation of fat around the heart and the risk of the most common form of irregular heart rhythms – atrial fibrillation.
This then culminated in a new collaboration, between pre-clinical researchers and clinical cardiologists at the University of Melbourne and Melbourne Biomedical Precinct.
Health & Medicine
World-first test could predict your risk of a heart attack
Our group has been researching the role of cardiac adipose (fat tissue) in regulating heart muscle contraction and heart pump function for a number of years.
And our partners, Drs Jon Kalman and Chrishan Nalliah’s team from the Department of Medicine at the Royal Melbourne Hospital, have been investigating the effects of patient obesity on the electrical abnormalities which provoke AF.
During the project, while patients were still undergoing surgery, we could rush heart tissue fragments (removed as part of the surgical process) into the research lab and work on them immediately.
The most common irregular rhythms of the upper chambers of the heart - atrial fibrillation - are more prevalent in aged and obese populations. One in three people will develop AF beyond the age of 55 – and the risk accelerates with increasing age.
People are often unaware they have AF – and the first sign could be tragic: a stroke due to blood clot traveling to the brain or the danger of a sudden blackout with dire consequences.
Silent progression to heart failure is common, with AF only detected when the symptoms of heart failure emerge.

Health & Medicine
Q&A: A new way to treat type 2 diabetes?
Changes in heart rhythms
Most people don’t realise that there is a lot of fat – adipose tissue – around the heart muscle. In extreme cases the amount of fat has been found to be up to 50 per cent of the entire heart weight.
Our research has shown that the adipose tissue around the heart produces biochemical factors which changes the way electrical signals move through the heart muscle tissue to generate the heartbeat.
The cell-to-cell communication is disrupted, and the transfer of the electrical signal between cells (which creates the heart beat) is delayed. These factors have a potentially major role in causing disruption of electrical activity which underlies atrial fibrillation.
And although BMI increases the risk of AF, it is the cardiac adipose burden (and not BMI) that is most important in electrical and structural disruption.

There are no general screening processes, no preventative treatments and AF and AF complications are associated with hospitalisation rates of up to 40 per cent.
It is also likely that AF is under-diagnosed in women.
Health & Medicine
Different fat cell types may be key to obesity
Men often undergo cardiac surgery to unblock coronary arteries where AF is then often detected. Heart disease with major artery involvement is much less common in women, so AF often remains undetected until the disease is dangerously advanced.
Potential new treatments
Understanding the basic causes, early intervention and developing new preventative therapies is crucial.
Current treatments for those diagnosed with AF are limited and lack effectiveness. They are designed to abolish the irregular heart rhythms without addressing the underlying cellular causes.
Drug therapies can actually make arrhythmias worse and the common atrial ablation catheter procedure only works for a limited time and repeat procedures are common.

By showing that the fat around the heart drives these rhythm irregularities, our study identifies potential new targets for developing preventative therapies that may reduce the catastrophic health consequences.

Health & Medicine
Empowering everyone to improve their own health
Our research suggests that more proactive management to measure the heart adipose load should be undertaken as part of a risk assessment.
It also raises the possibility that a surgical approach to reduce cardiac adipose (fat) tissue could be an intervention to consider in future and identifies molecular signalling which may potentially pave the way for targeted drug treatment.
A link to living in a time of covid-19?
Obesity has emerged as a major risk factor for morbidity in COVID-19 patients, with cardiovascular complications a major underlying cause of death.
The causes underlying this are poorly understood. It is possible that the fat surrounding the heart is implicated.
Our study shows that factors released from the heart can have potentially catastrophic effects on how the heart muscle functions – but the extent to which this underlies the cardiovascular component of COVID-19 mortality or morbidity has yet to be further explored.
Research support for this work was provided by the National Health and Medical Research Council.
Banner: Getty Images
