
Politics & Society
Disability-based disadvantage – a life sentence?

Better regulation of the use of coercion in healthcare settings is needed to protect human rights
Published 21 November 2016
Coronial inquiries provide a harrowing reminder of how the use of physical, chemical or mechanical restraint to control behaviour in Australian healthcare settings can go terribly wrong.
They certainly shocked Professor Bernadette McSherry, Foundation Director of the Melbourne Social Equity Institute at the University of Melbourne. It also inspired her to investigate how these practices could be curbed, if not eliminated. Given the complexity of the issue, it’s a formidable challenge.
“If a person is flailing out, and we know that those in healthcare settings do get assaulted, restraint is seen as a necessary evil,” Professor McSherry explains. “But the danger is that it becomes the norm. If someone is beginning to show signs of distress or acting up, the response is often, quickly, let’s restrain them or give them an injection to sedate them.
“It’s a fine line between restraining someone to prevent injury and using it as a control mechanism as part of a coercive culture.”

Incidents of restraint can be confronting. In South Australia, a 20-year-old man was shackled to a hospital bed, denied showering and toilet facilities and forced to wear an adult nappy for five days.
In another incident, a woman had both arms and a leg cuffed and chained while giving birth. Two men with mental health issues died in Victorian hospitals from ‘positional asphyxia’ while being restrained in a prone position on the ground.
“This could be the tip of the iceberg,” says Professor McSherry. “It could be worse. We just don’t know because there’s no national mandatory requirement for reporting.”
Regulations to control the use of restraint is patchy across Australia, a situation that she believes is failing to protect the basic human rights of those being restrained. She is leading a four-year investigation, funded by the Australian Research Council, that will produce a set of recommendations to regulate how and when restraint is used in mental health, aged care and disability care settings.

Politics & Society
Disability-based disadvantage – a life sentence?
Professionally, she is the perfect woman for the job.
Professor McSherry is an internationally recognised legal academic in the fields of criminal law and mental health law and for the past 15 years has served as a legal member of the Mental Health Tribunal of Victoria.
“I have always been concerned about the use of coercion,” she explains. “I have worked with a number of people who have experienced being restrained or secluded, and through hearing their stories, it has opened my eyes to what can happen in some settings.
“I would certainly like much more regulation and reduction of these types of practices.”
Professor McSherry readily accepts that on occasion the behaviour of some people may need to be controlled because they pose a risk to themselves or to someone else. For example, if someone high on drugs is admitted to an emergency department and is flailing about, physical restraint or sedation may be the only course open to staff. However, she believes that in an aged-care setting, other options may be considered ahead of restraint.
A number of options are open to healthcare professionals to calm patients without resorting to restraint. A trial of the ‘Safewards’ model is now underway in Victoria. It deploys a number of strategies, including the provision of a calm environment and the training of staff to recognise the signs of patients moving into stressful states, to reduce the rates of restraint.
Its effectiveness has not yet been established, but similar trials in England have shown promise.
The use of restraint may be tied to a lack of resources. “In pressured environments, it’s easy to control behaviour if you over-medicate people rather than spend time with the person, calming them down in order to avoid restraint.”
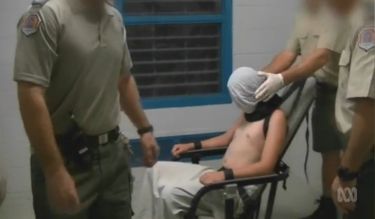
Politics & Society
Four Corners: Using restraints can be called torture
Professor McSherry believes Australia still lags behind Europe in its approach. In the Netherlands, for example, facilities can lose their accreditation if restraint rates go up. They also have in place more requirements for monitoring and reporting.
Given the demands on the Australian health dollar, resources tend to go to those groups who lobby hard. Many of those with mental health issues, with disabilities, or those who are in aged-care facilities are voiceless.
“This is about respecting the dignity of every human being,” she says.
“I was always taught in my law degree not to worry so much about what the law is, but what the law should be. I’ve always had that perspective of law reform – what can we do to make a change for the better rather than just accept the status quo.”
Professor McSherry is most interested in discovering how to provide good quality care that goes beyond coercion.
“At the moment we have an emergency driven system where you wait until a person is in distress before there is an intervention. I would much rather that the emphasis be placed on how we go about constructing a system where people get the treatment they need, they want, and that they have a say in. It’s about providing support before people reach the crisis point in their lives.”
Banner Image: Shutterstock