Health & Medicine
The right antibiotic at the right time

New research finds antibiotics are often prescribed inappropriately before, during and after surgery, and more needs to be done to change the culture of prescription
Published 4 December 2019
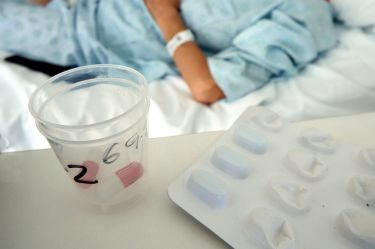
More than half of the antibiotics used to prevent infection before, during and after surgery may not be appropriately prescribed.
Antibiotics are commonly used to prevent infections before, during and after surgery (known as surgical antibiotic prophylaxis). In fact, surgical antibiotic prophylaxis has been identified as the most common reason for antibiotic use in Australian hospitals since 2013.

Our new study, a collaboration between the University of Melbourne and Monash University, has found that antibiotics are often prescribed at the incorrect time and for unnecessarily long durations after surgery.
Not all surgical procedures require antibiotics, and when they are needed, only a single dose is usually recommended beforehand.
For many procedures, the guidelines do not recommend additional doses after surgery.

Health & Medicine
The right antibiotic at the right time
The Hospital National Antimicrobial Prescribing Survey (Hospital NAPS) program at the University of Melbourne and Melbourne Health has consistently highlighted that surgical antibiotic prophylaxis is often prescribed inappropriately.
The program has expanded to include a new module, the Surgical NAPS, that specifically evaluates prescribing practices in surgical settings, with the aim of helping health services to monitor and improve prescribing.
Our research has found that less than half – 48.7 per cent – of 15,395 prescriptions for 9,351 surgeries (from 2016 to 2018) were assessed as appropriate.
Procedural antibiotic prescribing (antibiotics given before or during surgery) was assessed as inappropriate in 40.5 per cent of doses, while post-procedural prescribing was found to be inappropriate in more than 60 per cent of doses.

We also compared prescribing appropriateness across different types of surgeries (adjusting for hospital, patient and other surgical factors).
Our research has found that appropriateness of procedural prescribing ranged from 33.7 per cent to 68.9 per cent, while the appropriateness of post-procedural prescribing ranged from 21.5 per cent to 58.7 per cent.
When antibiotics were prescribed as required before surgery but were assessed as inappropriate, the most common reason for inappropriateness was timing (49.5 per cent) – that is, the antibiotics were administered too early or too late.

Health & Medicine
How do we close the gaps in appropriate antibiotic use?
However, the exact time that the surgery started (the time the first incision was made) was documented in only 65.6 per cent of cases, which makes it difficult to comprehensively assess appropriateness for the timing of antibiotic administration.
When antibiotics were prescribed as required after surgery but were assessed as inappropriate, the most common reason for inappropriateness was prolonged duration, at 54.3 per cent.
Our research highlights some key issues around the duration of post-procedural antimicrobial use, timing of antibiotic use and documentation of the time of surgical incision.
It’s also important to consider that decision makingabout antibiotic prescribing is complex and involves multiple healthcare professionals who work across pre-, intra- and post-operative surgical settings.

We conducted a second study to better understand what drives the prescribing of antibiotics in surgical settings, and what other factors may help facilitate quality improvement.
We found that improving antibiotic prescribing before and after surgery was considered a low priority, and guidelines were not regularly consulted.
The culture of prescribing (described elsewhere as ‘prescribing etiquette’) appears to reinforce established practices.
Health & Medicine
The rise of the latest drug resistant superbug
For example, some junior surgeons say that they feel uncomfortable challenging the practices of their seniors, for fear of professional repercussions.
“As a resident. . . it’s not within my power to say, ‘Just stop it [the antibiotics].’ I have to ask someone else.” (Public orthopaedic surgeon.)
The senior consultant has primary responsibility over the patient, and they will invariably determine how that patient is looked after.
“It’s (up to) the consultants. You can’t (change practice to single dose surgical antibiotic prophylaxis). . . They’ve got to be on board with it. Because, at the end of the day, you stop the antibiotics based on evidence, and something goes wrong – it will be your fault. Often, I’ll just go with what my seniors have told me because, you know, that’s what we do.” (Public surgical resident/registrar.)
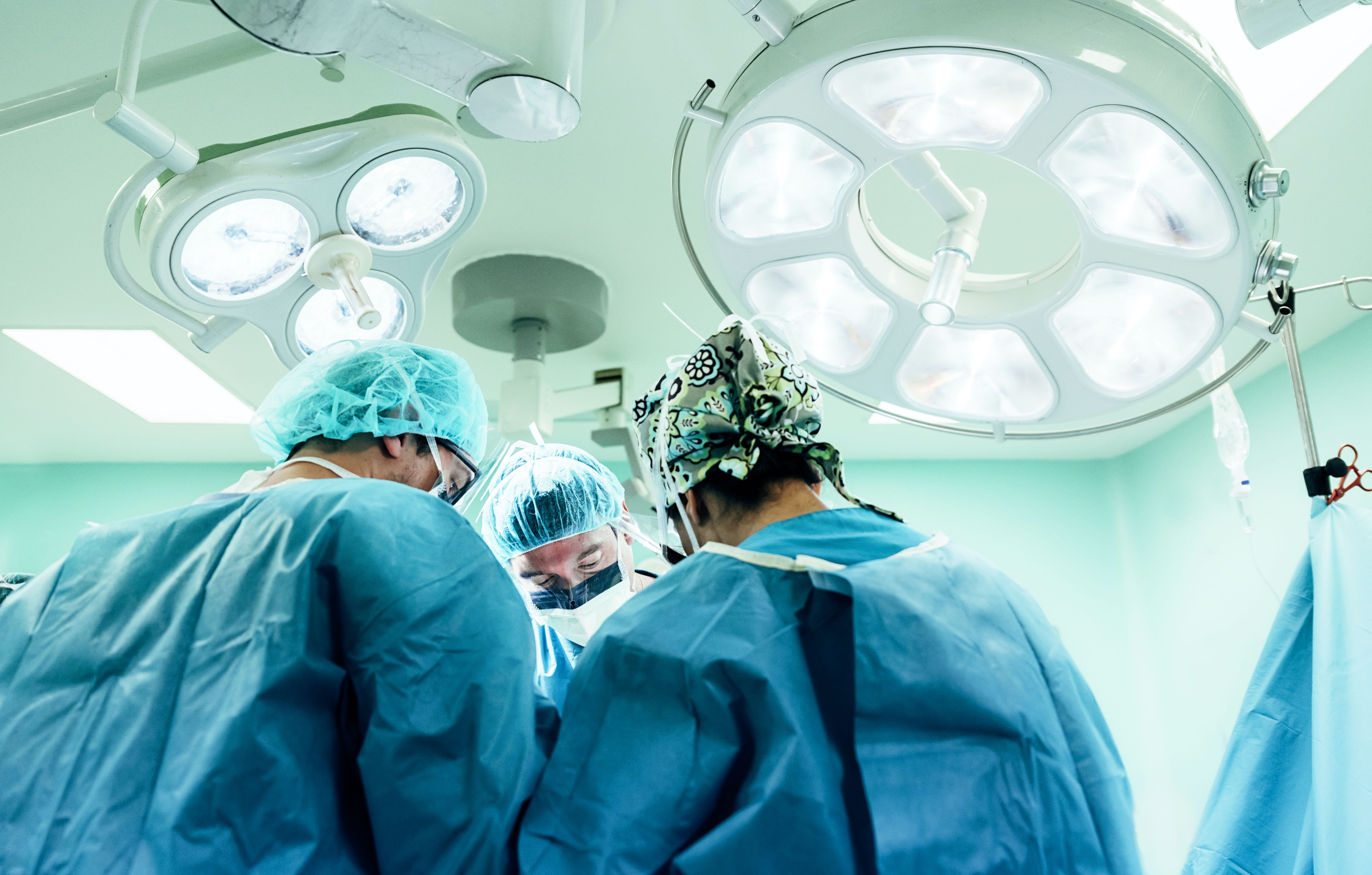
Many senior surgeons and anaesthetists describe their fears about missing infections. It’s apparent that their perceptions about the risk of infection, and justified fears about the consequences of missing infection, can hinder appropriate prescribing.
Clinicians also identified a need for improved communication, documentation and collection of local data for action.
The Surgical NAPS helps to facilitate this. But we need more resources to collect data on surgical outcomes that might support prescriber behaviour change.

Health & Medicine
Is this the end for alcohol handwash in hospitals?
However, clinicians have provided some positive feedback about current practices that could be used to improve antibiotic use.
Clinicians commonly use a time-out to plan a procedure and check that all the requirements have been met.
“They (surgeons, anaesthetists and scrub nurses) definitely use the time-out. Everyone uses the time-out.” (Private theatre nurse.)
In the future, factoring in a discussion about the prescribing of appropriate surgical prophylaxis before and after surgery within the time-out could be a practical way forward.
Our study follows on from qualitative research on surgical antibiotic prescribing culture conducted in both Australia and the UK. It also highlights factors that influence decision-making, and multiple barriers to, and enablers of, appropriate surgical prophylaxis prescribing.

Potential solutions could include targeting antimicrobial stewardship at senior surgical consultants, rather than junior surgeons. Surgeons should (and want to) be actively involved in addressing national and global concerns about the overuse of antibiotics.
Healthcare in Australia is multi-disciplinary and collaborative, so improving surgical antibiotic use is not solely a surgeon’s problem.
It requires extensive collaboration from everyone – from surgeons, anaesthetists and infectious diseases physicians, to pharmacists and nurses.
But it must be done with the backing of professional bodies such as the Royal Australasian College of Surgeons and the Australian and New Zealand College of Anaesthetists, as well as hospital executives and government.
Banner: Shutterstock