
Politics & Society
Chemical restraint: Behind locked doors

Victoria has some of the highest reported rates of restrictive practices in mental health in Australia, but the upcoming Victorian Royal Commission may not investigate them
Published 19 January 2019
Twenty years ago, it was generally agreed Victoria had the best mental health services in Australia. But today, there are signs it’s faring the worst.
Where once Victoria had the highest per capita spending on mental health care, it now has the lowest. Funding to community-based support and inpatient beds has failed to match significant population growth, leaving the state with the lowest number of full-time equivalent staff per capita in the country.
In response, the Andrews Government has taken the rare step of initiating a Royal Commission into Mental Health in Victoria. Public consultation to determine the Commission’s terms of reference is now underway and responses have already been strong.
One thing the proposed terms of reference doesn’t include is a consideration of the use of restrictive practices in services, and yet the issue requires urgent attention.
Restrictive practices are used in psychiatric wards, emergency departments and other mental health settings.

Politics & Society
Chemical restraint: Behind locked doors
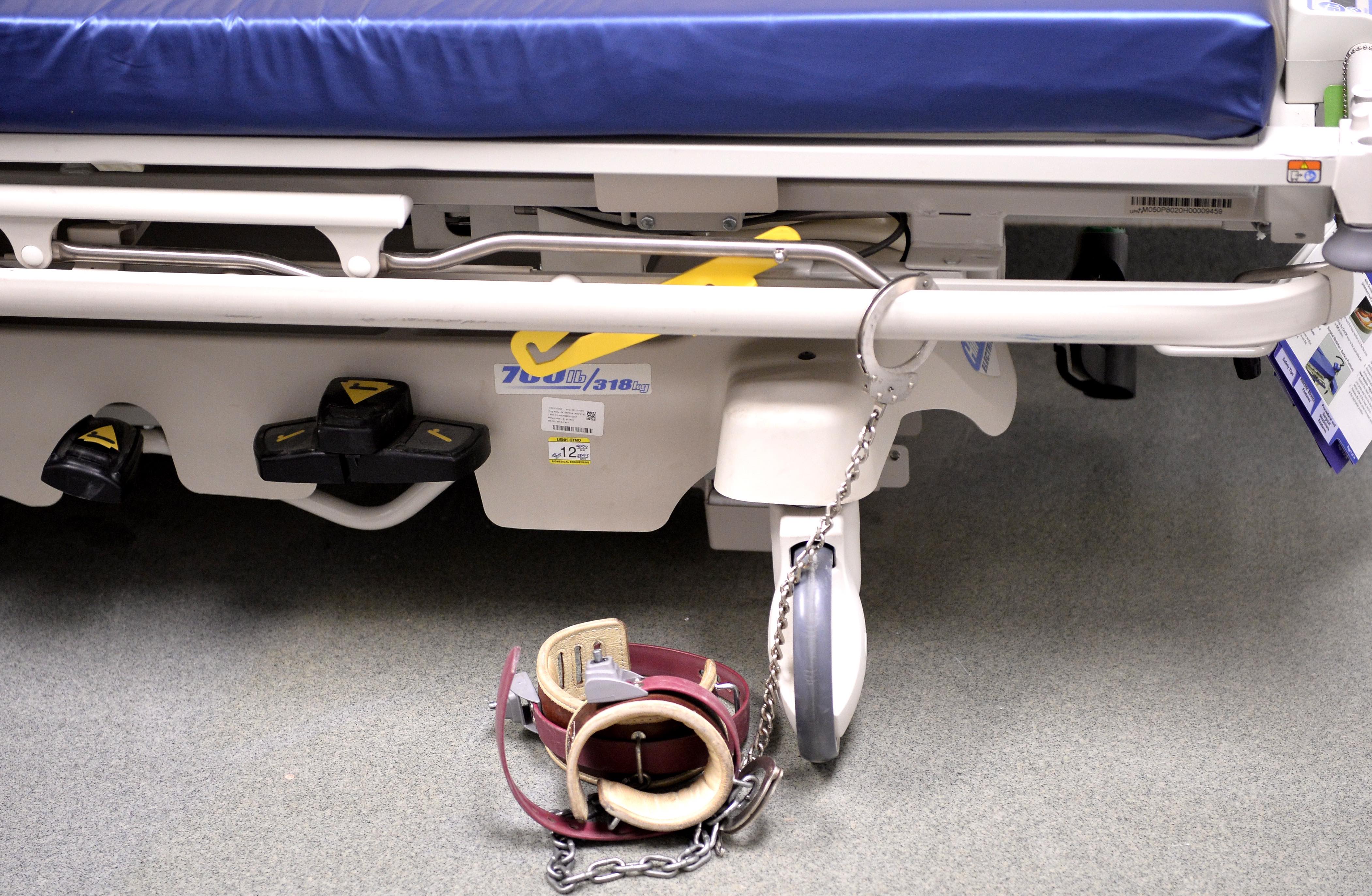
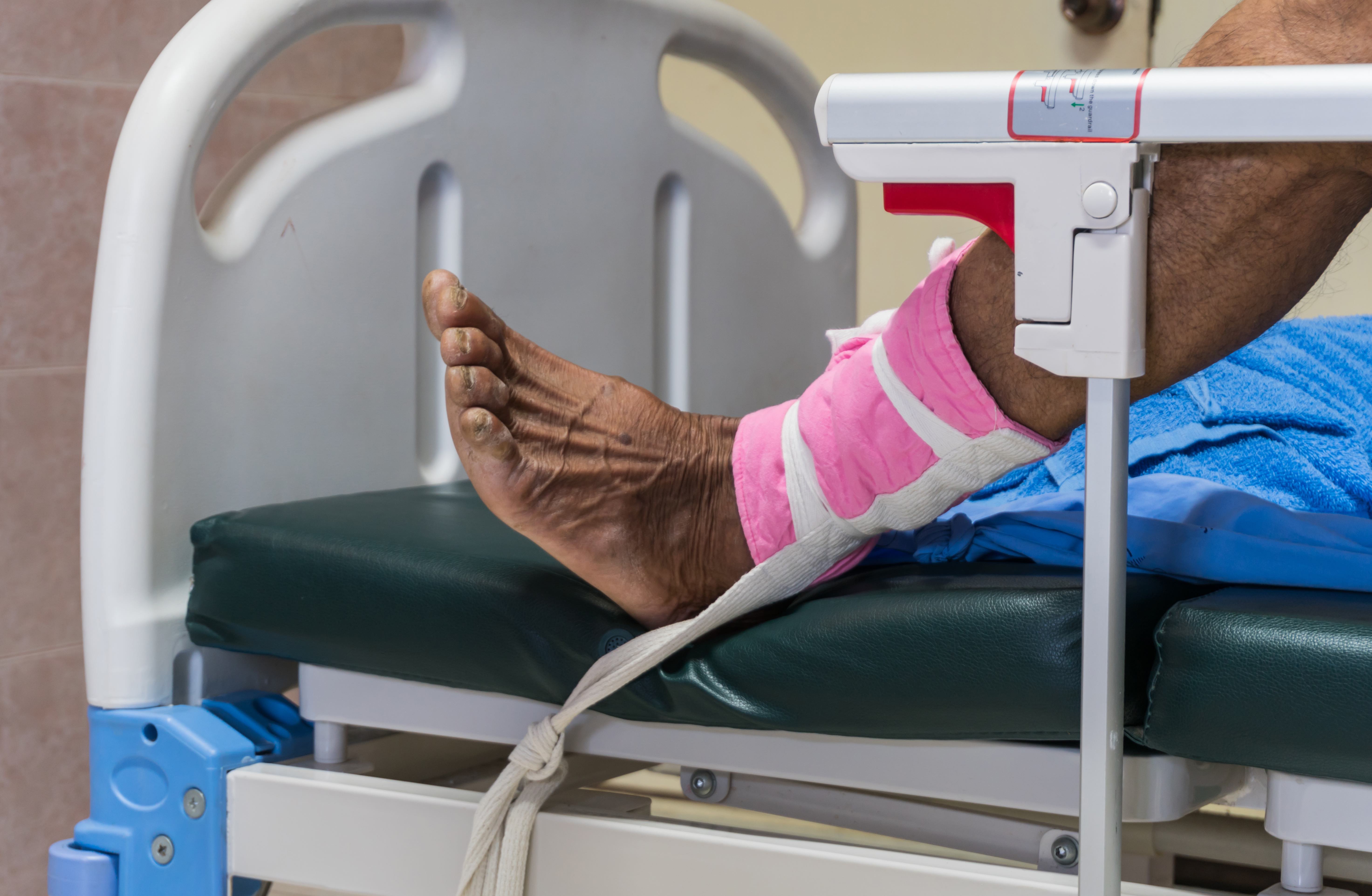
They include a range of practices used to control behaviour, including confining a person to a room or area that they cannot leave (known as seclusion), using physical restraint (like holding someone down), or mechanical restraint (the use of belts, straps and jackets).
It’s an issue that’s already been raised in aged care. Most recently the ABC’s 7.30 Report covered the practice used on dementia patients. Now, Aged Care Minister Ken Wyatt has announced new regulations to regulate physical and chemical restraints in aged care homes. Sadly, with the Royal Commission into Aged Care Quality and Safety now underway, many similar stories will undoubtedly emerge.
The use of restrictive practices in Victorian mental health services is currently regulated by legislation and guidelines, and is generally permitted where necessary to prevent harm to an individual or others, and where no less restrictive intervention seems possible.
Chemical restraint is not permitted in Victoria, although advocates and researchers have expressed serious concern about the sedating use of commonly administered medications.

Some commentators and advocates have called for the elimination of all restrictive practices on the basis they cause harm and are counter-therapeutic, but there continues to be a widespread view that some restrictive intervention is needed in certain emergency situations.
However, it’s also generally agreed that high rates of restraint and seclusion in mental health services in Australia and elsewhere are a sign that mental health systems are in crisis.
In a recent report commissioned by the World Psychiatric Association, the 40 authors commented that the ‘[u]se of compulsion needs to be seen as a system failure’.

Health & Medicine
Time to hold back on the use of restraints
Statistics comparing Victoria to other states and territories are compiled by the Australian Institute of Health and Welfare (AIHW). The AIHW offer the caveat that Victoria’s seclusion and restraint figures may be inflated by its service delivery model, which produces a higher threshold for acute admission.
Differences in service models and definitions of restrictive practices between jurisdictions also make it difficult to get definitive data. But while some caution should be used to interpret the data, Victoria’s rates of seclusion and restraint paint a troubling picture.
In 2015-17, the AIHW reported that Victoria had the highest national rates of physical restraint (although data was not publicly available for Queensland). Under prevailing definitions used by the AIHW, Victoria’s rate was more than double the national average.
Victorian public sector acute hospitals also reported the highest average duration that a person was secluded. The average time a person in Victoria spent in seclusion in these settings in 2016-17 was reportedly 10 hours — again, more than double the national average reported by the AIHW.
Victorian hospitals have the second highest proportion of mental health-related admissions that resulted in seclusion, and the third highest rates of seclusion per capita.
While the AIHW did report a 50 per cent reduction in seclusion rates in Victoria since 2008, more recent statistics suggested that rates are again increasing.
Other forms of coercion, such as involuntary treatment and detention in hospital, also raise concerns in Victoria.
Politics & Society
Four Corners: Using restraints can be called torture
Most people who experience mental health conditions seek help on a voluntary basis but in certain circumstances, mental health legislation authorises detention in mental health facilities and compulsory treatment regardless of a person’s wishes and preferences.
Nationwide, people who were admitted to specialised psychiatric care for a mental health crisis were given an involuntary status under law in 2016-17 at an average rate of 45.4 per cent, according to the AIHW. In Victoria the rate of compulsion in 2015-16 was reported to be 52 per cent of hospitalisations overall.
Involuntary treatment outside hospital, in people’s homes – referred to as ‘community treatment orders’ (or CTOs) – is also unusually high in Victoria. According to one study, Victoria has the highest rate of CTO-use recorded nationally, and possibly even one of the highest rates in the world.
The Royal Commission into Mental Health presents an opportunity to listen to the voices of mental health service users who have been subject to restrictive practices, involuntary detention and treatment or CTOs, and to identify opportunities to address the high rates of their use in this state including clarifying data issues.

There is a growing body of evidence for ways to reduce and even eliminate coercive responses to mental distress, and the Royal Commission could draw attention to such practices.
This includes existing Victorian Government initiatives like Safewards, a program currently being rolled-out to reduce seclusion and restraint measures in inpatient mental health units across the state including adult, adolescent, aged and secure units.
But if the Victorian Royal Commission overlooks the use of restrictive practices in mental health services, the opportunity to shine a light on this important issue may pass.
The Victorian Government is seeking public feedback on the proposed Terms of Reference for the Royal Commission into Mental Health. Submissions are due by the 27th of January. For more information on restrictive practices in mental health services, find University of Melbourne research here and here.
Banner: Getty Images