Health & Medicine
Rethinking premature baby care
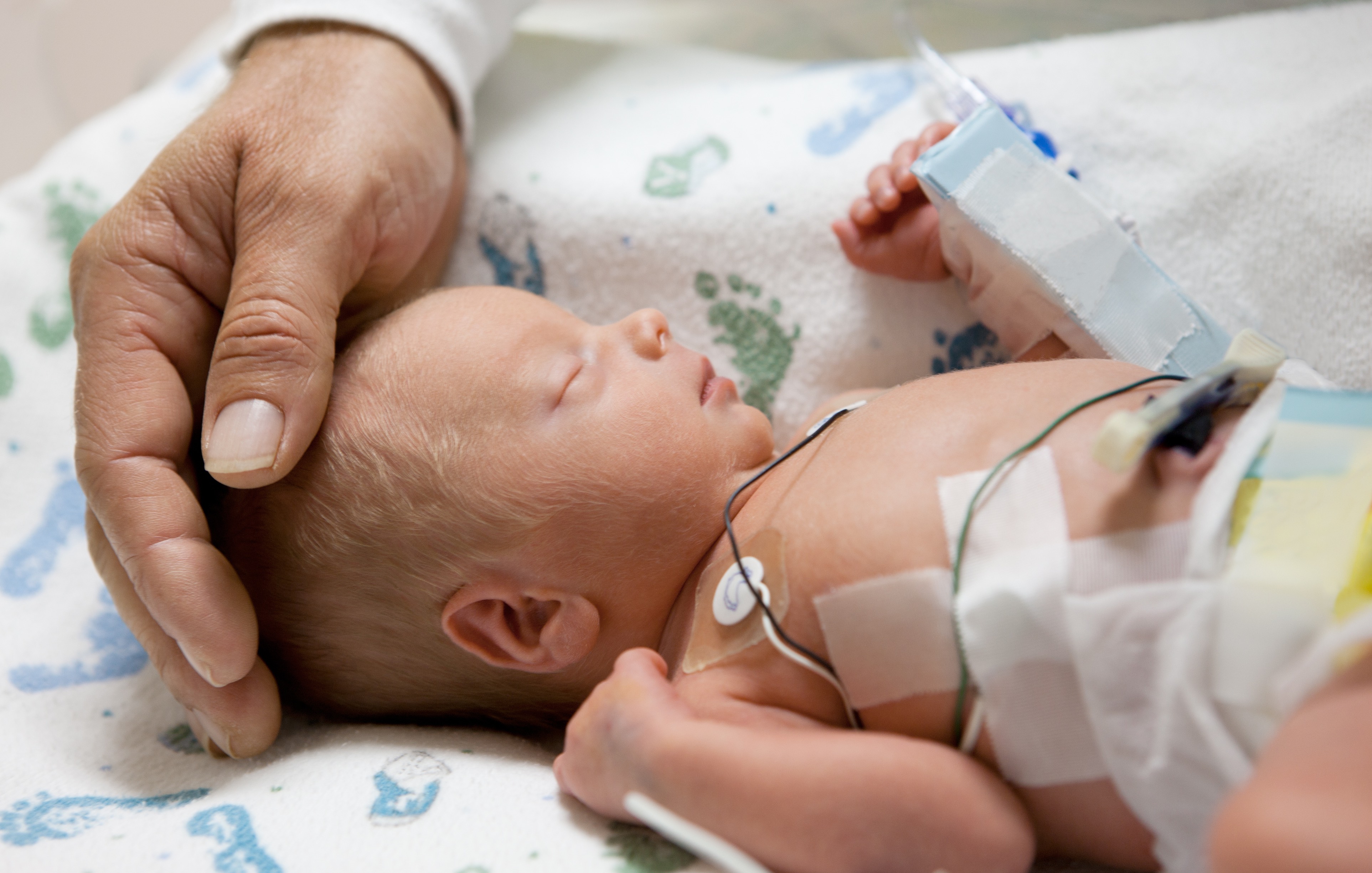
An Australian-first study has found that underweight preterm babies face no more risk of serious short-term complications than normal weight preterm babies of the same gestational age
Published 28 October 2017
Pregnancy should be an exciting time for all couples, but can become very stressful if their baby is not growing as expected.
Intrauterine growth restriction (IUGR) is a common complication of pregnancy and in the majority of cases involves the placenta not providing enough nourishment to meet the needs of the growing baby.

Babies are usually diagnosed with IUGR when they have an expected birthweight that is below the tenth percentile for their gestational age. It is well known that babies born prematurely can be at risk of serious complications in the newborn period; it is less well known whether babies who are both small for their age and premature suffer additional complications.
There is no treatment for IUGR, doctors can only monitor the baby’s progress and decide if and when it needs to be delivered early by induction of labour or Caesarean section. Babies with IUGR are often born early when monitoring indicates that delivery is safer than the risk of worsening growth, and possible non-survival if pregnancy continues.
A new study has found that babies with IUGR who are born preterm at a Melbourne hospital fared no worse than normally grown preterm babies. This reassuring retrospective data confirms that gestational age at delivery has the greater impact on newborn outcomes.
This result indicates doctors are monitoring the condition well and making the correct decision about if and when to deliver these IUGR babies.

Health & Medicine
Rethinking premature baby care
Lead researcher Dr Bridie Stewart, an obstetrics and gynaecology resident at Western Health’s Sunshine Hospital, conducted the study when she was a University of Melbourne medical student under the supervision of Associate Professor Joanne Said.
“This is a common complication of pregnancy,” Dr Stewart says of IUGR.
“The only management we have is monitoring and deciding on the optimum time for delivery.”
Dr Stewart explains that IUGR is diagnosed and monitored using ultrasound technology to observe the growth of the baby, blood flow between mother and baby and fluid around the baby, as well as the baby’s heart rate. Doctors must then decide on a case by case basis if and when the baby is safer outside the womb.
“It has a number of causes but the most common cause is called placental insufficiency,” she says of IUGR. “The placenta that supplies blood, oxygen and nutrition to the baby isn’t working as it should.”
While past cohort studies have investigated preterm IUGR outcomes elsewhere, this was the first time an Australian cohort has been reviewed.
Published in the Australian and New Zealand Journal of Obstetrics and Gynaecology, the study looked at pre-term babies born at Western Health’s Sunshine Hospital between 32 and just under 37 weeks of pregnancy from January 2012 to December 2014.
The study found that abnormalities in fetal monitoring was the main reason for preterm delivery of IUGR infants, but there were also other pregnancy complications causing preterm delivery such as high blood pressure in the mother.

Of the 146 infants born during the study period who were considered small for their gestational age, 103 were born early for medical reasons. The smaller babies had higher odds of hypoglycaemia and neonatal jaundice than pre-term babies who were normally grown for their age, but there was no increase in the risk of respiratory distress or sepsis, both of which can have significant implications for newborns.
“This result provides reassurance the current practice appears to be optimising outcomes overall. It provides support for obstetricians when they are counselling women who may be facing a preterm delivery for a growth restricted pregnancy.”
Dr Stewart’s study identified the need for more research to corroborate the Melbourne findings.
Banner image: iStock