Health & Medicine
Breathing easy: Treating steroid resistant asthmatics
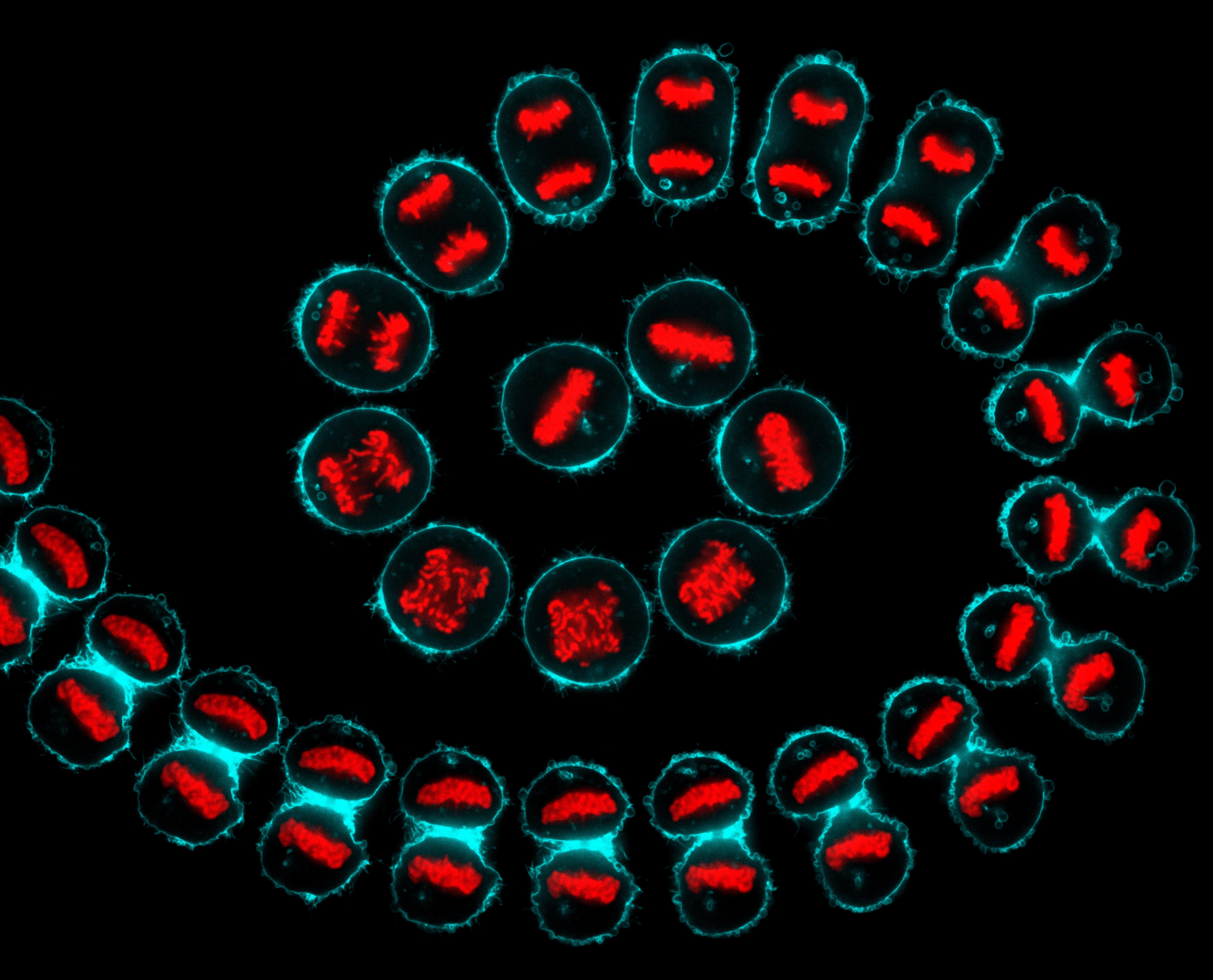
Researchers have uncovered a whole new class of drug compounds with the potential to completely stop the proliferation of specific cancers like leukaemia and liver cancer, and maybe help keep other cancers in remission
Published 2 August 2018
How our cells proliferate from a single egg cell into a precisely formed human composed of trillions of cells is a stupendous feat of genetic regulation.
But it also contains the seeds of cancer when the controls are lost and these cancerous cells can proliferate relentlessly into tumours.
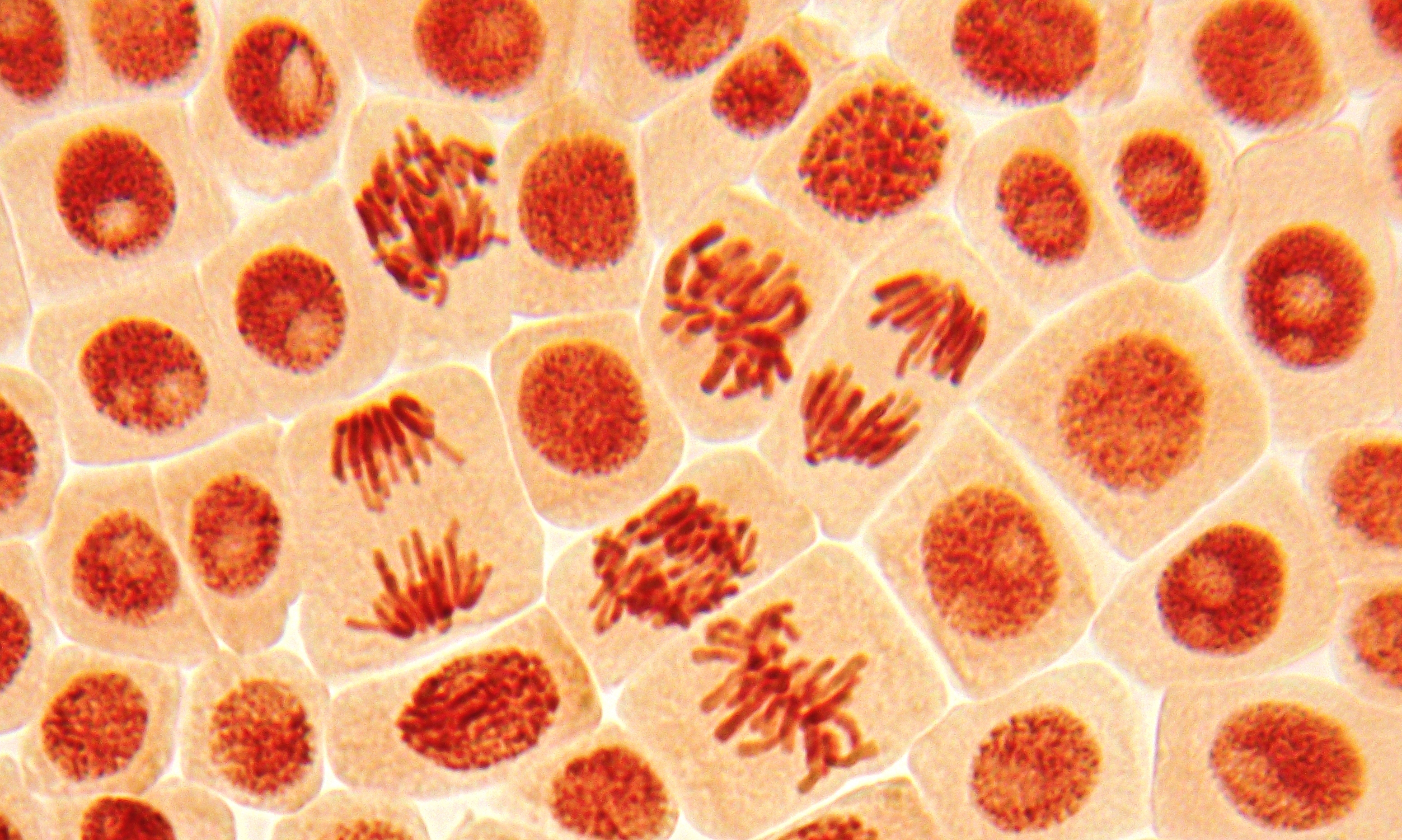
More than two decades ago, a group of scientists began delving into embryonic development to better understand how our cells are directed to make us as we are. It started as curiosity-driven basic research, but has now led to the discovery of a wholly new class of anti-cancer drugs that can stop specific cancer cells from proliferating – putting them to “sleep,” potentially permanently.
The research, just published in scientific journal Nature, has shown the compound works in animal models (mice and zebrafish) by blocking key genes involved in cancers like blood and liver cancers. Unlike chemotherapy and radiotherapy, there is no damage to healthy cells.

Health & Medicine
Breathing easy: Treating steroid resistant asthmatics
“This new class of compounds stop cancer cells dividing and proliferating by switching off their ability to continue the cell cycle,” says joint research leader Associate Professor Anne Voss of the Walter and Eliza Hall Institute of Medical Research and the University of Melbourne.
“The technical term is cell senescence, but essentially the cells are put to sleep. The cancer cells aren’t dead, but they are effectively stopped in their tracks.”
Joint research leader Associate Professor Tim Thomas, also of the Walter and Eliza Hall Institute and University of Melbourne, says that subject to clinical trials the compound has the potential to be “an entirely new weapon for fighting cancer.”
“The compound was well tolerated in our preclinical animal models and is very potent against tumour cells, while appearing not to adversely affect healthy cells,” he says.
At this stage it is unclear what happens to the “sleeping” cancer cells, but the researchers suspect that over time they could be killed and cleared by the immune system.
“We suspect that inducing senescence in the cancer cells will give the immune system more chance to clear these cells because they will eventually be recognised as abnormal,” says Dr Thomas.
The compound may also work as an adjunct for treatment where a therapy has already been effective in clearing a cancer. By inhibiting the specific processes involved in cancerous cell proliferation the compound could help keep a treated cancer in remission.
Health & Medicine
Our cancer preventing genes revealed
“It could be both a frontline treatment for specific cancers and a useful consolidation therapy for some other types of cancer,” says Dr Thomas.
The targeted genes are known as KAT6A and KAT6B and are involved in the growth and development of organisms.
“These genes control cell proliferation and are important in regulating how embryos develop to ensure that everything is in the right place and is the right size. But in some cancers, these are the same genes that will be mutating and driving the growth of cancer.
“So, we always had in the back of our minds that what we were exploring may have implications for treating cancer,” says Dr Thomas.

They had a breakthrough six years ago when team member and then University of Melbourne PhD student, Dr Bilal Sheikh, discovered that removing KAT6A from mice with fatal lymphoma (cancer of the lymph nodes carrying white blood cells) quadrupled their life expectancy from three-and-a-half months to about 14 months.
“By learning that KAT6A and KAT6B and the protein they express are important drivers in some cancers, we knew that if we could find a molecule of the right size and shape we should be able to inhibit or block it.”
But finding that right molecule was a lot easier said than done.
They had to screen almost a quarter of a million different potential molecules before they found one that had promise.
“In hindsight you’d have to say 1-in-nearly 250,000 aren’t great odds,” laughs Dr Thomas.
Health & Medicine
Exposing malaria’s atomic machinery
Indeed, unbeknown to the research team, which also includes Professor Jonathan Baell at the Monash Institute of Pharmaceutical Sciences and Dr Brendon Monahan at the Cancer Therapeutics Cooperative Research Centre, drug companies had been on the same trail but had given up, leading some to believe that these genes were “undruggable.”
It is understandable why. Just working out how to screen the molecules took the team a year of work.
They had to develop a robotic process in which the protein generated by the genes was suspended in a tiny droplet of solution that light would be shone through to monitor the chemical processes they were seeking to inhibit. The process was automated so that 384 molecules could be screened at once on a plate full of tiny wells, each holding a droplet of fluid.
“The research has been a big collaboration and that is most obvious in the screening and testing,” says Dr Voss. “Much of that work was done by the Cancer Therapeutics CRC.”

The next step now is to team up with a pharmaceutical company to pursue clinical trials on patients with the specific cancers that can be targeted through these genes.
“We think these compounds will be effective in treating those cancers where the proliferation of cancer cells through the cell cycle is driven by these KAT6A and KAT6B genes, and if we inhibit these genes it should have a therapeutic effect,” says Dr Thomas.
“For example, we think it will be effective in some blood cancers that block cells from differentiating normally into different cell types.

Health & Medicine
An unexpected step in the fight against stomach cancer
“In the case of leukaemia, the cancer causes the excessive proliferation of white blood cells, diluting oxygen-carrying red blood cells. Eventually a patient starts to lose their ability to circulate oxygen. We’d hope to be able to stop that from happening.
“I think the future of cancer treatments is very much going to be focused on developing specific treatments like this that target different cancer pathways, rather than a universally applicable therapy across cancer,” says Dr Thomas.
But the source of such treatments will always be knowledge-building, curiosity-driven research.
“We need first of all to understand how the body works if we are to reliably design new therapies, otherwise we are just relying on luck – trying something just to see if it works. Most therapies are derived from knowledge and then experimentation,” says Dr Thomas.
“It can be painstaking and slow, but if you are single-minded enough to keep going the rewards can be potentially life changing for patients.”
Banner Image: Time lapse image of a human cancer cell dividing. Picture: Kuan-Chung Su, London Research Institute, Cancer Research UK/Wellcome Collection