Health & Medicine
Gaining clarity on the ethical issues of a possible COVID-19 vaccine
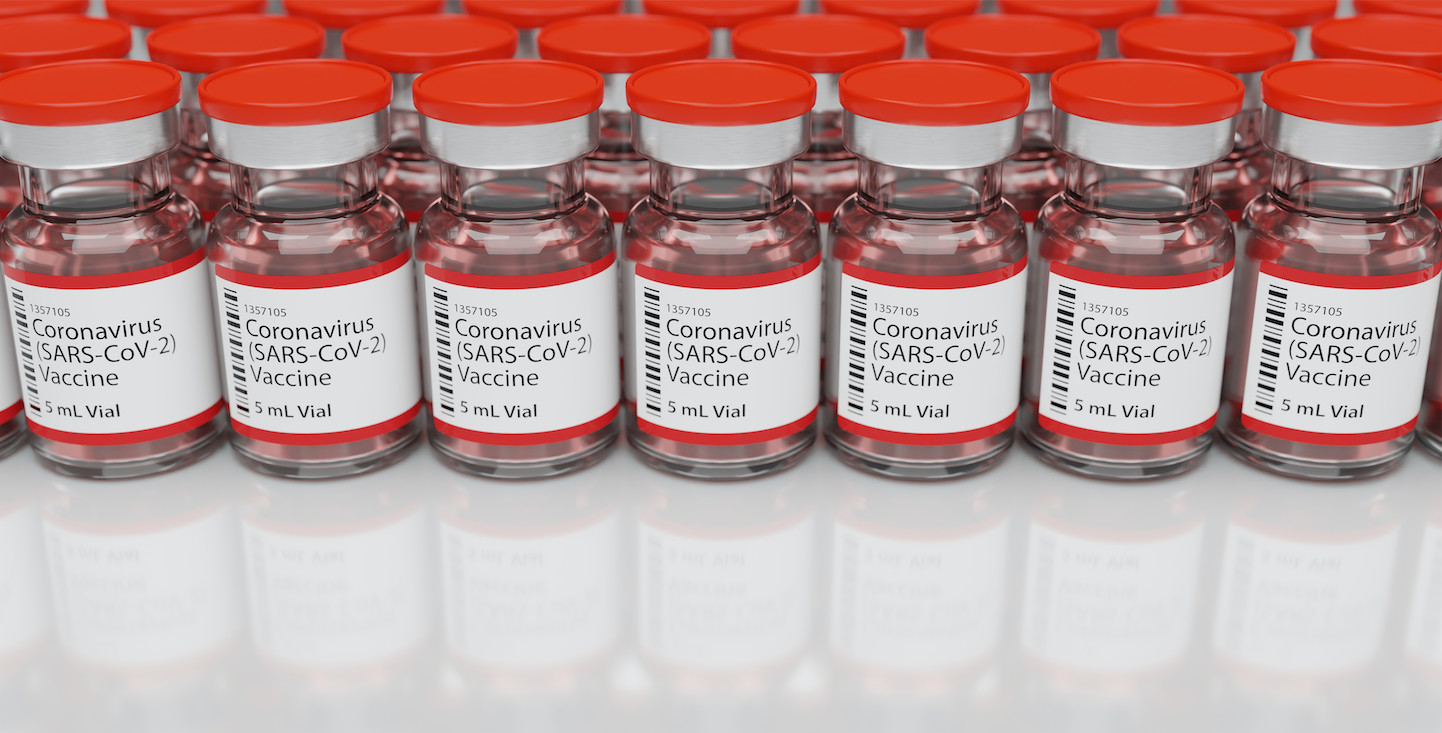
History will judge “terribly” any country which finds a COVID-19 vaccine but does not share it, says Prime Minister Scott Morrison. How do we ensure this doesn’t happen?
Published 9 September 2020
The race is on to produce a COVID-19 vaccine.
Although the trial is currently paused, the University of Oxford and AstraZeneca have said they could put a vaccine before regulators this year. In Australia, human trials of a potential vaccine developed by the University of Queensland began in July.

But as the world waits for a vaccine to become available, steps need to be taken to ensure that when that vaccine arrives, it is available to all. And this requires looking closely at the issue of patents.

Health & Medicine
Gaining clarity on the ethical issues of a possible COVID-19 vaccine
In the fight to provide immunity from COVID-19, those who would ban patents on vaccines may prove more dangerous than those who would ban vaccinations. Whereas ‘anti-vaxxers’ rely on ignorance and fear to push their case, the anti-patent brigade uses logic – making their argument potentially more persuasive.
Economics tells us that the exclusive rights provided by a patent makes the patent holder a monopolist over the invention. Monopolists reap monopoly profits. They sell at artificially high prices by restricting production.
And where production is restricted, the invention will be available only to those people most able to afford it.
In the case of a patented vaccine, this means that only people in rich countries will get access and so enjoy immunity from a virus responsible for more than 890,000 deaths worldwide as of 8th September, 2020.
According to this logic, to ensure availability to all, we must not grant patents on COVID-19 vaccines. But the problem with this message is that it only represents part of the story.

Health & Medicine
The science behind the search for a COVID-19 vaccine
The missing element is the understanding that by providing an inventor with exclusive rights, a patent can actually make it easier – not harder – to ensure the widest availability of the invention.
Patents are not absolute. All countries have the ability to ‘bust’ the patent monopoly by compulsorily taking a licence to the invention. For example, Australia has a Crown use provision in its patent legislation that allows a government to make, use and sell a patented invention “for the services of the Commonwealth or the State”.
Clearly, a government can override a COVID-19 vaccine patent to ensure that Australians have access to the vaccine. But such a provision can only apply where there is a patent to override.
You might think that where there is no patent then there is nothing to stop a government, or anyone else, from freely making the vaccine. But this presupposes that they have the necessary information to be able to do so.

A patent is a two-sided bargain. In return for obtaining a time-limited monopoly, the inventor must disclose the invention so that others know how to make it. Where there is no patent, there may be no disclosure and the inventor can instead keep crucial information secret.

Health & Medicine
A remedy for false COVID-19 cures?
Even where the necessary information is available, not every country will have the technical capacity to make the vaccine. And even where they do, a vaccine costs money to make.
So countries that can make the vaccine will have to do so for the countries that can’t, and they will have to supply the vaccine at a subsidised price.
Unfortunately, sometimes unscrupulous distributors or corrupt governments in poorer countries take advantage of the willingness of citizens in richer countries to pay a higher price for medicines.
The danger is that a subsidised vaccine supplied to a poor country may end up being exported to richer countries for profit, instead of being given to its citizens.
A patent can help prevent this. The patent holder can stop such ‘leakage’ by exercising their exclusive right of importation.

The international community is alert to the problem of inequitable access to medicines. For a decade, the UN-backed Medicines Patent Pool (MPP) has arranged for patent holders to deposit their patents into a pool from which voluntary licences are granted to manufacturers in poorer countries.
The MPP increases access to, and facilitates the development of, life-saving medicines for low and middle-income countries. To date, it has agreements for HIV antiretroviral medications and hepatitis C and tuberculosis treatments.
The WHO recently announced that it will use this model to ensure access to COVID-19 vaccine patents. But clearly, a patent pool only works when there are patents to deposit into it.
No-one disagrees that a COVID-19 vaccine must be available to all who need it - not just to those who can afford it. But in tackling that concern, patents need to be seen as part of the solution and not as part of the problem.
Banner: Shutterstock