
Health & Medicine
Switching to a plant-based diet? Keep an eye on your micronutrients

Computer modelling shows that swapping meat and milk for plant-based alternatives isn’t a simple switch when it comes to our health
Published 20 April 2023
Mitigating climate change is a key challenge of our time. One way many people try to reduce their greenhouse gas emissions is to eat less animal-source food – like meat and dairy – and instead eat more plant-based food.
But rather than transitioning to diets high in coarse grains, pulses, fruit, vegetables, nuts and seeds as recommended – people are more commonly simply swapping dairy milk for plant-based ‘milk’ and animal meat for plant-based ‘meat’.

Over the past decade or so, there has been phenomenal growth in the range and sales of plant-based ‘milk’ and ‘meat’ in Australia and internationally, and this trend is predicted to continue.
Plant-based ‘meat’ and ‘milk’ are similar in appearance and function to the animal-source originals, so it’s an easy and convenient swap to make. Most consumers perceive plant-based ‘milk’ and ‘meat’ as healthy.
So, what happens to our nutrient intake when these simple swaps are made?

Health & Medicine
Switching to a plant-based diet? Keep an eye on your micronutrients
Unfortunately, it’s complicated.
For one, plant-based ‘milk’ and ‘meat’ are not nutritionally equivalent to the animal-source versions. Additionally, plant-based foods that appear similar to each often vary widely when it comes to nutritional composition.
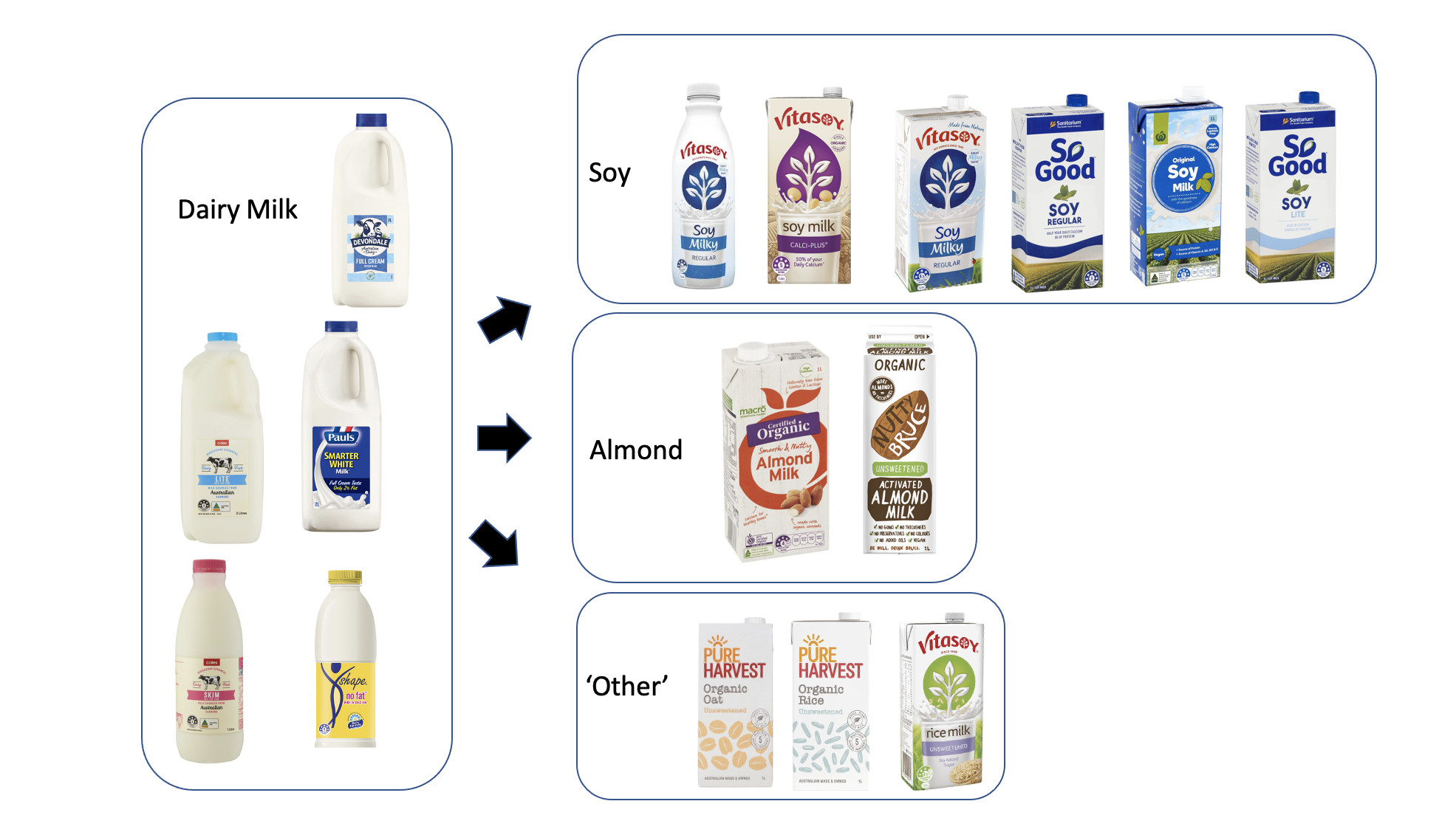
For example, the nutritional makeup of plant-based ‘milks’ varies according to the base ingredient (like almonds, oats, rice or soy), as well as by the type and level of fortification (added nutrients like calcium) and sweetening.
On top of this, most foods contain many more nutrients than are listed on their label, so assessing the full implications of our choices can be difficult.

To get a fuller picture, we looked at the food composition database published by Food Standards Australia New Zealand, covering 53 nutrients across 5,740 foods and beverages.
Our recent study, published in the journal Nutrients, used a computer simulation called dietary modelling to assess the likely nutritional implications of Australians swapping animal products for plant-based copies.
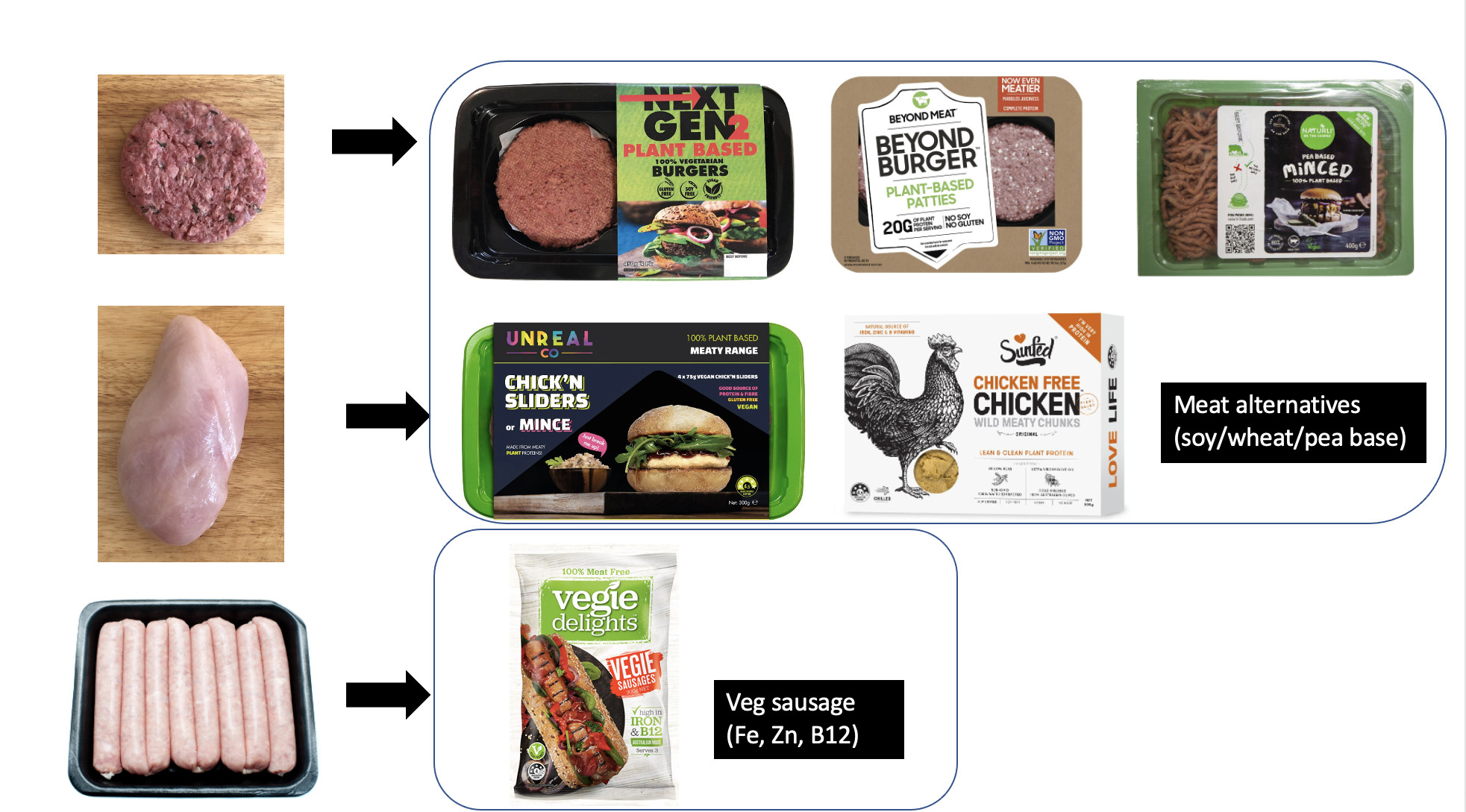
We modelled a scenario where the Australian population, on average, swapped approximately 2.5 meals per week of animal-source meat (beef, chicken and sausages) for plant-based ‘meat’ and approximately one litre of dairy milk for plant-based ‘milk’s (soy, almond, oat and rice).
Health & Medicine
Eating supplements cannot beat the real thing
We focused on the main nutrients that these ‘easily swappable’ animal-source products contribute to our overall diet, using the full range of nutrients from our national food composition database rather than just those listed on the food labels.
Our modelling shows that the likely impact of switching varies from nutrient to nutrient – iron intake increases by 15 per cent and unfortunately sodium intake increases by seven per cent, but most other nutrients decline.
Most concerning were the predicted declines in intake of vitamin B12 (19 per cent), iodine (14 per cent), long-chain omega-3 fatty acid (eight per cent) and zinc (seven per cent).
These nutrients are important.
Iodine is an essential component of thyroid hormones and is critical for brain development; Vitamin B12 is important for neurological pathways and normal blood functioning; Zinc is an important component of many enzymes needed to keep us healthy; and Omega-3 has health benefits throughout life, from foetal development through to keeping our hearts and brains healthy as we age.
Already, quite a lot of us don’t get enough of these nutrients, and the declines we modelled with a simple, like-for-like move from animal-sourced to plant-sourced foods would likely make these dietary inadequacies worse.

Health & Medicine
Why COVID-19 should make us rethink our relationship with meat
For example, the World Health Organization has classified the Australian population as mildly iodine deficient and women are at continued risk of iodine deficiency during pregnancy.
Milk is an important source of iodine in Australia, but without fortification, plant-based milk is very low in iodine. As a result, in the UK around 20 per cent of plant milks are iodine fortified but, here in Australia, just one per cent of plant-based ‘milks’ sold in supermarkets contain iodine.
Vitamin B12 is present in both meat and dairy, and between five and eight per cent of females aged 14 years and over don’t get enough. Switching to plant-based versions is likely to exacerbate this dietary inadequacy.
Approximately one in three young men and two in three older men don’t have enough zinc in their diets. And there’s a double whammy with switching to plant-based versions. Meat contains chemicals that enhance zinc absorption while plants often contain factors that reduce zinc absorption.
So, making the switch not only leads to a fall in zinc intake, but the zinc provided by plant-based ‘meat’ and ‘milk’ is likely to be less available to the body.
Approximately 80 per cent of Australian adults consume less than the recommended intake of long-chain omega-3 fatty acids. Australian meat, especially if grass-fed, is a useful source of long-chain omega-3 fatty acids, particularly for people who consume little or no fish.
Plant-based ‘meat’ tends to contain little or no long-chain omega-3 fatty acids.

Health & Medicine
Food Health Star labels are driving healthier products
While dietary recommendations encourage us to eat less meat and dairy, and eat more coarse grains, pulses, fruit, vegetables, nuts and seeds, clever marketing and the comfort of familiarity mean that meat and milk are often replaced by plant-based copies.
It’s time to re-consider regulations for fortifying plant-based ‘meat’ and ‘milk’ with nutrients that might otherwise be missing from our diets. This may help those transitioning to plant-based diets to maintain an adequate nutrient intake.
We also need to consider how plant-based ‘meat’ and plant-based ‘milk’ best fit into Australia’s national food selection guide, the Australian Guide to Healthy Eating.
At present, calcium content is the main determinant for the inclusion of plant-based ‘milks’ in the same food group as dairy milk – should we also look at nutrients like vitamin B12 and iodine?
‘Green nudges’, policy actions and public health messages to encourage the transition to a more environmentally sustainable diet are vital. But we also need to consider nutrient intake when developing them, particularly for the young, the elderly and women of childbearing age.
Banner: Getty Images