
Health & Medicine
How caffeine helps premature babies breathe easy

Modern medical care for pre-term newborns is inadvertently causing more lung issues for these children as they grow up, compared to older techniques
Published 31 July 2017
After decades of incremental improvements in neonatal wards, you’d expect babies born in recent times to be doing much better than those born 25 years ago.
But surprisingly, new research from University of Melbourne Professor of Neonatal Paediatrics Lex Doyle and his colleagues shows the opposite.
Professor Doyle, who works at the Royal Women’s Hospital in Melbourne, studied children born at 22-27 weeks in 1991-1992, 1997 and 2005.

They looked at how much medical help premature babies received to assist their breathing, from ventilators and other techniques, and then assessed their lung function as eight-year-olds.
Their findings, published in the New England Journal of Medicine, show the 2005 group received more assistance for a longer period than the earlier groups, but their lung function at age eight was worse.
“The differences aren’t huge, but they’re going in the wrong direction,” says Professor Doyle. He says he suspects the extra medical help premature babies now receive to aid their breathing might be the cause, but cautions that further research is needed.
His paper points out that equipment to monitor blood oxygen levels did not exist in the 1970s but is ubiquitous now, meaning clinicians are aware of even slight dips in oxygen, sometimes brought on by a brief pause in breathing.
“The result is pre-term babies are receiving help to breathe for longer, being exposed to more oxygen and their lungs are not quite so good at age eight.
“We have to make sure we use the tools appropriately. Just because they’re there, doesn’t mean they have to be used.”
Extremely premature babies – those born at 27 weeks or less – who survive often do so with the aid of corticosteroids (a class of steroid hormones) given to their mothers before birth. They are also helped by ventilators that assist their breathing, monitoring equipment to check their vital signs, and medicines to prevent their tiny lungs from collapsing after birth.
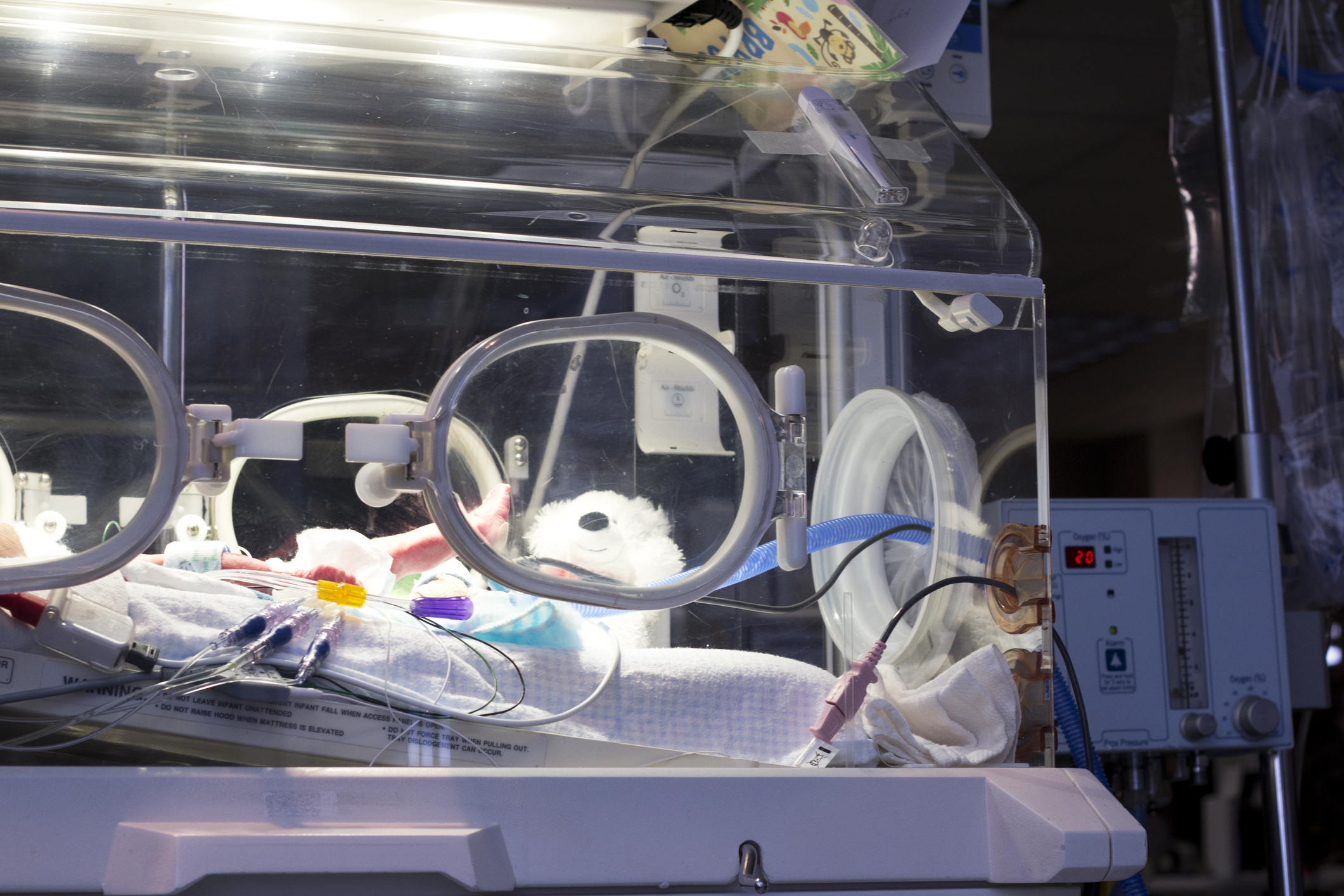
“Pre-term babies sometimes lack surfactant, a substance that helps prevent their lungs from collapsing, and they can tend to forget to breathe, known as apnoea,” says Professor Doyle.
“They face many hurdles and their treatment is a delicate balancing act.”
To understand why the group of children born in 2005 fared worse than the older children in Professor Doyle’s study, it is necessary to look at how this highly specialised area of medicine has evolved.
Oxygen was first pumped into enclosed incubators from the 1940s. Although it saved some lives, unfortunately it was often overused and a lot of babies went blind in the ten years or so it took to discover what was happening, says Professor Doyle. High exposure to oxygen was eventually linked to retrolental fibroplasia (RLF), an eye disease that can affect premature babies which involves irregular blood vessel growth interfering with vision, potentially leading to the retina being detached.
The first ventilators began pumping oxygen-enriched air into tubes down babies’ windpipes in the 1960s, and was adopted in Melbourne in the 1970s.

Health & Medicine
How caffeine helps premature babies breathe easy
“This had some success but a lot of the babies still died,” says Professor Doyle.
In the late 1970s doctors started giving corticosteroids to pregnant women at risk of going into early labour. This helped babies produce surfactant before birth.
To counter apnoea clinicians started giving babies methlyxanthines which are similar to caffeine, and later actual caffeine.
In 1991 doctors in Australia began giving babies synthetic surfactant and their outlook improved significantly. Around the same time ‘non-invasive ventilation’ was introduced and became the preferred way of helping babies breathe.
Instead of tubes down their throat, pre-term babies now had two little tubes resting just inside their nose with Continuous Positive Airway Pressure (CPAP) delivering air and oxygen, and helping their lungs stay inflated.
But a seemingly unavoidable problem is that while pre-term babies must breathe air to survive, oxygen also damages their tiny lungs, potentially leading to problems in adulthood such as such as emphysema.
This is why Professor Doyle says it is so important to check in with the babies as they grow up.
“The reason we do these studies is we’ve got to make sure that what we do in the newborn period doesn’t have adverse long-term consequences.
“I think of it as quality control.
“If there’s something we see that’s not quite right, we have to look back and say, ‘What’s different? What can we do?’”

He admits he expected to find those born more recently, who received less invasive treatments and newer medicines, would have better lung function as eight year-olds.
“But no. It went the other way. Lung function looked like it might have been getting better between the 1991-1992 group and the 1997 group. But the 2005 group was definitely worse than both earlier groups,” Professor Doyle says.
“It’s a worry and we’ve clearly got a problem that we’ve got to sort out. We’ve got to think of what we’re doing in the newborn period. Can we support them for shorter periods or more gently again, or use other methods that won’t aggravate their lungs?

Health & Medicine
Predicting premmies: The test that could save babies’ lives
“I think sometimes perhaps we’re over-treating some of that. But that’s pure guesswork, I can’t prove that.
“I think maybe we’ve gone a little bit too far with the help with breathing, but I can’t be certain about that, either,” says Professor Doyle.
But medicine is constantly evolving.
Since 2005 a new technique has been devised with smaller lighter tubes sitting just inside the baby’s nostrils delivering gas using a high flow rate, replacing CPAP in many cases.
“They’re much lighter and friendlier, but we don’t yet know what the long-term consequences are of that treatment.
“In the short-term they have been shown to help, but we need to wait and see what the long-term effect is,” says Professor Doyle.
Banner image: iStock