
Health & Medicine
The long-term benefits of controlling your asthma
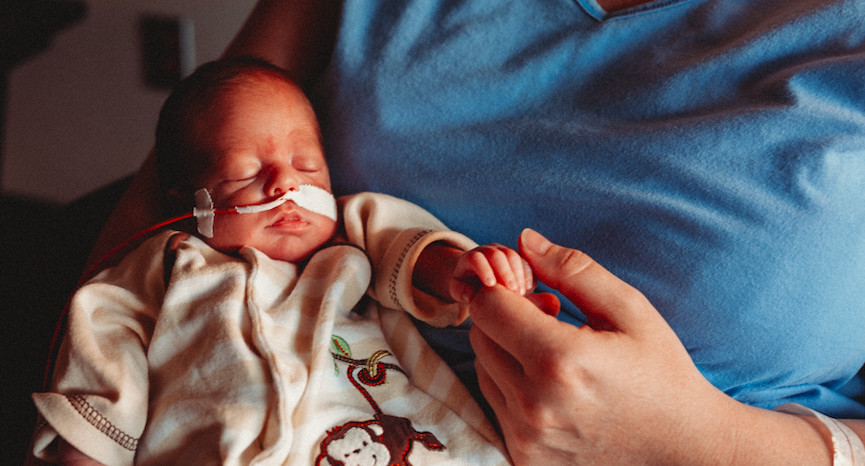
New research shows a link between premature birth and obstructive lung disease after age 50, highlighting opportunities for reducing risk factors like smoking in people born preterm
Published 20 February 2022
A few decades ago, researchers began noticing that as the number of premature births increased, so did the number of cases of a serious lung condition in 50 to 60-year-olds.
Known as chronic obstructive pulmonary disease, COPD is a chronic inflammatory lung disease that causes obstructed or reduced airflow from the lungs. Symptoms can include difficulty in breathing, shortness of breath on exertion, coughing, excess mucus (sputum) production and wheezing.

COPD is typically caused by long-term exposure to irritating gases or particulate matter, often from cigarette smoke. Emphysema and chronic bronchitis are the two most common conditions that contribute to COPD.

Health & Medicine
The long-term benefits of controlling your asthma
People with COPD are also at increased risk of developing heart disease, lung cancer and a variety of other conditions.
COPD is currently the third leading cause of death, contributing to over three million deaths annually worldwide. By 2030, it is projected to cause/lead to over 4.5 million deaths annually.
In parallel to this increase in COPD, a systematic data review published in 2019, showed that the rate of preterm birth increased from 9.8 per cent in 2000 to 10.6 per cent in 2014 globally.
To understand if increases in premature birth were linked with increasing COPD, our research team analysed data compiled over six decades from 1445 participants from the Tasmanian Longitudinal Health Study (TAHS) who were born in 1961.
TAHS started in 1968, recruiting all students aged seven in Tasmania, and has regularly followed participants to their sixth decade. We used TAHS in this study as it is now one of the world’s longest and largest ongoing respiratory studies.

Specifically, we compared data on gestational age from hospital records and parent reports with lung function measured at 53 years. Gestational ages were categorised as: very preterm (28 weeks to less than 32 weeks), moderate preterm (32 weeks to less than 34 weeks), late preterm (34 to less than 37 weeks) and term (at or over 37 weeks).
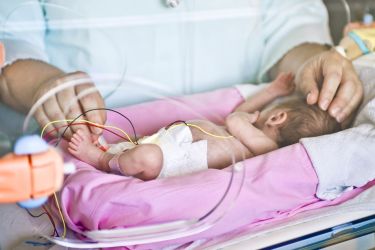
Health & Medicine
How every day counts for pre-term babies
COPD was defined based on post-bronchodilator spirometry, which is a breathing test that measures how effectively and quickly the air in the lungs can be emptied by measuring lung volumes during breathing.
We found that compared to term, very to moderate preterm birth was associated with a 2.9-fold increase in the risk of COPD development.
Those born prematurely (very to moderate preterm) also had reduced lung function measures, suggesting that prematurity may affect the development of both small and large airways.
This study is the first to show that being born prematurely is a risk factor for COPD that can become apparent in later mid-adult life.
Not only very preterm but moderate preterm survivors may also suffer from increased risk obstructive lung function deficits and COPD at age 53 years.

Importantly, we also found that the impact of preterm birth on impaired lung function at 53 years of age was stronger among smokers. In other words, lung function deficits in relation to preterm birth were much greater if individuals were smokers as adults, highlighting an opportunity for early education interventions.

Health & Medicine
The impact of air pollution on life expectancy
Because lung development commences during the intrauterine period with the completion of substantial structural development by term, being born early may shorten the time for full lung development.
Such impairment during the development phase may persist and have a long-term impact on its own. Moreover, such impairment may make survivors more susceptible to the harmful impact of later-life exposures like smoking, air pollution or occupational exposures.
Our findings highlight important public health issues, but also an opportunity to address them.
Preterm births are increasing due to advances in perinatal medicine and this is likely to impose an increasing burden on the health system globally as larger numbers of preterm survivors reach their 50s and 60s in coming decades.
Our findings also indicate the importance of prenatal and perinatal care and interventions to reduce the rate of preterm birth, which may have multiple health benefits apart from lung health.

We also see this as an opportunity to reduce the burden of COPD associated with preterm birth by encouraging smoking avoidance in preterm survivors through targeted health education in this high-risk group.
Our next research project will focus on modifiable factors that can reduce the risk of lung function impairment and COPD in preterm born survivors, to develop and evaluate potential interventions. These may include measures to reduce exposures to air pollution and occupational hazards.
We also aim to incorporate lifetime risk factors including birth characteristics to develop a comprehensive prediction tool for COPD. Being able to reduce risk factors earlier will allow more of us to live a longer, as well as a healthier life.
The recently published study was conducted by a research team at the Allergy and Lung Health Unit, Centre for Biostatistics, Melbourne School of Population and Global Health, led by Dr Dinh Bui, Dr Jennifer Perret, Associate Professor Adrian Lowe, Associate Professor Caroline Lodge and Professor Shyamali Dharmage.
Banner: Getty Images