
Sciences & Technology
Why we show the whites of our eyes

As researchers refine the capabilities of bionic eyes, restoring sight to some blind people may be just around the corner. But what are the ethical implications of ‘artificial’ sight?
Published 5 December 2017
Curing blindness – at least in some of its many guises – with a prosthetic retina, also known as a bionic eye, has occupied researchers for more than a decade.
And they have come a long way. Bionic vision technology has already been able to restore a degree of visual perception in patients with age-related macula degeneration or retinitis pigmentosa, who are often rendered completely blind.
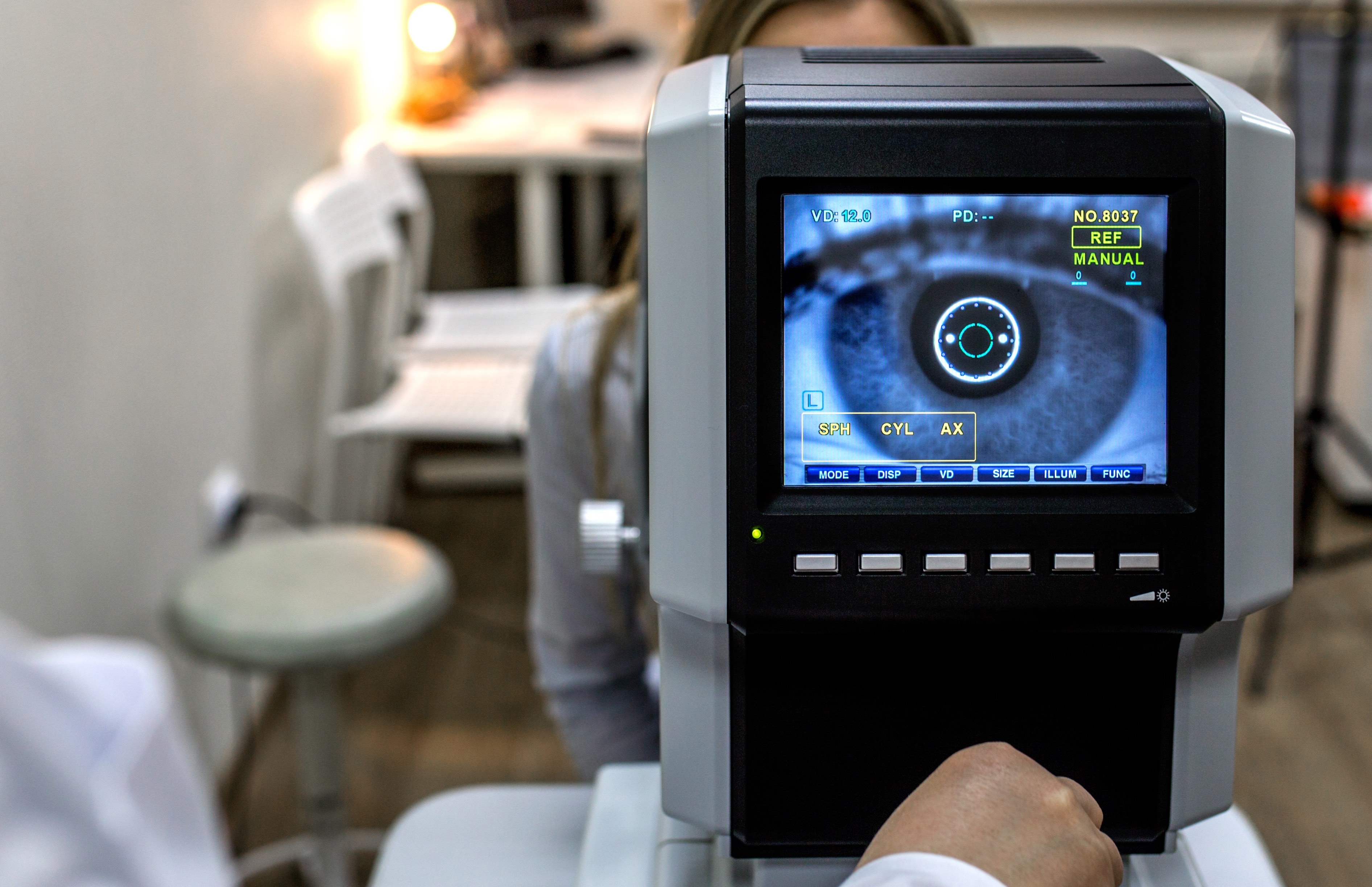
While the research remains in its infancy, it is likely to keep improving to the stage where a meaningful form of sight is restored for these patients in the not-too-distant future.
But what are the ethical implications of an electronic prosthesis replacing natural vision? What happens if the technology goes wrong and patients’ visual perception is distorted or altogether misleading? And who is responsible for high-impact decisions?
Retinal prostheses work by electrically stimulating the retina, essentially doing the job of the photoreceptors that are killed off by disease.

Sciences & Technology
Why we show the whites of our eyes
The ‘sight’ they currently provide is heavily limited and usually manifests as small, grey-scale flashes of light that loosely correlate to the presence of objects in the central visual field. This in itself is a remarkable achievement of neuroscience but unfortunately patients usually remain in a heavily debilitated state, unable to distinguish between faces, numbers, read fine text, or make high order decisions autonomously.
But Dr Matthew Petoe from the Bionics Institute in Melbourne says patients may soon be able to navigate without the use of a guide dog and recognise distinct facial expressions. The exact nature of the stimulation requirements for these sorts of outcomes remains unclear, but he is certain bionic vision will continue to improve at a rapid pace.
Based on only a limited number of clinical trials of bionic eyes, it’s difficult to say how open to misinterpretation the patient’s perception may be. And therein lies the problem. The future of bionic vision represents a potential infringement upon individual autonomy to an unknown degree.
Of course a more functional bionic eye will lead to greater autonomy overall but at what cost? It isn’t good enough to offer an improvement to a diseased person’s quality of life if that improvement goes hand in hand with a newly imposed risk of suffering.
For example, the inability of patients to distinguish between numbers and read fine text means that misinterpretation could result in material losses beyond their control when managing their finances.

Additionally, misinterpreting facial expressions may skew a person’s judgement in a social context and misreading crucial information like street signs could put them in harm's way. At the time of interpreting these perceptions, patients will have no way of knowing how truthful a representation of reality their prosthetically induced perception actually is.
One of the difficulties in making bionic vision more naturalistic is the wide range of diseases that warrant a bionic eye, as well as the number of differences in psychophysical responses to a given stimulus. That is to say, different people respond differently to the same thing.
It is likely the risk of misinterpretation and perceptual distortion won’t be the same for everyone.

Sciences & Technology
Laser device will see what the eyes cannot
Cellular gene therapy is an alternative approach to treating retinal degeneration that is tailored to the individual and may therefore be robust against the sorts of inherent ethical complications associated with retinal prostheses.
However, while acknowledging the successes of gene therapy, Professor Michael Ibbotson, director of the National Vision Research Institute says “it is unlikely to solve all neurological issues. There is very likely to be a need for bionics”.
It is then incumbent upon the neuroscientists and biomedical engineers recently tasked with the development of an Australian made bionic eye, to consider their ethical responsibilities. As with any new technology, there is a risk that it will be used malevolently and to influence the behaviour of vulnerable populations.
The ethical future of bionic vision is somewhat cloudy, but Professor Ibbotson and others at the Bionics Institute who have been strong proponents for the advancement of bionic vision in Australia maintain there is an ethically justifiable balance of benefit and risk.
Blindness due to retinal degeneration is a profound challenge, not to mention a hefty public health burden.
One in 12 Australian adults will experience macula degeneration in their lives and to date, bionic devices have shown by far the greatest promise of any treatment option in being able to help these individuals to fully experience the world once again.
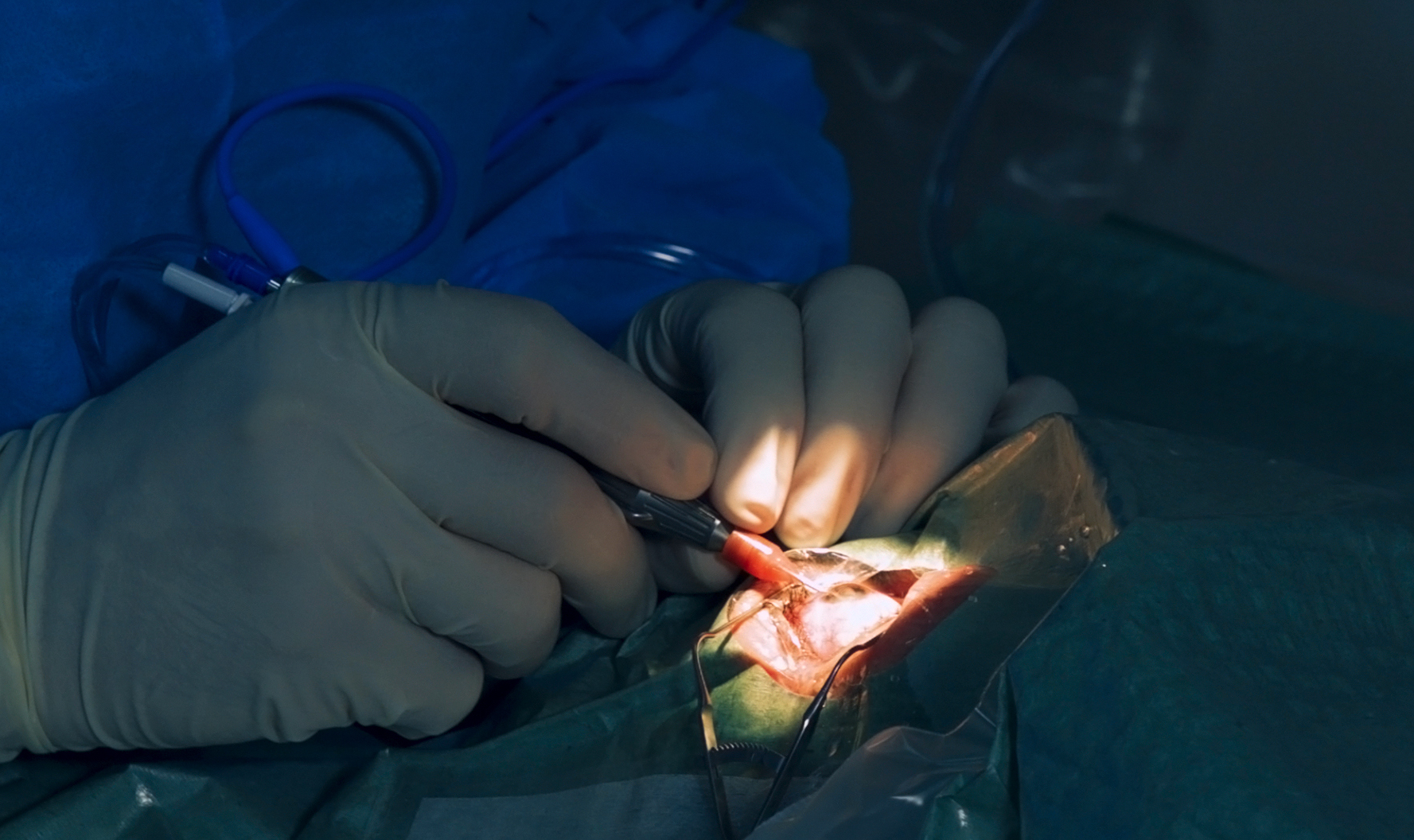
A healthy dose of scepticism surrounds the development of brain interface technology, as it becomes a more common research topic. These devices, which include prosthetic limbs, have the potential to greatly assist disabled people.
Developing and making accessible a bionic eye absent of any serious ethical violations would greatly enhance public acceptance and enthusiasm towards the development of bionics that could do wonders for people in need.
Banner: iStock