
Health & Medicine
Reading the body’s electrical signals to treat illness
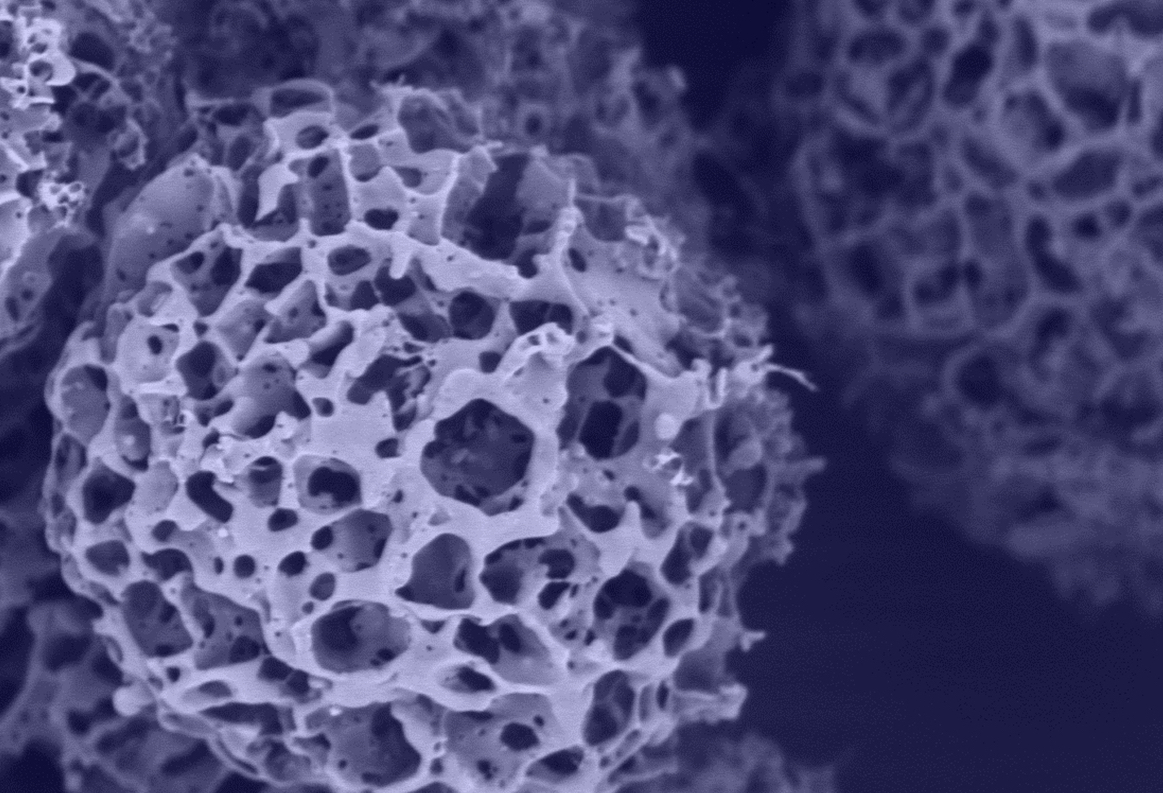
Tissue engineering can restore damaged or lost tissue in the human body, and biomedical engineers are working to one day scale up the technology to regenerate entire organs
Published 26 August 2019
Tissue engineering is still a relatively new field in regenerative medicine but an important one. It’s working to restore or substitute damaged or lost tissue in the human body.
Although the research field is only 25 years old, which is nothing in terms of the lifetime of engineering innovations, major breakthroughs in tissue engineering are paving the path to innovative medical treatments.
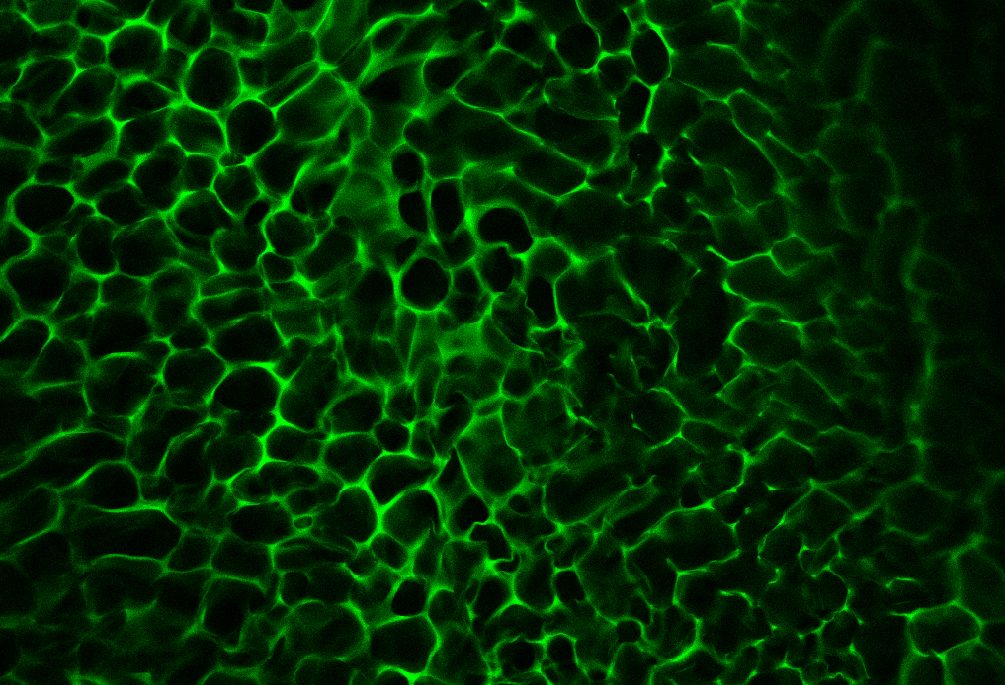
Aside from blood, the human body is primarily made up of tissues, ranging from the smallest components through to entire organs.
While current research can create tissues at a micro scale of less than half a millimetre, the idea is that tissue engineering could one day scale up to include structures as large as a human liver or lung.
Professor Andrea O’Connor can still remember the first time she heard of tissue engineering.

Health & Medicine
Reading the body’s electrical signals to treat illness
“One of the surgeons walked down the hallway of the chemical engineering department asking if someone could make a scaffold to support growing tissue. He’d read a paper on it and figured he needed engineering input”, she says.
It was this moment that ultimately propelled her to her position today as head of Biomedical Engineering at Melbourne School of Engineering.
One key project she is involved in aims to regenerate one small, specific tissue in the eyelid with benefits for patients who have had surgery to remove part of their eyelid due to conditions like melanoma.
The mechanical properties of this tissue are critical to the function and shape of the eyelid and so careful engineering is needed even though it’s quite small. Currently, surgeons don’t have perfect materials to replace this tissue, so the prospect of growing replacement tissue with the right properties for this purpose is exciting.
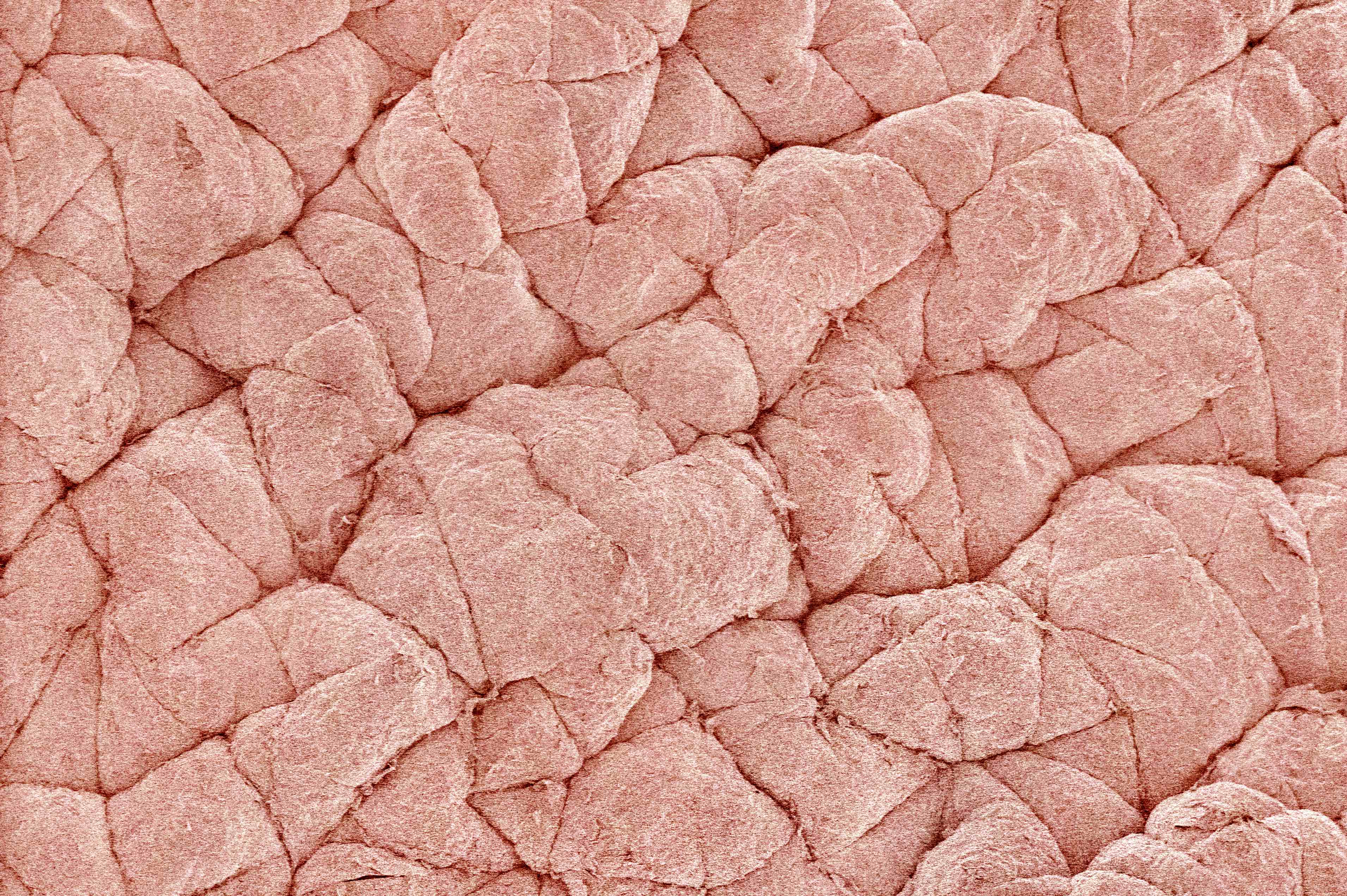
Tissue engineering focuses on restoring the functions of our tissues like the structural strength of bones, the hormone production of the pancreas and the protective barrier functions of the skin .
But, the outcome of this research could mean more personalised options for patients, with the new tissue specifically engineered for their body, as well as reductions in the need for animal testing.
Professor O’Connor’s most recent research is investigating forming tissues by applying forces to cells.
Health & Medicine
Putting cells through their paces
Her research focuses on the control and understanding of cell interactions using a technique that manipulates cells to form 3D structures called cell constructs, or spheroids.
This is done by attaching magnetic particles to cells and applying magnetic forces that bring them together into clusters, or aggregates.
Under the right conditions, once these cells get close enough, they secrete certain protein and sugar-based molecules that help them to stick together.
Using magnetic fields to generate an external force, rather than traditional methods like using centrifugal forces, speeds up the process and results in good contact between the cells.
These structures have high cell densities and their shape can be easily controlled by changing the magnetic field patterns.
This ultimately leads to better control over 3D construct production.
Fusion of these spheroids into larger constructs can also be achieved using magnetic forces, which could potentially lead to engineering more complicated structures in the future.
Health & Medicine
Organoids: the next revolution in human biology has begun
Unlike typical 3D printing, where cells are mechanically forced through a tiny nozzle, Professor O’Connor’s new magnetic method exerts gentle forces on the cells. It also means this force can be applied over an extended period, making it possible to move cells around while they are growing in the laboratory.
Alongside these advancements in tissue engineering, the materials we use have also taken a leap forward. For example, hydrogels, which have come a long way in a short space of time.
In the area of tissue engineering, hydrogels are used as a medium to transfer and host cell structures during growth and for transplantation.
Professor O’Connor’s research into the regeneration of eyelid tissue used a hydrogel made from the waste shells of crustaceans.
The resulting material after some processing is called chitosan, a sugar-based molecule which has chemistry very similar to the molecules in our body. That means it is more biomimetic – mimicking aspects of the biological materials in our bodies.
As a result, it naturally degrades over time after the tissue is transplanted leaving no residue in the body.
“The material is processed into a porous sponge (made from hydrogel) with holes the right size for cells, providing a biomimetic environment for cells to stay alive and function”, says Professor O’Connor.
Professor O’Connor has also worked with breast tissue reconstruction which progressed to a clinical trial with collaborators at the O’Brien Institute and St Vincent’s Hospital, Melbourne.
Health & Medicine
Why can’t we cure cancer?
In that study, the patient’s own fat tissue was used to replace missing breast tissue for women who had breast cancer. The process involved using a custom-made chamber that was implanted in the patient’s chest with a blood vessel from the area.
A small amount of the patient’s own tissue was included in the chamber as a starting point for growing replacement tissue. This allowed healthy vascular fat tissue to grow and fill up the chamber.
Many of these new techniques used in medical treatments are a result of a burgeoning biomedical engineering sector.
While significant progress has been made in a short time, it’s only through interdisciplinary collaborations including those of biomedical engineers like Professor O’Connor and her colleagues that new possibilities are being realised for the future benefit of patients.
Banner image: Supplied