Sciences & Technology
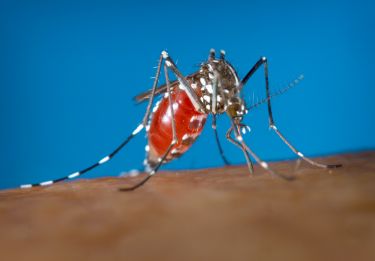
Using bacteria to control mosquitoes
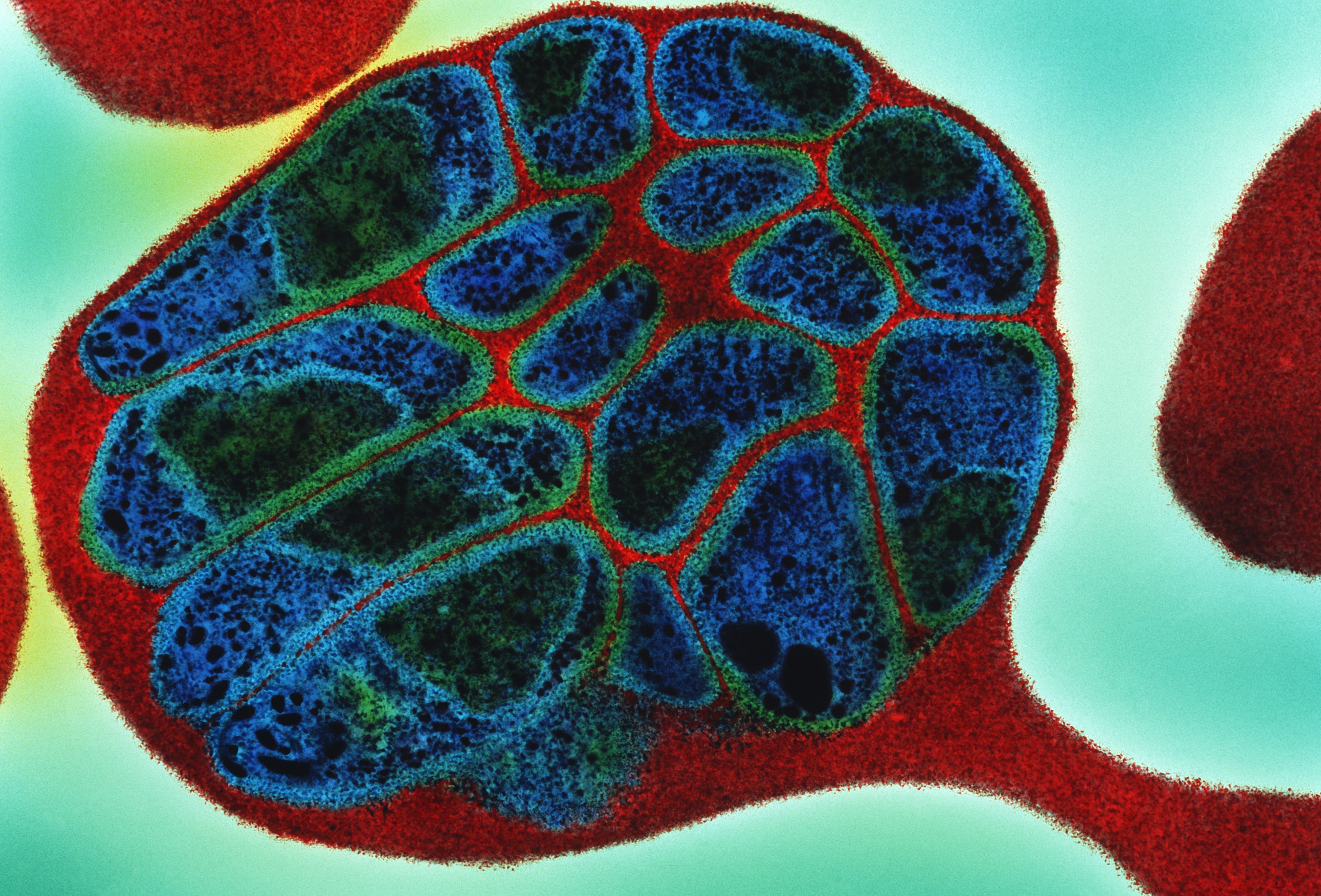
New research exploring our body’s inflammation response to malaria could open up new avenues for treating chronic viral infections and autoimmune diseases like HIV
Published 21 November 2019
Malaria remains one of the most harmful infectious diseases affecting humans.
The disease, which is caused by Plasmodium parasites, still results in more than 200 million clinical cases each year around the world, and many more that are asymptomatic or undocumented. Young children and women are particularly susceptible.

Symptoms of malaria range from fever to complicated syndromes including severe anaemia, acute respiratory distress, renal failure, seizures and coma.
These are a result of the parasite itself, but also a consequence of the body’s severe inflammatory response to malaria infection.
Malaria is fascinating for its ability to fly under the radar of the host immune system. Unlike many viral and bacterial infections, like measles or tetanus, which can induce lifelong protection after a single exposure, immunity to malaria is strikingly less efficient.

Sciences & Technology
Using bacteria to control mosquitoes
Our team has spent more than 10 years trying to understand why people living in malaria endemic areas must be continuously exposed to malaria, usually for decades, before they eventually develop immunity.
But even this immunity is still not fully protective – it simply prevents episodes by substantially reducing parasite burden in the blood, that is the number and virulence of infecting parasites.
So, a patient experiences debilitating symptoms for many years then continues to be infected, just without obvious clinical symptoms.
They can, however, still carry and transmit the parasite.
So, what makes malaria so different to these other diseases, where a single exposure confers immunity for life?

Antibodies are critical to the immune system’s ability to develop long-term immunity to many infections.
In 2016, my team showed that inflammatory molecules ‘sabotage’ the body’s ability to protect itself by hampering the action of helper T cells.
Helper T cells work hand-in-hand with B cells, activating and training them to produce potent antibodies that are highly specific for an invading pathogen.

Sciences & Technology
The genes that turn malaria into a killer
In our previous paper, we found that inflammatory signals activated molecules that arrested the development of helper T cells.
This meant that B cells did not get the necessary instructions to make antibodies, and the entire antibody response was reduced.
So, when we began this study looking at the effect of inflammatory signals on B cells, we expected to see this again.
But, in fact, opposite is true. The inflammatory signals were improving the quality of the antibodies produced.
Inflammatory signals increased by the action of a protein called T-bet, encoded by the Tbx21 gene, sent the B cells to an elite training ground – the dark zone of germinal centres in immune tissues.
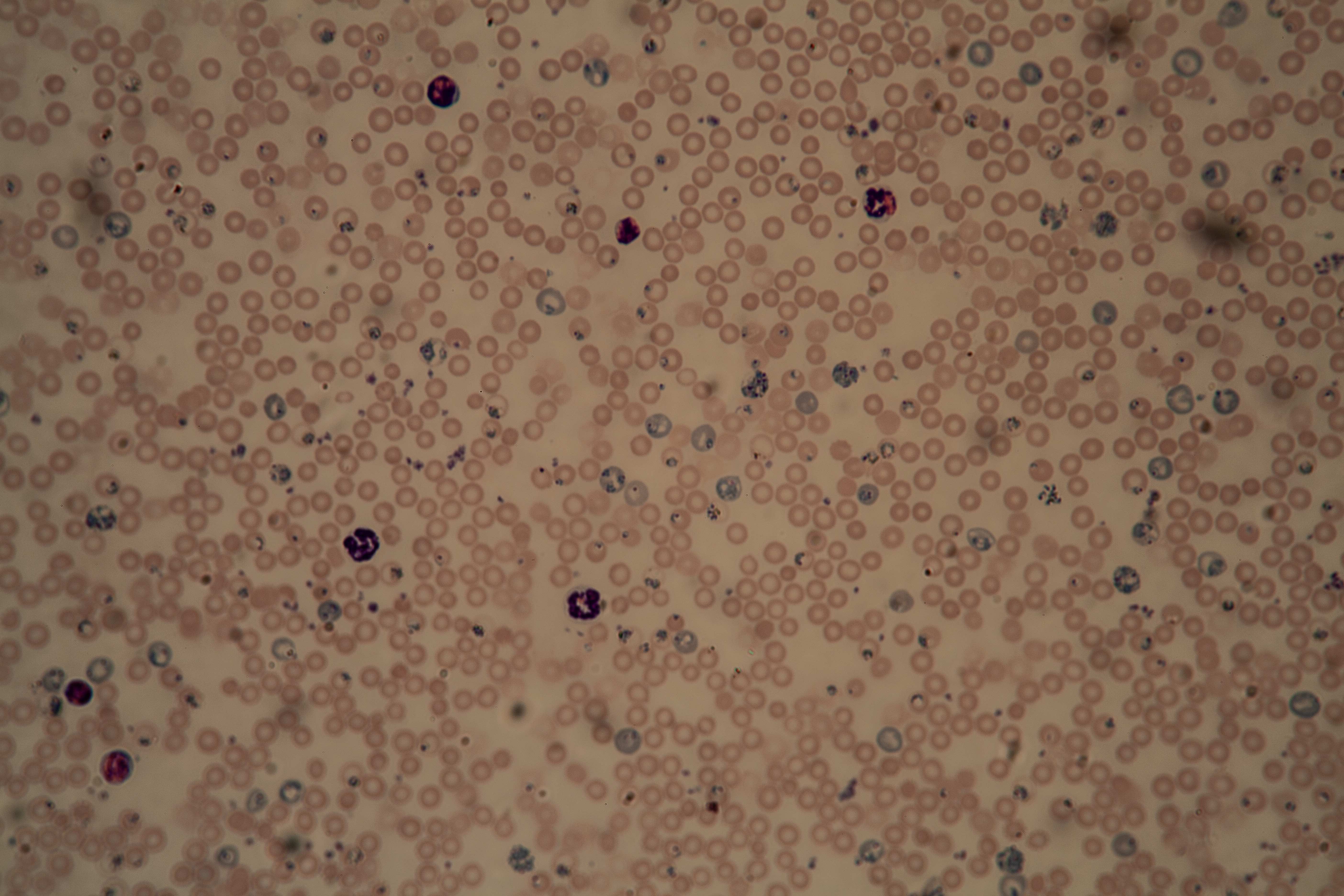
There, they underwent an exhaustive program to acquire the capacity to bind to malaria parasites – effectively becoming professional disease fighters.
Overall, these studies indicate that while inflammatory signals govern the ‘magnitude’ of the antibody response by the development of helper T cells, its expression in B cells controls the quality of the antibody response.
Our research helps explain what is happening in malaria.

Sciences & Technology
Malaria’s dark secrets exposed by a simple glow
The inflammatory reaction to the parasite diminishes the activity of helper T cells and hinders effective control of the infection in the short term.
But, over long periods of time, enough B cells that make highly potent antibodies are generated to keep the parasites at bay, at least enough to prevent clinical symptoms.
One of the reasons this discovery is so exciting is because it goes beyond malaria alone.
With this knowledge, we have the opportunity to explore new avenues for treating chronic viral infections and autoimmune disease.

In chronic viral infections like HIV and chronic hepatitis C, producing very high quality, potent antibodies is critical for clearing the infection.
On the flip side, B cells that are primed to make antibodies that target self-antigens – our body’s own proteins and tissues – are incredibly destructive, leading to autoimmune diseases such as lupus.
If we can target the molecular ‘switch’ that drives the immune system to produce highly-potent antibodies, or other molecules in the same pathway, we could offer a more ‘precision medicine’ approach to treating these diseases than currently exists.

Sciences & Technology
Waiting for the Tiger mosquito
We know that the molecular switch that we have identified in B cells during malaria infection is also found in B cells of people experiencing chronic viral infections or lupus.
The hope is that our new research could lead us to design new vaccines or therapies that would ‘switch on’ molecules that help to produce these elite B cells to fight chronic infections better –or ‘switch off’ the same molecules in autoimmune diseases to stop the production of B cells.
But it gives us a fascinating insight into the way the human body – and our professional fighting cells – could potentially offer us a way to combat autoimmune diseases and viruses like HIV in the future.
Banner: Getty Images