
Health & Medicine
Where are all the missing girls?
Global rates of caesarean section are rising alarmingly, especially in Asia, and as the Indonesian experience shows, these rates are accompanied by widening inequality in access
Published 5 January 2021
Caesarean section rates are increasing globally at an alarming rate. In some countries more than half of births are by caesarean section.
It is alarming because, while caesarean section can be a life-saving procedure when complications arise during childbirth, there are no additional health benefits for women and babies if it is used without good clinical reason.
Unnecessary caesarean sections are a waste of scarce health resources.

There are important differences in caesarean section rates both between and within countries.
For instance, at a national level, caesarean section rates are over 50 per cent in the Dominican Republic Brazil, Egypt and Turkey, compared to around 30 per cent in Australia and the USA, and less than three per cent in South Sudan, Nigeria and Ethiopia.
The World Health Organization has advised that caesarean section rates higher than 15 per cent at a population level may not improve women’s or babies’ health; while caesarean section rates below 10 per cent may be a sign of inadequate access to quality maternity care.
It means that globally people are undergoing caesarean sections when they don’t need it and others who do need it are missing out.

Health & Medicine
Where are all the missing girls?
There is a need then to optimise the use of caesarean section globally.
We need to reduce caesarean section use in women who are over-receiving it without good medical reason, while also increasing caesarean section use in women who are under-receiving it.
Asia is the region where rates of caesarean section are rising the fastest.
Taking Indonesia as an example, our research has found that rising rates of caesarean section has been accompanied with a troubling increase in inequalities in term of access to the procedure.
We analysed the trends of caesarean section and its inequalities over 30 years – between 1987 and 2017 – in Indonesia using seven waves of the Demographic Health Survey.
We found profound inequalities in which groups of women receive caesarean section in Indonesia – relatively advantaged (e.g. highly educated) groups of women are over-receiving caesareans while disadvantaged groups (e.g. no school education) are under-receiving the procedure.
We found that caesarean section rates have increased steadily in Indonesia from 1.6 per cent in 1991 to 17.6 per cent in 2017.
We also found that caesarean rates were higher in public health facilities compared to private health ones – and that is despite more births occurring in private facilities.

This is a unique trend compared to other countries where the majority of caesareans occur in private health facilities. The more usual higher prevalence in private facilities may reflect non-medical factors like people simply paying up to have the procedure.
However, in Indonesia, healthcare providers receive higher payments for caesarean births compared to vaginal birth, which may unintentionally be encouraging health providers to overuse caesarean section.
While the national rate of caesarean section in Indonesia is marginally higher than the 10-15 per cent optimal threshold, it hides important inequalities.
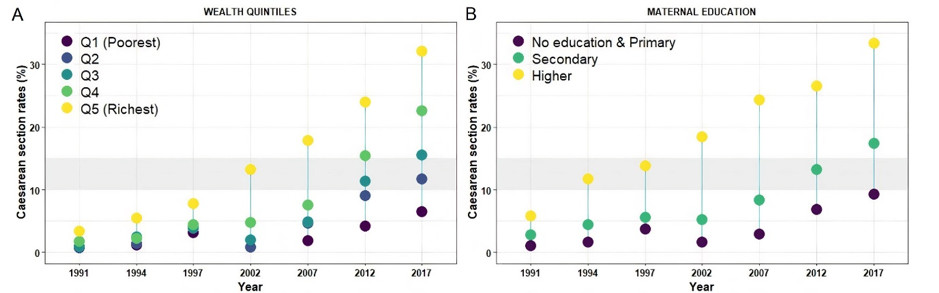
We identified widening absolute inequalities across all socio-economic determinants we analysed – across regions, woman’s urban or rural residence, women’s household wealth and women’s education.

Health & Medicine
Do new doctors get enough child health experience?
We found significantly higher rates of caesarean section among women who live in Western Indonesia (the most wealthy and advantaged areas), compared to Eastern Indonesia (the poorest and least advantaged areas).
For example, Jakarta and Bali have caesarean rates of 31.3 per cent and 33.4 per cent respectively, compared to North Maluku and Papua at only 6.7 per cent and 9.8 per cent.
This wide gap between advantaged and disadvantaged women is concerning.
In 2017, the caesarean rate among women with a higher education qualification was 33.4 per cent compared to 3.4 per cent among women with no education. Likewise, the caesarean section rate among the wealthiest group of women was 32.1 per cent compared 6.5 per cent among the poorest women.
Monitoring health inequalities over time is critical to identify differences in health across population groups, and to generate evidence on who is being left behind.
This evidence should be used to inform the development of health policy and programs that aim to close gaps and achieve health equity for all.
There are key questions that remain to be answered: do women in Indonesia prefer and make informed decisions to have a caesarean section? Or does the health system and healthcare providers channel women into having a caesarean section for other reasons, such as based on the woman’s status, provider preference, or financial incentives?

To date, there are no studies exploring these important questions in Indonesia. However, studies conducted in other countries have found many factors are influencing the increasing rates of caesarean section.
Some women may prefer to have a caesarean section due to a previous negative childbirth experience, fear of labour pain and a perception that it is “safer, quick, painless and easy” compared to vaginal birth.
Moreover, maternity providers may prefer caesarean section over vaginal birth due to fears of litigation, because of financial incentives in the health system, the convenience of scheduling, or the belief that caesarean is a safer option.

Health & Medicine
Many of the world’s women are mistreated during childbirth
Based on historical trends, caesarean section rates will likely keep increasing in Indonesia in coming years.
Importantly, the COVID-19 pandemic may serve as a catalyst to accelerate the increase of caesarean section as a result of misinformation. Some media in Indonesia reported that all pregnant women are mandated to have caesarean section during the pandemic (regardless of COVID-19 status), contrary to the risk-based decision-making suggested by national guidelines.
This misinformation may exacerbate women’s preferences for caesarean section, or encourage providers to undertake caesarean section. Indeed, local media reported a rapid 20 per cent increase in caesarean section from January to May 2020 in Pamekasan District of East Java.
Public health programs in Indonesia should aim to optimise the use of caesarean section.
This includes implementing measures to reduce non-medically justified caesarean sections in regions and groups of women with high rates of caesarean section, while simultaneously improving the uptake of caesarean section in groups where rates are low.
This may be done by implementing antenatal education and decision-aids for women and their families on the benefits and challenges of vaginal birth versus caesarean section, as well as auditing the compliance of health providers with guidelines and providing feedback.
Health programs also need to balance women’s preferences for vaginal or caesarean birth, with the health benefits and risks of different ways to give birth.
Maternity care providers should support women to express preferences, while managing expectations about likelihood of the fulfilment of preferences, in order to minimise feelings of disappointment and improve women’s experiences of care.
Banner: Getty Images