
Health & Medicine
Saving lives when the power goes out
By targeting an essential nutrition pathway, researchers hope to develop drug targets against the bacterium that causes pneumonia
Published 7 August 2021
The invitations, decorations, candles and the cake – there’s a lot to remember when you organise a birthday party for a five-year-old. One thing we thankfully take for granted in Australia is that our five-year-olds reach this milestone at all.
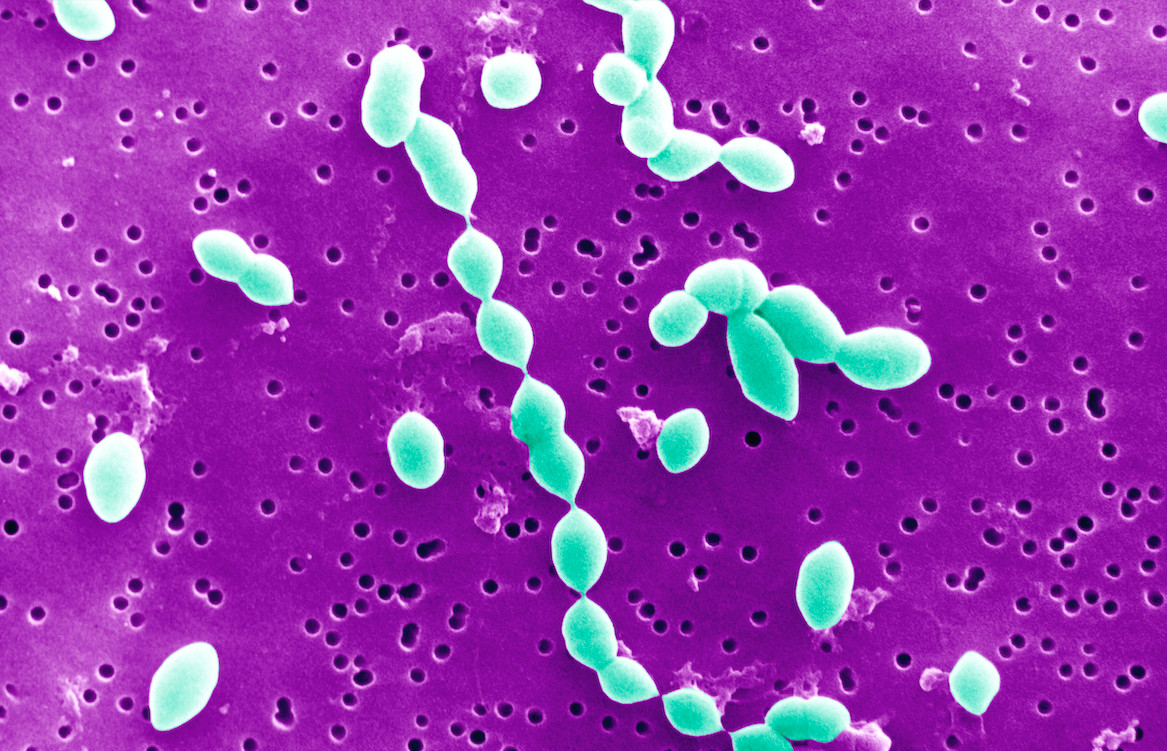
But close to half a million children infected worldwide by the bacterium Streptococcus pneumoniae each year, never make it to their 5th birthday.

Like COVID-19, Streptococcus pneumoniae spreads in droplets when we cough or sneeze. It is responsible for deadly pneumonia, meningitis, sepsis or blood poisoning, as well as inner ear infections that commonly cause deafness in Aboriginal and Torres Strait Islander children.

Health & Medicine
Saving lives when the power goes out
Before the COVID-19 pandemic, S. pneumoniae was the leading cause of death by pneumonia globally. It accounted for more deaths than all other causes of pneumonia combined in 2016.
This is despite the widespread use of antibacterial agents, vaccines and antibiotics, to protect against S. pneumoniae infections. Our current vaccines provide limited protection, working against only a fraction of all strains of S. pneumoniae. The other challenge is that resistance to antibiotics is rapidly developing.
New approaches are urgently needed to prevent death and to treat the disease and disability caused by S. pneumoniae, like brain damage, hearing loss and impaired lung function into adulthood.
One new approach may be to starve the pathogen.
“Vitamins and minerals including iron, copper, zinc and manganese are critical for human health, but bacteria need them too,” explains Associate Professor Megan Maher, a structural biologist and chemist at the University of Melbourne’s School of Chemistry and Bio21 Institute.

Over a decade ago, Professor Christopher McDevitt, laboratory head at the Doherty Institute, and Associate Professor Maher forged a collaboration to pursue a clue that manganese was vital for the survival, metabolism and infectivity of S. pneumoniae.

Health & Medicine
The Indigenous eye-care gap is closing, but not fast enough
Professor McDevitt, a microbiologist, first identified that zinc was toxic to S. pneumoniae because it blocked manganese from coming into the cell.
“Our work showed that the pathogen had to steal manganese from the body to cause infection. Part of the body’s immune response against the bacterium was to use zinc to block this pathway,” says Professor McDevitt.
Knowing that manganese was an essential mineral for the pathogen, Professor McDevitt and his team searched for and identified the ‘gate’ or transporter in S. pneumoniae that is specific for taking in manganese.
“S. pneumoniae only has a single transporter to take up this essential nutrient. We already knew that if you disrupted any part of that transporter the pathogen was incapable of causing an infection. As this type of transporter isn’t in humans, it makes an ideal target for new antimicrobials,” explains Professor McDevitt.
“The ultimate goal was to determine the structure of the transporter that S. pneumoniae uses, in order to design drugs against it. At the time this was very difficult to do so Professor McDevitt approached me and asked, shall we go for this?” recalls Associate Professor Maher.
“To understand how the transporter works, we used X-ray crystallography,” says Associate Professor Maher.

This technique requires crystals of the protein to be grown in the lab, and then an X-ray beam is directed at the crystals. For each crystal, light scatters in a unique way, known as a diffraction pattern, to build a precise three-dimensional structure of the protein. These 3D structures are depicted as beautiful loops, sheets, and spirals.

Health & Medicine
Molecules in motion
But extracting the manganese transporter from S. pneumoniae was a particularly difficult task because it was tightly embedded within the bacterial cell membrane, where it serves to control the entry of the metal to the cell.
The cell membranes act as a barrier between the inside of a cell, which contains the machinery necessary for life, and the outside world. It is composed of fat or ‘lipid’ molecules. This makes the membrane proteins located within them particularly challenging to isolate.
“It took us six years, including time at La Trobe University, and was completed at Bio21 Institute. Membrane proteins are among the most difficult classes of protein you can work on and so represent only a tiny proportion of all known protein structures because they are so tricky, that’s why it took six years,” says Associate Professor Maher.
“We used detergents to take the protein out of the membrane and keep it soluble in solution. Once the protein was encased by a shield of detergent molecules, we grew crystals with the detergent present.”
Protein crystals are grown under highly controlled conditions. It can take weeks, months and many attempts to get the conditions right to grow them.
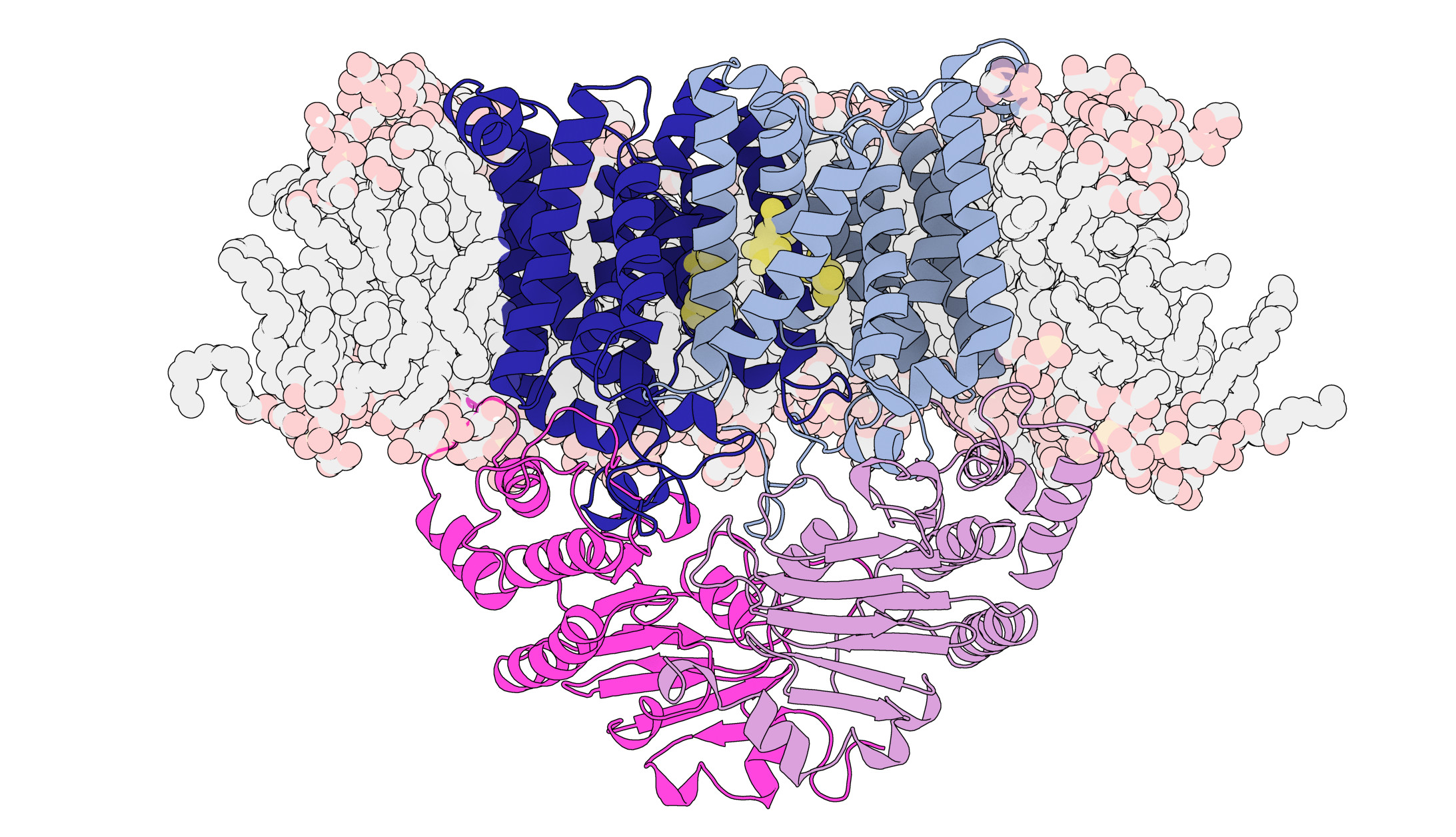
“This manganese transporter certainly did give us a lot of surprises. It belongs to a very large family of proteins called ‘ABC transporters’ but looks quite different to others in the same family, where the structures have already been revealed,” explains Associate Professor Maher.
Health & Medicine
Improving how we manage sepsis
“It is smaller and more compact than other ABC transporters and has a distinctive pathway where the manganese travels through. Similar ABC transporters have been referred to as ‘teflon-coated channels’ where once the correct molecules are received by the transporter, they just slide through it into the cell without any interactions,” she says.
“What we’ve discovered is a unique pocket halfway through the transporter, which specifically interacts with the manganese.”
Membrane proteins that work as gateways in cell membranes are particularly interesting as drug targets because of their important roles in transporting essential molecules – like manganese – as well as in signalling and other functions.
“Manganese is a tiny chemical species. For the transporter to specifically select for it, there needs to be an interaction inside of the gateway to help pull the correct molecule through. It’s an example of ‘coordination chemistry’,” explains Professor McDevitt.
“With lots of other soluble proteins, we can predict what they are going to look like because we already have so many other structures in databases we can compare to. Because we don’t have many structures for membrane proteins, when you get a new structure, it’s often quite different from the ones that already exist out there,” says Professor McDevitt.
“Knowing the structure is the first step to developing a drug or therapy against S. pneumoniae. Our approach would be to block this pathway and prevent the transporter from bringing manganese into the bacterium,” says Professor McDevitt.
“This can be done by creating specific antibody drugs or other binding molecules that specifically target this transporter and block it. That’s what we’ll be working on next,” explains Associate Professor Maher.
Traditionally, antibiotics against S. pneumoniae target cell wall production, but currently there are no antibiotics that target nutrition for the organism.
Targeting the gateway that allows S. pneumoniae to obtain the essential element manganese is a completely new approach and a positive step towards a new way to tackle the rising rate of antibiotic resistance.
Banner: Streptococcus Pneumoniae, Sem 7800X. Credit: BSIP/UIG Via Getty Images