
Health & Medicine
Staying active in lockdown can make for a better normal

The discovery of how a key protein works in your liver to reduce blood glucose levels could lead to a more effective type 2 diabetes drug.
Published 3 September 2020
Type 2 diabetes affects 1.2 million Australian adults and 400 million people globally. But those figures are rising – fast – and there’s an urgent need to develop new approaches to treat people with this disease.
High blood glucose levels experienced by those with type 2 diabetes can lead to cardiovascular disease, nerve and kidney damage. While current treatments might be effective, they also have limited tolerability and significant side effects.

A University of Melbourne-led study published in Science Translational Medicine has found that the SMOC1 protein – naturally produced by the liver – can decrease blood glucose levels. This means an engineered form of SMOC1 could potentially treat people with type 2 diabetes.
Here, we ask lead author Dr Magdalene Montgomery and senior author Professor Matthew Watt, of the School of Biomedical Sciences, to explain how a new class of SMOC1-based treatments could prove more effective, and what it means for those living with this underestimated killer.

Health & Medicine
Staying active in lockdown can make for a better normal
Most of us know someone with type 2 diabetes. Not only is it already a common condition but it is likely to become even more widespread. Type 2 diabetes is closely linked to obesity and the reported incidence of obesity is growing – more than 2 billion people worldwide are overweight or obese.
It is estimated that 578 million adults will have diabetes by 2030, and 700 million by 2045.
High blood glucose levels are an underestimated killer. People with diabetes have many complications that can affect their quality of life and contribute to a reduced life expectancy, including high blood glucose. If left unchecked and untreated, it can cause the development of many serious health problems.
It is one of the reasons why people with diabetes are up to four times more likely to suffer heart attacks and strokes, while kidney failure is three times more likely.
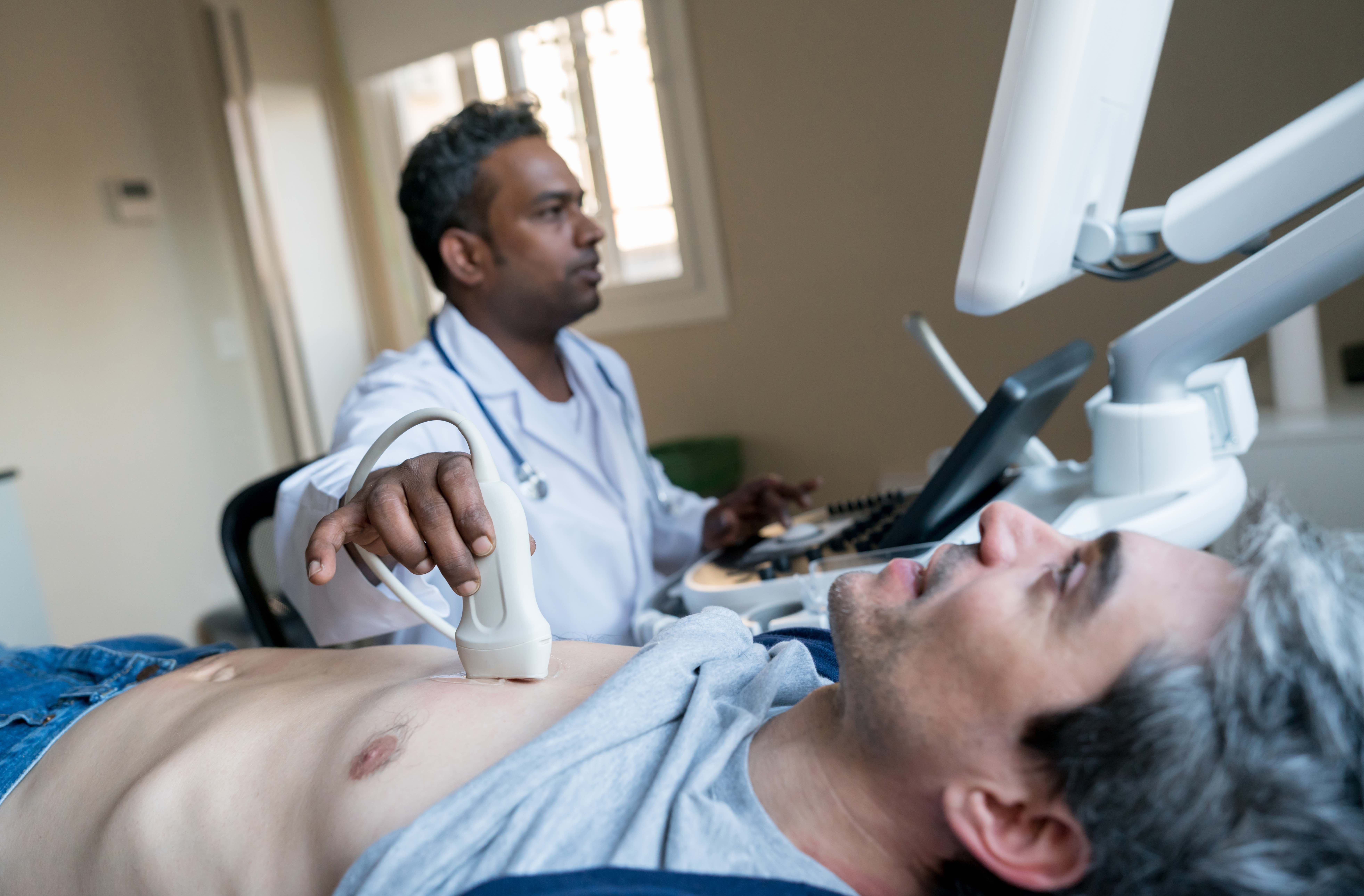
Diabetes can also lead to peripheral artery disease, which causes your blood vessels to narrow and reduces blood flow to your legs and feet. This puts patients at increased risk of developing ulcers on the feet and legs which can become infected, and in the worst cases, develop gangrene. Tissues die and amputation is required.
It is also the leading cause of preventable blindness in Australia.
The constant stress caused by the disease, including the need to manage glucose levels, also takes a mental toll and one in three people with diabetes experience depression, anxiety and/or distress.

Health & Medicine
Sea snail venom holds clues for diabetes treatment
Reducing blood glucose levels before any sign of diabetes damage is evident can work to prevent the complications of this silent and underestimated killer.
There are several medications that help maintain a patient’s blood glucose levels. Metformin tops the list, with physicians prescribing it to more than 120 million people worldwide. However, while Metformin is generally a safe and effective treatment, it frequently causes gastrointestinal symptoms like diarrhoea and flatulence.
In fact, all diabetes medications have either limited effectiveness or unintended effects that can impact on a patient’s health.
An additional complication with many diabetes medications is the possibility of causing hypoglycemia (very low blood glucose levels). This is a day-to-day concern for diabetics as hypoglycemia can leave them feeling shaky, anxious, sweaty, cold, lightheaded, confused and, in severe cases, can even induce coma or death.

So, there is an urgent need to develop new approaches to treat patients with this disease.
Our research team recently identified a novel protein called SMOC1. This is naturally produced by the liver and is released into the blood when glucose levels are high. The finding suggests this protein plays a role in the control of blood glucose. Indeed, when SMOC1 is injected into diabetic animal models blood glucose control substantially improves.
Health & Medicine
The vaccine that may help prevent type 1 diabetes
Following this observation, we engineered a long-lasting form of SMOC1, which only needs to be injected once a week. So far, the results have shown this to be effective in managing blood glucose levels. Notably, SMOC1 was found to be more effective than Metformin.
The common side effects of hypoglycemia in animal models were also not seen in the research. Additionally, the engineered SMOC1 reduced fatty liver and blood cholesterol levels, which are also common health problems in type 2 diabetes patients.
We anticipate SMOC1 could be effective in people with newly diagnosed and advanced type 2 diabetes. The engineered long-lasting SMOC1 would make daily medications a thing of the past, which would work to improve a patient’s quality of life.
Given the prevalence of type 2 diabetes, the impact on reducing the burden on the health care system would be sizeable, with less hospital visits and shorter hospital stays related to this new treatment.
We now need to carry out trials of SMOC1 in humans. With the right support from the pharmaceutical industry, SMOC1 could move to human trials relatively quickly. Potentially within six to eight years we could have an available new medication, helping us get closer to relieving the increasing global burden associated with type 2 diabetes and obesity.
Banner: Getty Images