
Health & Medicine
As a health worker, what’s my risk from COVID-19?

From a key role in intensive care to recovery rehabilitation, physiotherapists are working on the frontline to help COVID-19 patients recover
Published 20 August 2020
While 2020 has been an unprecedented year around the world, this is especially true for the health workforce who are working tirelessly in the fight against COVID-19.
This new disease has required health professionals to stop, reflect and quickly adapt in order to care for patients with COVID-19.
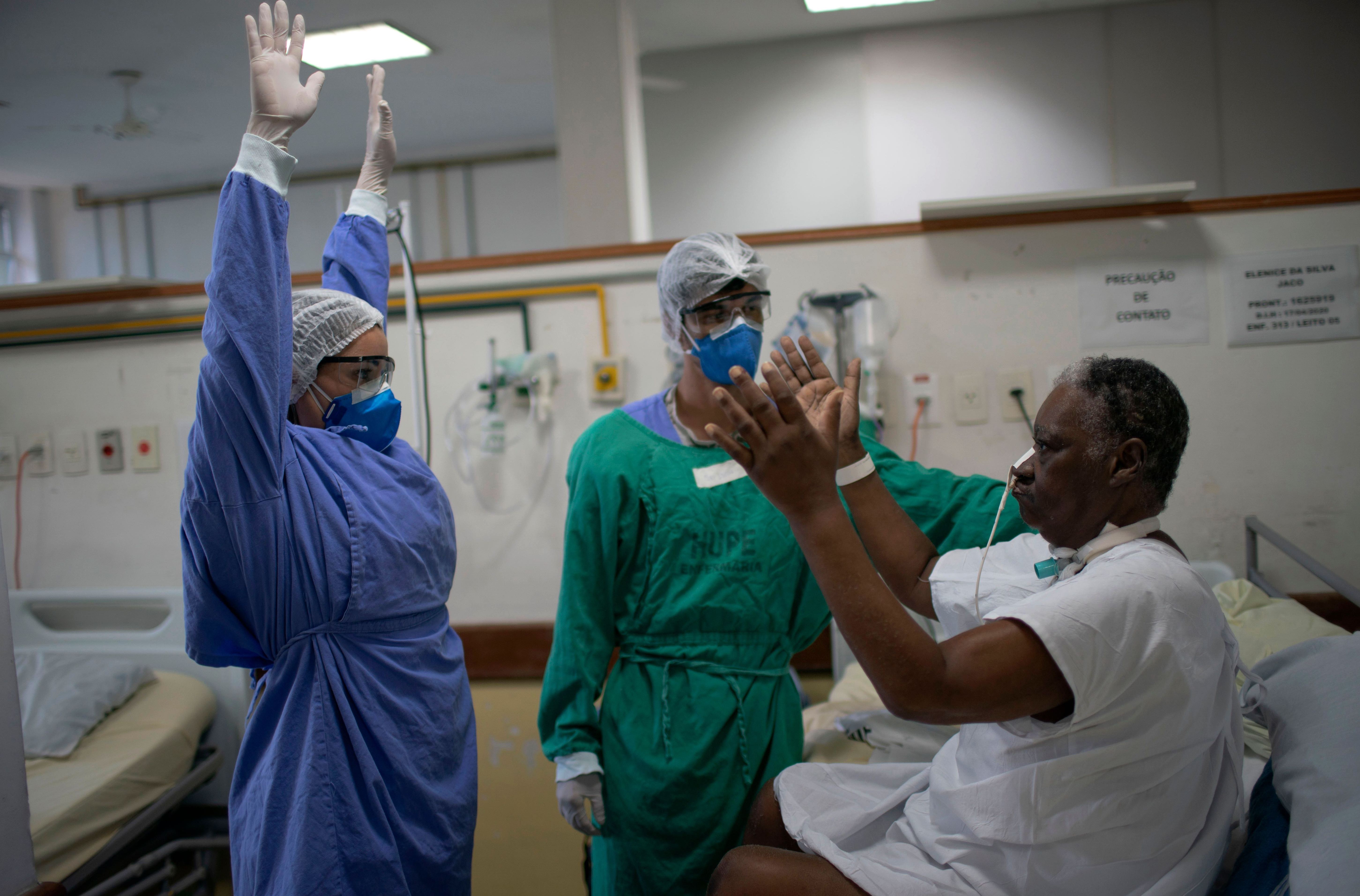
And physiotherapists are one key group working hard to help people throughout this pandemic.
Currently, there are more than 35,000 physiotherapists working in Australia and about one in five are working in a hospital on the frontline caring for patients with COVID-19. This work often begins in the intensive care unit (ICU), where the sickest of patients are cared for.
Most people with COVID-19 have no symptoms or only end up with a mild illness. But in Australia, 12 per cent of people are admitted to hospital and one in five of those individuals end up in ICU.

Health & Medicine
As a health worker, what’s my risk from COVID-19?
Globally, hospitalisation rates are much higher.
With more than 21 million confirmed COVID-19 infections globally, we’ve seen a massive surge in demand around the world for intensive care beds.
According to Lisa Beach, a senior intensive care physiotherapist at The Royal Melbourne Hospital, the physiotherapist’s role in intensive care is helping patients in their recovery after they have been critically unwell with COVID-19.
This involves patient assessment, goal setting as well as the prescription of mobility and rehabilitation treatments. To do this, physiotherapists work alongside a large multidisciplinary team.
Early rehabilitation and mobilisation involves helping to get patients up and moving, says Thomas Rollinson, a senior intensive care physiotherapist at Austin Health. He highlights how important it is to get patients up and moving and to facilitate their discharge from intensive care and hospital as quickly as possible.

According to the physiotherapists on the front line we’ve spoken to, they are seeing a range of people in hospital, from those in their early 30s through to people in their 80s.
Many of these people were previously fit and well, with no other health problems before getting COVID-19.

Health & Medicine
How to take care of yourself if you have COVID-19
Patients who end up in intensive care for a long period of time can become quite weak. An important part of a physiotherapist’s role is to help rehabilitate these patients. That means doing exercises, as well as sitting up and walking with these patients.
All of this while wearing personal protective equipment (PPE).
So, as Thomas Rollinson says it can get quite hot, sweaty and tiring, particularly when there are multiple patients requiring rehabilitation.
But a further key element of a physiotherapist’s role in intensive care is improving a patient’s lung function.
Many patients who have severe respiratory failure as a result of COVID-19 need to be on a breathing machine. Some require ‘proning’ – or turning them onto their tummy – which is a way to help people clear their lungs, as well as improve lung capacity and oxygen levels.
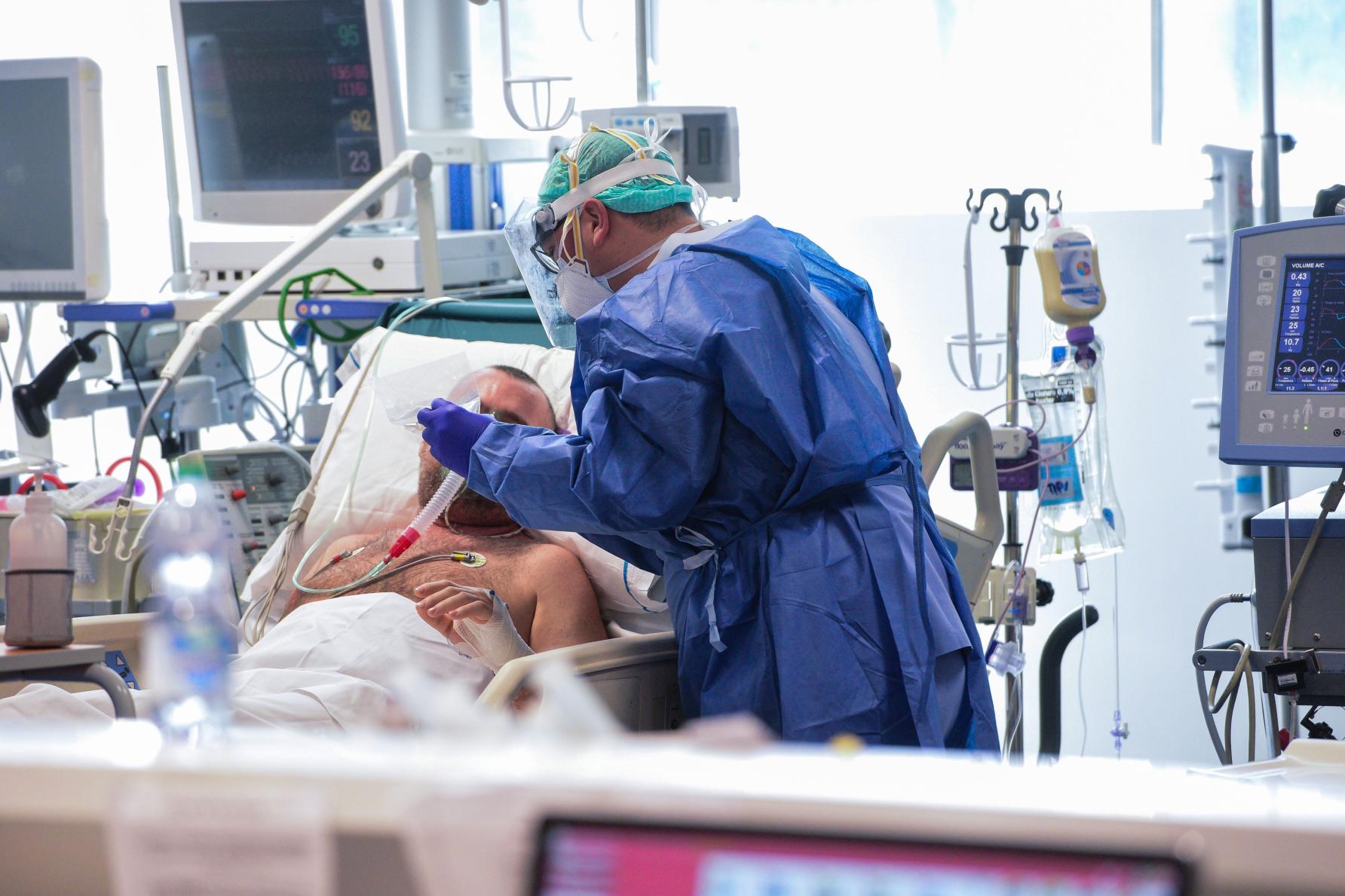
To do this, and to assist with the breathing machine, a patient is placed in a deep coma.
Proning is a difficult task that requires several members of the multidisciplinary team.
It’s a treatment that’s usually only used three to four times per year for patients with severe respiratory problems, but now in some hospitals, specific physiotherapy-led proning teams have been set up to help patients with COVID-19.

Business & Economics
More transparency needed in PPE supply chains
Although these treatments are very important in the severe stage of disease, they can contribute to greater muscle weakness and physical disability in the longer term.
For some patients, their muscle strength may have been relatively good despite being in the intensive care unit. But increasingly, we are seeing patients that are profoundly weak and unable to move their arms and legs.
For them, the road to recovery is much longer.
We do not yet fully understand the long-term health impacts from COVID-19.
But we do have a vast amount of research on the recovery patterns of patients who have been in intensive care with acute respiratory distress syndrome, a condition that is somewhat similar to what happens in the lungs of a patient with COVID-19.
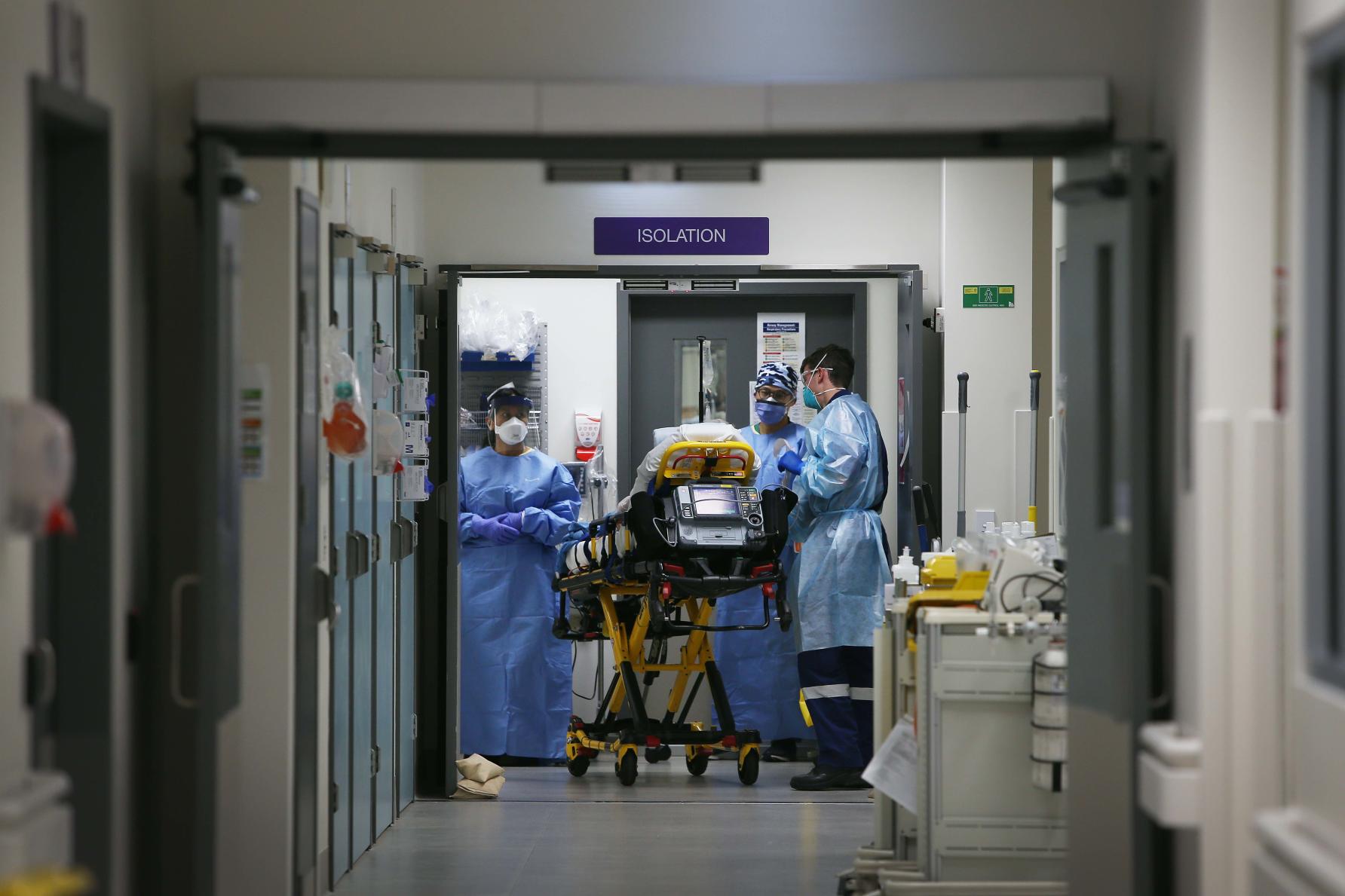
From this work, we know that patients who are in intensive care, in a coma and on a breathing machine for a long period of time, are more likely to suffer long-term problems from their critical illness.
This is referred to as Post Intensive Care Syndrome (PICS) which is the severe ongoing physical, cognitive and psychological consequences of critical illness. It can last for months or even years.
These problems start early in the intensive care stay.

Business & Economics
How are Australia’s doctors faring during COVID-19?
Patients can lose up to 20 per cent of their muscle bulk within the first week of being in intensive care and can be very weak when they wake up from the coma.
Rehabilitation begins as soon as possible in order to improve strength and mobility. It is recommended within clinical practice guidelines as an integral component of ICU care.
It has been less than a year since the first case of COVID-19 emerged. Around the world, researchers and clinicians are trying to understand what the path to recovery may look like.
Persistent fatigue, breathlessness and ongoing pain are recognised as some of the key challenges for the ‘COVID-19 long haulers’: those who have ongoing symptoms long after the initial positive test.
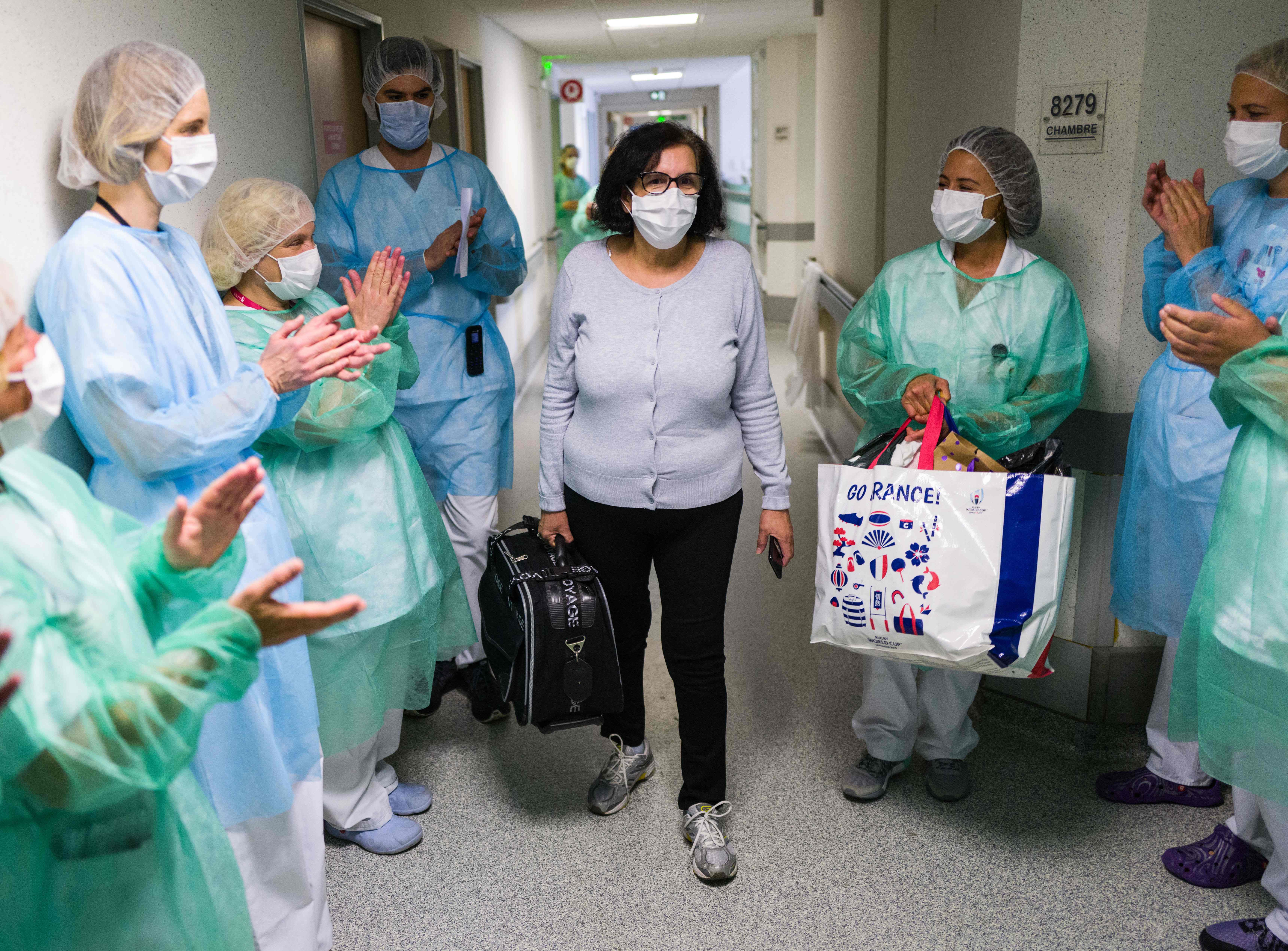
So, establishing how to support patients in the months after that is crucial.
Currently there is no standard dedicated rehabilitation pathway for intensive care patients after they leave hospital. So, it’s crucial to understand how we can ensure access to rehabilitation support beyond the hospital stay.
According to physios on the frontline, Thomas and Lisa, a number of our younger patients, who were working full-time and going to the gym pre COVID-19, are now suffering from fatigue just completing everyday tasks.
So, although they are out of hospital, they are still far from what is normal for them.
Also important is the human contact a physiotherapist can bring to a recovering patient. Even just being able to talk with patients while they do their exercises can help.
So, as the world negotiates the potential long-term effects of COVID-19, the role of a physiotherapist is crucial in helping patients recover and heal in one of the toughest time of their lives.
Banner: Getty Images