
Arts & Culture
Running on rainbows

There’s a growing tendency to link mental health and wellbeing as an inseparable conceptual couple, but the two concepts have very different connotations
Published 19 July 2021
Mental health and wellbeing are in our cultural spotlight as never before.
The psychological toll of the COVID-19 pandemic has been front of mind for the past year, but that concern is superimposed on others that preceded it.

We worry about rising mental ill-health among the young, increasing suicide rates and deficiencies in the mental health system. Hand-in-hand with these concerns, we’re seeing a growing supply of wellbeing initiatives in companies, universities and schools – all promising enhanced wellness and resiliency.
And, increasingly, mental health and wellbeing are presented as an inseparable conceptual couple.
Australia has its National Survey of Mental Health and Wellbeing and the two concepts are paired in the Australian government’s pandemic response plan and in its healthdirect advice service.
They sit-by-side in the Victorian Department of Education and Training statements about schools. They are conjoined online on the sites of numerous universities, health organisations, government units, and research projects.
The growing tendency to treat mental health and wellbeing as interchangeable ideas reflects the adoption of expansive definitions of mental health.
Keen not to present mental health as simply the absence of mental illness, the World Health Organization (WHO) defines it as “a state of wellbeing” in which people can successfully cope with stress, work effectively, contribute to their communities, and realise their potential.
The Australian organisation Everymind agrees, defining mental health as “a positive concept related to the social and emotional wellbeing of individuals and communities”.

The distinction between mental health and wellbeing may have become hazy, but the two concepts have very different connotations.
The WHO may align mental health with wellness, but mental health remains strongly tied to ideas of mental illness. The distinction between mental health and wellbeing is compelling and it has some important implications.
One way to explore the different meanings of wellbeing and mental health is studying people’s mental associations with the two concepts.

Arts & Culture
Running on rainbows
Small World of Words, a resource developed by Dr Simon De Deyne and his team, provides the tools to do so.
The English version contains associations for more than 15,000 words made by over 100,000 people. This massive data set allows us to explore the cultural meanings of concepts by examining the words people most commonly associate with each one, and to visualise those associations.
Let’s look first at the associations for wellbeing.
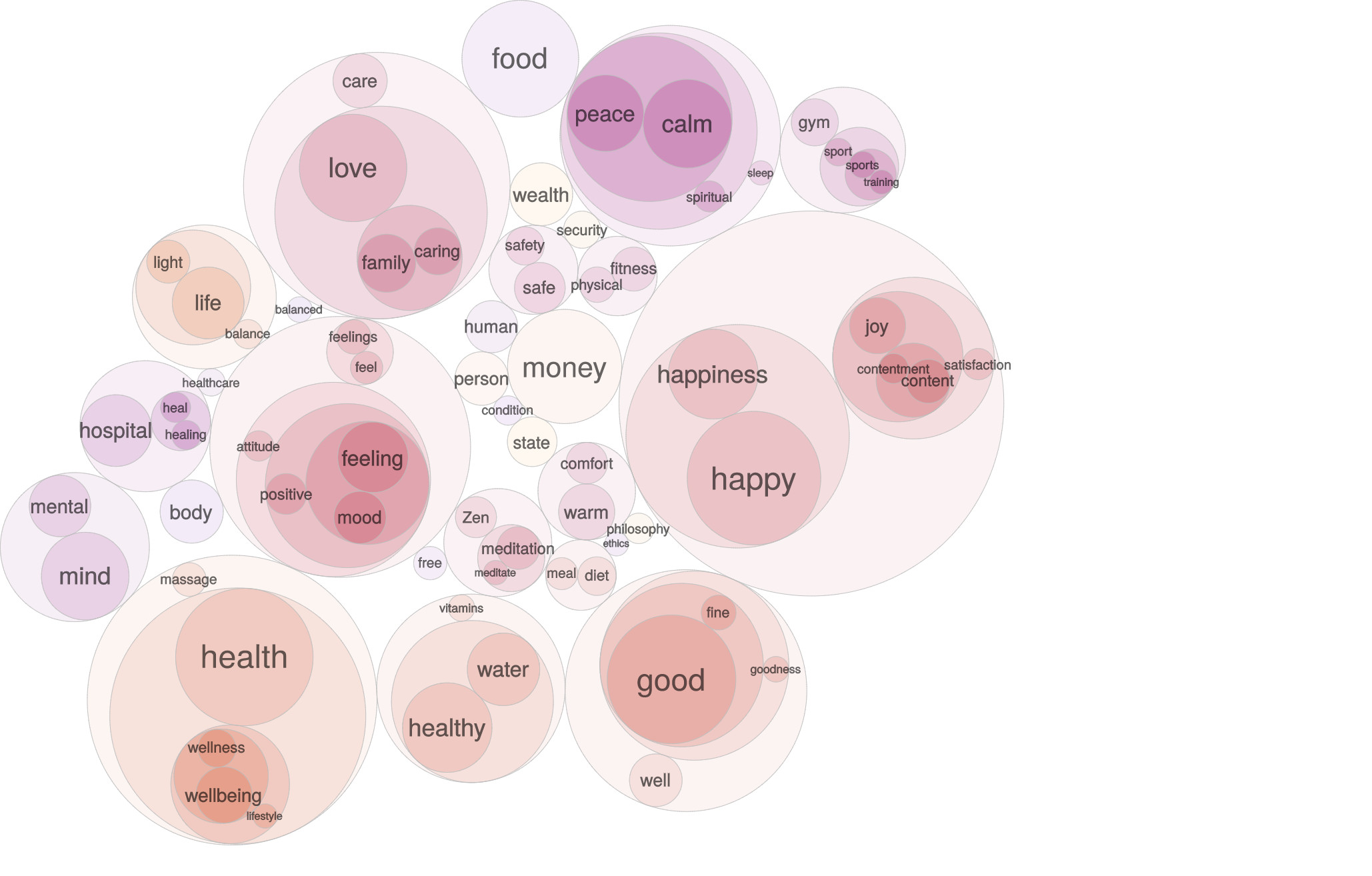
The larger circles represent more strongly associated words, and the circle colours identify clusters of related ones. Wellbeing is associated with goodness, health, love, happiness, peace, and things that might promote wellbeing, like money and food.
Wellbeing is a node in a network of positivity.
Now let’s look at the associations for mental health.

Despite the fact it’s ostensibly a form of health, the concept is primarily associated with sickness and disease, and with medical treatments and professionals.
It’s linked to suffering (depression, anxiety, stress), to psychiatric diagnoses (schizophrenia, bipolar) and to stigmatising labels, like ‘crazy’ and ‘insane’.
Although it has weak connections to ideas of happiness, calm and health, people think of mental health mainly in relation to illness, not wellness, and they embed it in a network of negativity.

Arts & Culture
There is no ‘normal’
Mental health and wellbeing don’t only differ in our mental associations.
Research by the likes of American sociologist Professor Corey Keyes tells us that they are also distinct in our experiences.
The team assessed large samples of adults using diverse measures of wellbeing – like positive emotions, life satisfaction and a sense of meaning and purpose, as well as measures of mental health problems – like depression and anxiety.

They found that people differ along two underlying dimensions, one corresponding to degrees of positive wellbeing and the other to degrees of mental illness.
Although these dimensions are separate, they are negatively related. Having a mental illness is not the same as having low wellbeing, although these states often go together.
Professor Keyes then constructed a model of the ‘mental health continuum’. At one end of the continuum are people who lack positive wellbeing, a state he calls “languishing” and also experiencing a mental illness.

Arts & Culture
Hey Siri, how’s my mental health?
At the other end of the spectrum are people who score high on positive wellbeing and who do not have a mental illness. Professor Keyes calls these fortunate folk “completely mentally healthy”.
In between these extremes are people who have a mental illness, but who are not languishing, and people who are languishing but do not have a mental illness.
By showing that this broad definition of mental health fuses two distinct dimensions – absence of mental illness and presence of positive wellbeing – Professor Keyes’ work also points to a problem with the broad definition.
People who lack or lose positive wellbeing – languishers – can be seen as having problems with their mental health, even if they do not have a mental disorder. Languishing is not mental illness, but when we view it through the illness-coloured lens of ‘mental health’ we may see it as if it is.

Due to the fact that ‘mental health’ is still conceptualised as the mirror image of ‘mental illness’ these broad concepts of mental health run the risk of broadening what we think of as mental health problems.
If we see mental health as a state in which people can successfully cope with stress, work effectively, and realise their potential, then it’s hard to avoid seeing ordinary experiences of stress and anxiety, Zoom fatigue and unattained goals through the lens of mental ill-health.

Arts & Culture
The microbiota and our mental health
Pathologising everyday experiences of sadness, dread, loss of motivation, and self-doubt as problems of ‘mental health’ may be counterproductive. By placing a psychiatric frame around their experiences, it may lead some people to catastrophise those problems, over-estimating their vulnerability and under-estimating their capacity to cope.
Some research is beginning to suggest that broad concepts of harm may have negative implications of this kind.
A recent study found that people who held broader concepts of trauma responded with more intense and lasting negative emotions to a disturbing video clip, and that seeing more things as traumas contributed to their vulnerability.
Holding broad concepts of mental health (and illness) may have similar implications.

Nothing here minimises the importance of being alert and responsive to mental health problems or trivialises the experiences of people who are experiencing distress through the pandemic.
Many people are suffering and often that suffering crosses the threshold of mental disorder.
But we are suggesting that it is not always beneficial to frame that suffering in terms of mental health. Sometimes we may be better off seeing our distress as a normal loss of wellbeing rather than as an abnormal loss of mental health.
Part exhibition, part experiment, MENTAL is a welcoming place to confront societal bias and stereotypes about mental health. It features 21 works from local and international artists and research collaborators that explore different ways of being, surviving and connecting to each other. Opening in July 2021, book your free tickets now.
Banner: ECHO by Georgie Pinn: Installation view, MENTAL: Head Inside, Science Gallery Melbourne/Picture: Alan Weedon