
Politics & Society
Chemical restraint: Behind locked doors

Secluding, physically restraining or overmedicating people experiencing mental health crises still happens, but countries around the world are trialling successful alternatives
Published 7 October 2018
Controlling the behaviour of people experiencing mental health crises by strapping them into beds or chairs or overmedicating them may seem like something that would happen elsewhere, or in the past.
Yet it sometimes happens here in Australia in 2018, and may even be permitted under mental health laws.

While most Australians who experience mental health conditions can seek help on a voluntary basis, legislation does allow for people with severe mental health conditions to be compulsorily detained and treated - regardless of their wishes.
Unsurprisingly, when treatment without consent is combined with closed environments, coercive practices and human rights abuses can become the norm.
Consider Robert Spriggs, for example. His story emerged during inquiries into practices at the Oakden Older Persons Mental Health Service in South Australia.

Politics & Society
Chemical restraint: Behind locked doors
Shortly after being admitted to Oakden in 2015, the 66-year-old Mr Spriggs was taken to Royal Adelaide Hospital with significant and unexplained bruising on his hip and thighs.
His family later learned he had been given 500 milligrams of the anti-psychotic drug Seroquel, instead of the prescribed 50 milligrams. The bruising was likely caused by his being strapped to a chair.
South Australia’s Chief Psychiatrist issued a damning report, pointing to the “ongoing [and] repeated use” of practices like strapping people into chairs and overmedicating them in ways that were “likely implemented for staff convenience and or used as punishment”.
The scandal also gave rise to a report by South Australia’s Independent Commissioner Against Corruption and the Senate Community Affairs Reference Committee.
Our research examines ways of avoiding coercive practices to ensure people experiencing mental health crises are treated with dignity and respect.
Most recently, we undertook a systematic review of global practices that aim to reduce, prevent and end coercive practices in mental health settings.

The review was commissioned by the United Nations Office in Geneva. It will inform a report of the United Nations Special Rapporteur on the Rights of Persons with Disabilities, whose role is to promote the human rights of persons with disabilities worldwide.
We found that when governments, service-providers, courts and communities take concerted action to move away from coercive practices, they are almost always successful.

Health & Medicine
Time to hold back on the use of restraints
While practices like seclusion, physical force, using belts or straps to restrict movement or medication to control behaviour are arguably justified in extreme circumstances to prevent harm to the person or to others, according to a World Health Organization report, they are counter-therapeutic.
Coercive practices can impede people’s recovery and re-traumatise those who have previously experienced sexual and physical abuse.
We wanted to know whether they can be avoided altogether and we found many examples from around the world where they are.
In the Netherlands, for example, a national policy that aimed to reduce rates of seclusion in mental health settings reportedly resulted in an average reduction of yearly seclusion incidents by nine per cent.
In China, a national policy designed to stop people with mental health conditions being ‘shackled’ in family homes and villages, reportedly had a 92 per cent success rate.
Within hospitals, the Six Core Strategies to Reduce the Use of Seclusion and Restraint is prominent, and has been successfully applied in the United States, Canada, Australia and New Zealand.

The initiative includes strategic use of data, leadership, workforce development, service user roles in inpatient settings, and the use of targeted tools to reduce incidents of restraint and seclusion in mental health settings.
Some practices were led by people who have themselves used mental health services. An Australian study, for example, looked at an initiative in a hospital in the Australian Capital Territory where the Six Core Strategies were applied. Seclusion incident rates reportedly fell from 6.9 per cent to less than one per cent over a two-year period.
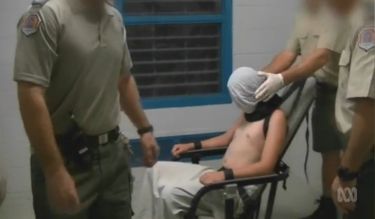
Politics & Society
Four Corners: Using restraints can be called torture
Other countries, like New Zealand, the United States and Germany, have seen the proliferation of service user-led crisis respite homes, with promising results.
Some unexpected findings emerged from the review.
Certain assumptions in mental health care practice were challenged, such as the notion that psychiatric wards need to be locked. This assumption is based on a belief that locked doors prevent people from absconding, attempting suicide or dying by suicide.
German researchers who examined around 350,000 admissions to 21 hospitals over a 15-year period, concluded that “there is insufficient evidence that treatment on locked wards can effectively prevent these outcomes”.
In fact, their research suggests the opposite. Open wards were associated with a decreased probability of suicide attempts, absconding with return, and absconding without return. However, open wards did not appear to affect rates of death by suicide.
An Italian study reported on an “open door… no restraint system of care for recovery and citizenship” in the city of Trieste. According to the author, Trieste’s mental health system “changed from a clinical model based on treating illness to a wider concept of mental health that looks at the whole person and [his or her] social background”.
These examples provide a glimpse into the many global initiatives that aim to provide high-quality healthcare that is non-intrusive, service user-led and preferred by local groups.
Our review highlights a broad suite of practices, policies and interventions with a strong evidence base. No single country or region has implemented the full range of measures to reduce and eliminate coercive practices.
Perhaps, in order to avoid another Oakden scandal - it’s time to find out what would happen if they did.
Banner image: Shutterstock