Repairing brain injury by learning from a fish

In the quest to repair brain cells after injury or disease, scientists are learning from the zebrafish, which can heal its own tissue
Published 6 August 2017
Repairing brain injury by learning from a fish
In the waterways around the Himalayas lives a small, stripy fish.
As it goes about its daily life searching for food and avoiding predators, the zebrafish can perform an amazing feat to keep itself alive. If injured, even in the eye or brain, it can repair itself using cells that reside within the injured tissues to fully restore function.
In contrast to humans, zebrafish are masters at regenerating their nerve cells. But scientists at the University of Melbourne are studying how they activate certain cells to heal eye injuries with the aim of replicating the process in humans.

“Unlike damage to our skin, which we can repair well, unfortunately an injury to the human eye, brain or spinal cord results in little nerve cell regeneration and a permanent loss of neural functions,” Dr Patricia Jusuf says.
Dr Jusuf and her team, as well as many others around the world, use the zebrafish as a model animal because they belong to the same vertebrate family as humans, and therefore share the crucial genes that enable nerve cell creation. Also, their entire genome has been sequenced, making the zebrafish an ideal place to find answers to genetic questions about human health.
Her team focuses on understanding how regeneration occurs in the eye’s nerve cells, which are affected in neurodegenerative visual diseases, and are similar to nerve cells in the brain and spinal cord.
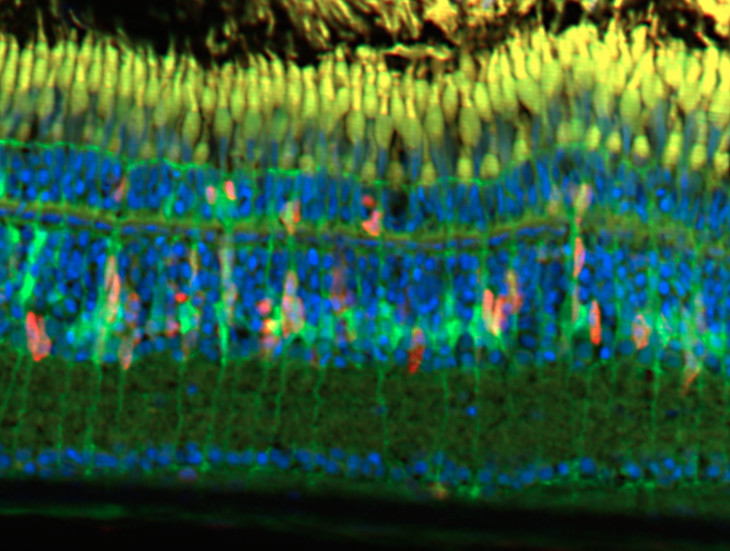
“All vertebrate animal retinas (the sheet of nerve cells in the eye) contain the same cells, including Müller glia cells that are ‘switched on’ or activated after injury,” says Dr Jusuf.
She explains that when these glia cells sense an injury in zebrafish, they activate a whole gene network, including the important master regulator Ascl1, which reprograms them back into stem cell-like precursor cells. These can once again divide to make many new cells that can replace lost nerve cells and so repair the eye tissue and function.
“The eye, brain and spinal cord of zebrafish and humans contain similar glia cells, that have the potential to regenerate nerve cells, ” Dr Jusuf says.
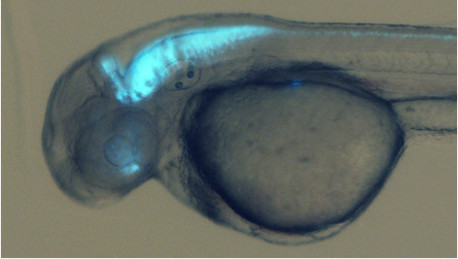
Using a genetically modified strain of zebrafish, in which these glia cells express green fluorescent protein, the cells can be visualised throughout the regenerative response. Using a red stain that shows dividing cells, the green glia cells can be seen to divide to generate new nerve cells following injury.
“Unfortunately when human brain tissue is damaged by injury or disease, we increase the expression of different genes in these glia, resulting in glial scar formation, and permanent loss of neural function.”
It is currently unclear why human glia cells, which have the same genes as zebrafish, so the same ‘ingredients’ for repair, re-express different genes rather than undertaking the regenerative process found in the fish.
A recent study led by the University of Washington has shown that the approach of reactivating regenerative mechanisms identified in zebrafish in a mouse model makes it possible to reactivate glial cells to repair injured nerve cells in the eye.
“This is an amazing result, because it confirms the ability of mice and hopefully humans in using their own glia cells to regenerate their own nerve cells,” Dr Jusuf says.
“By understanding and copying how zebrafish regenerate nerve cells, we hope to benefit patients suffering traumatic spinal cord injury in an accident, or conditions that destroy brain tissue such as Parkinson’s or Alzheimer’s disease,” she adds.
However, once successfully activated, glia still need to regenerate the correct nerve cell to restore appropriate function, as many disorders specifically affect distinct nerve cell types. Each of these may require precise re-expression of different sets of genes, which could complicate this process enormously, given the many different types we possess.
In order to better understand this process of cell specification, Dr Jusuf and her team, including researchers from the Australian Regenerative Medicine Institute at Monash University, removed specific nerve cells in the zebrafish retina, and tracked activated glia throughout the repair process.
Their study revealed that injury repair is actually ‘dynamic’, so the existing glia are able to take cues from their environment, and sense which cell is needed to be produced for efficient repair.

“We found that regenerating glia were incredibly adaptive. When we removed nerve cell types A and B, glia regenerated lots of A and B, until the normal cell type proportions were restored. Glia then switched back to making all five retinal nerve cell types, thus constantly adjusting and fine tuning their regenerative response to ultimately restore appropriate cell type ratios,” says Dr Jusuf.
This incredible dynamic ability of glia means that once activated within the injured tissue, regenerative processes could restore the correct proportion of nerve cell types without further genetic intervention, regardless of the injury or cell type lost.
The next step for Dr Jusuf’s team is to work out ‘cues’ that these glia use to successfully regenerate specific nerve cells, such as those lost in different visual diseases including retinitis pigmentosa and glaucoma.
To do this, and other related projects, Dr Jusuf has set up the University’s first zebrafish focussed laboratory. She aims to expand work on the zebrafish as a model system with new collaborative projects in the University and the Parkville research precinct, including drug screening approaches for human health.
The little zebrafish has certainly come a long way from the waterways of Asia, and still has a lot to teach us about our own biology.
Banner image: Getty Images
