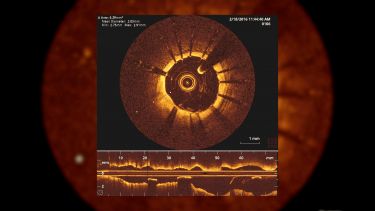
Health & Medicine
Using maths to assess blocked arteries
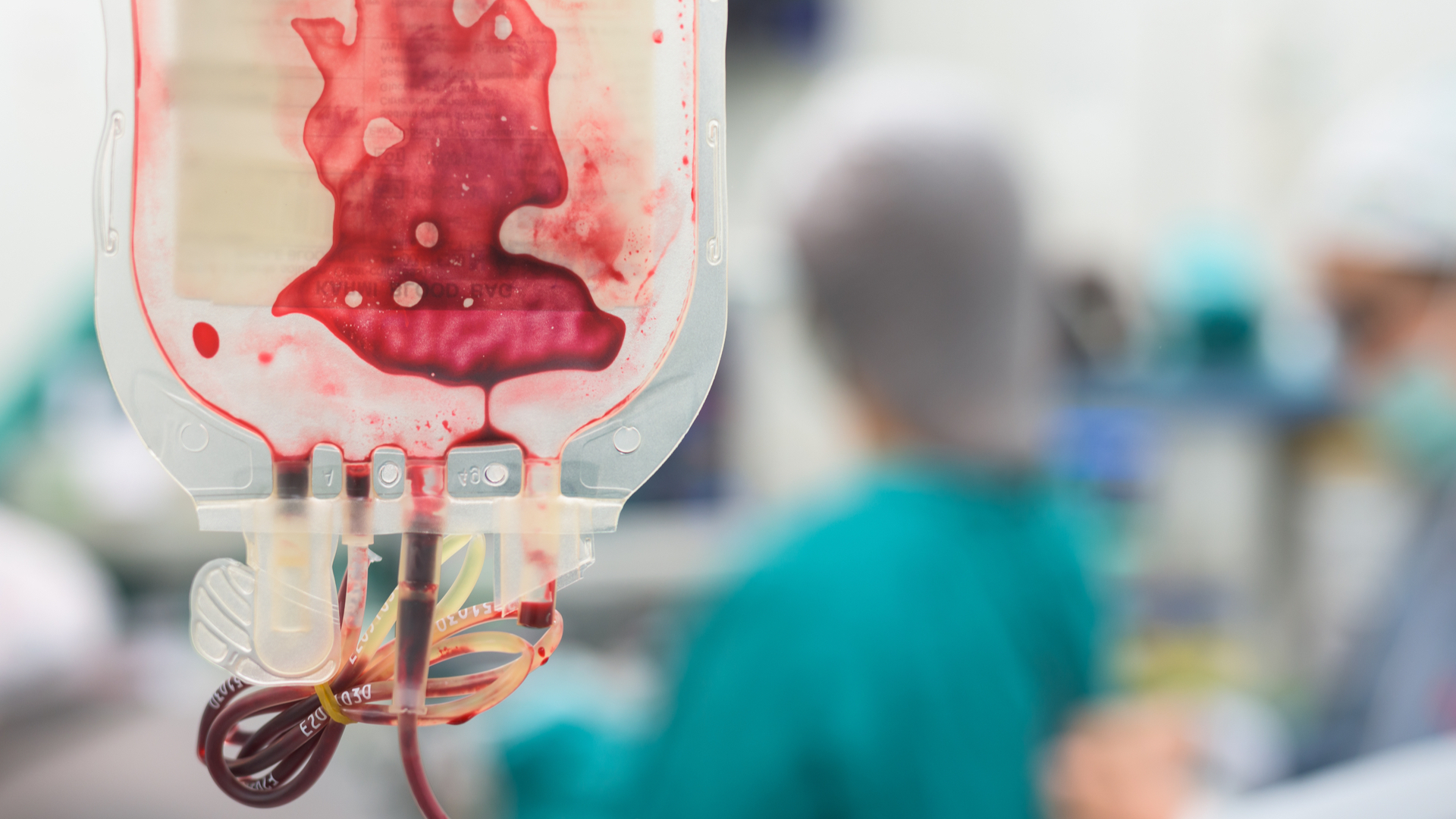
Heart surgery uses more precious donated red blood cells than almost any other procedure, but a major global study has confirmed that its safe for surgeons to use less
Published 13 November 2017
Heart surgery requires more blood transfusions than almost any other surgical procedure.
But a major international study of over 5,000 heart surgery patients has now shown that surgeons can safely use significantly less blood than they have been. The potential saving is equivalent to around one blood donation (about 470 millilitres) per moderate-to-high risk patient.
During a heart bypass operation, a patient’s blood is first drained into the heart-lung machine and then pumped back into the patient. The heart is then flushed with potassium to put them into cardiac arrest. Primed with 1.5 litres of mostly salty water, the machine pumps about 4.5 litres a minute of blood through an oxygenator and then back into the patient’s bloodstream.
The fluid is needed to displace all of the air in the pump circuit. Within about 60 seconds, the pump prime dilutes a patient’s blood by about a third, diluting the blood’s oxygen-bearing haemoglobin and leaving patients anaemic.
“It is one of the most dramatic alterations to someone’s blood composition in all of medicine,” says Royal Melbourne Hospital heart surgeon and University of Melbourne deputy director of surgery Professor Alistair Royse.
It is why heart surgery requires high quantities of blood as patients generally need red blood cell transfusions to boost their haemoglobin levels. But the evidence is now in that patients can safely tolerate lower levels of haemoglobin during surgery, meaning less blood is needed.

Health & Medicine
Using maths to assess blocked arteries
“This study may significantly change clinical practice across the globe by supporting the ongoing trend towards using blood transfusions at a lower haemoglobin concentration,” says Professor Royse who led the Australian arm of the study that involved over 620 patients across 12 hospitals in Victoria, New South Wales and South Australia.
“There is a philosophical mind-set towards using less blood and what this study shows is that it is safe to be going down this pathway,” says Professor Royse.
Using less blood during heart surgery would represent a significant cost saving to health systems globally. In Australia while blood is given freely by donors, it costs AU$412 per unit to supply red blood cells. On top of that there are hospital costs that Professor Royse says can take the total cost of a completed transfusion up to as much as AU$1,000 per unit.
Led by principal investigator Professor David Mazer from the University of Toronto, the five-year study, published in the New England Journal of Medicine, is the largest of its kind and monitored patients at 73 institutions across 19 countries. Australia’s National Health and Medical Research Council provided AU$1.4 million in funding that was crucial in the study being expanded from an initially planned 3,500 patients to more than 5,000.
Over the last decade there has been a growing international trend among heart surgeons to use less blood, not just to save limited donated blood supplies, but also to avoid the rare health complications that can arise from blood transfusions. These include allergic or immune reactions to the introduced blood, and the risk of receiving disease infected blood.
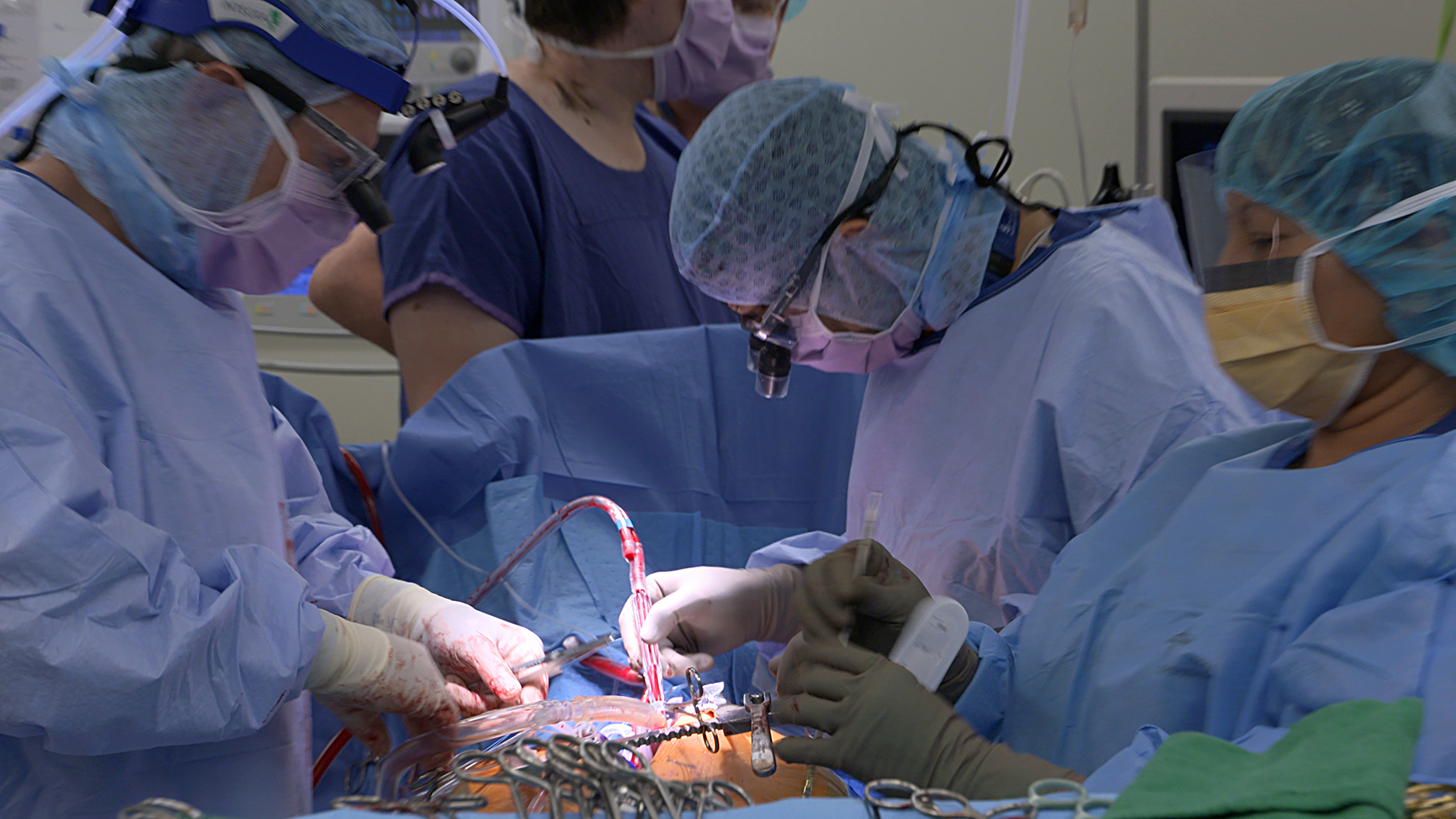
But the safety of tolerating lower haemoglobin levels in heart surgery patients was thrown into doubt in 2015 by a study of just over 2,000 patients in the UK.
The study found that the death rate 90 days after surgery among those treated with lower haemoglobin levels was 4.2 per cent, much higher than the 2.6 per cent death rate among the group treated with higher haemoglobin levels. While the nature of the deaths didn’t indicate a causal link to haemoglobin levels, the researchers concluded that the results were a cause for concern.
However, this much larger international study, which was focused on moderate-to-high risk cardiac patients who are more likely to need transfusions, found no significant difference in outcomes between a low-haemoglobin treatment regime and a more traditional regime.
“The UK study raised a lot of questions and this study was specifically designed to answer the question of whether a restrictive haemoglobin regime was as safe as the standard liberal regime, and the answer according to our study is yes, it is just as safe,” says Professor Royse.
Health & Medicine
Surgeons go green: Recycling general anaesthetic
The randomised study recruited heart surgery patients aged 18 and over who were classified as being moderate-to-high risk, and then tracked them from the start of their operation until discharge, or 28 days, whichever came sooner.
In half the patients, surgeons tolerated a diluted haemoglobin level as low as 9.5g/100mls, representing a more “liberal” and traditional use of blood. That compares with normal haemoglobin levels of around 14g/100ml. But the other, more “restrictive” group were allowed to tolerate haemoglobin levels as low as 7.5g/100mls.
Contrary to the smaller UK study, the death rate was actually slightly lower in the “restricted” group at 3 per cent compared with 3.6 per cent for the “liberal group.” The proportion of patients that experienced either a subsequent heart attack, stroke, kidney failure or death was also lower among the restrictive group at 11 per cent, compared with 12 per cent for the liberal group.
“Given the large sample size we have, these results are more than sufficient to be confident that the restrictive practise wasn’t inferior to the liberal practice,” says Professor Royse.
Dr Chris Hogan, a haematologist and transfusion medicine specialist who works with Professor Royse at Royal Melbourne Hospital, says the study represents “landmark” evidence supporting the trend toward using less blood.
“To date, there has been significant concern, and a lack of a very strong evidence base, to extrapolate this type of more conservative and restrictive transfusion practice to cardiac surgical patients,” says Dr Hogan. “But these research findings represent a landmark study in the contemporary transfusion medicine literature, and should now confidently inform transfusion practice in cardiac surgical settings.”
The ideal next step says Professor Royse to undertake an economic analysis to quantify the cost savings of implementing a more “restrictive” haemoglobin regime. There is also scope he says to research the safety of tolerating even slightly lower haemoglobin levels.
“This study has been extremely successful, the whole system worked really well at the lower threshold and it was a great outcome. But from here we need to go the next step and investigate how low should we go,” says Professor Royse.
“We also should be researching whether we have to dilute blood during heart surgery as much as we do in the first place.”
Banner image: Shutterstock