
Health & Medicine
Reinfection in COVID-19
What are the implications of reinfection for vaccines, antibody passports and herd immunity?
Published 23 September 2020
Over the past two weeks we’ve discussed two well-documented instances of reinfection in people who had symptomatic COVID-19 infection and apparently recovered, but became infected again with a distinct ‘bar-coded’ (by mutation) virus variant.
There are also a couple of fragmentary media mentions of individual cases in Belgium and the Netherlands.
So far, only one person (Nevada) has been reported with substantial clinical symptoms the second time round though, as the interval between the two infections was relatively short, at least some of this could have been a carryover from the first exposure.
And, in none of the instances so far, was it established that the second infection led to the production of infectious virus.
The perception at this stage is thus: that reinfection with SARS-CoV-2 can occur in the absence of any significant antigenic change in the spike protein receptor binding domain (RBD for ACE2), though perhaps uncommonly, during (at least) the first six months.

Health & Medicine
Reinfection in COVID-19
And, even when that does happen, this may have the desirable effect of boosting the individual’s immune response. Such reinfection is common for many respiratory viruses.
Children, for instance, can be reinfected with the same parainfluenza virus variant in successive cold and flu seasons, with the first instance causing a disease that ranges in severity from a common cold, to croup, to something like influenza.
The symptoms becoming progressively less severe in the following two to three years, when the individual seems to become fully immune. The young can, though, reinfect their grandparents, who likely went through the same sequence of annual challenge many decades earlier.
That can have severe clinical consequences in the elderly, and in children who are immunosuppressed by, for example, cancer chemotherapy or bone marrow transplantation.

Even so, the fact that we’ve never bothered to try to make vaccines against these viruses is a measure of the overall level of unconcern.
In this capacity to reinfect, the parainfluenza viruses seem to be different from the not too distantly related influenza viruses, where there is evidence of much more enduring immunity to the exact same sub-strain.
Unlike the coronaviruses and the parainfluenza viruses, influenza A and B viruses constantly throw-off enormous numbers of antibody-selected mutants with, each year or so, one of those antigenic variants emerging to cause a new ‘seasonal’ epidemic.

Health & Medicine
Reinfection in COVID-19- Part two
For some reason, when those viruses inevitably ‘go global’, we still identify these events as an epidemic rather than a pandemic. When a new ‘seasonal flu’ emerges, the strain that was circulating the year before disappears, often very fast.
So what does this tell us about COVID-19 and the prospects for achieving herd immunity?
Looking at the numbers of reported infections, I’m not convinced that we’ve actually achieved herd immunity in all but the most severely affected locations.
Some serological surveys looking for antibody as a measure of past exposure have suggested that I may be very wrong in this, but there have been real concerns about the sensitivity and specificity of, particularly, some early Ig assays.

Where possible, they need to be validated by checking panels of ‘historical’ reference sera collected back before November 2019.
My conviction at this stage is, though, that we will only achieve widespread herd immunity with vaccines. And, given that reinfection can occur, that would include boosting those who have already had clinical disease and/or been positive by the PCR test.
It may also be the case that we will need to give an annual vaccine booster shot, perhaps with (as in influenza) a vaccine that has been ‘tweaked’ (using a slightly different spike protein RBD) to cover for antigenic changes in the virus.
Health & Medicine
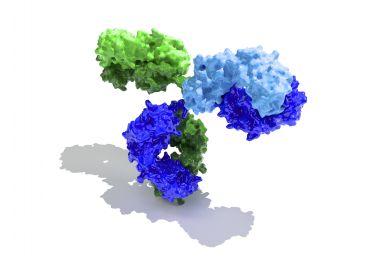
Your protective Igs: The major focus of COVID-19 vaccines
Licensing such a variant COVID-19 vaccine should, following the influenza model, be a straightforward and rapid process.
Will we see antibody passports? I think their time is past.
A more likely scenario is that all of us will have an official vaccination certificate showing that the holder has received the one or two (or more) required ‘shots’ as the necessary documentation for travel, access to restricted locations and employment and so forth.
And what about vaccines?
I’ll be writing a lot more about vaccines when we see data on how well any of the current products are working in people.
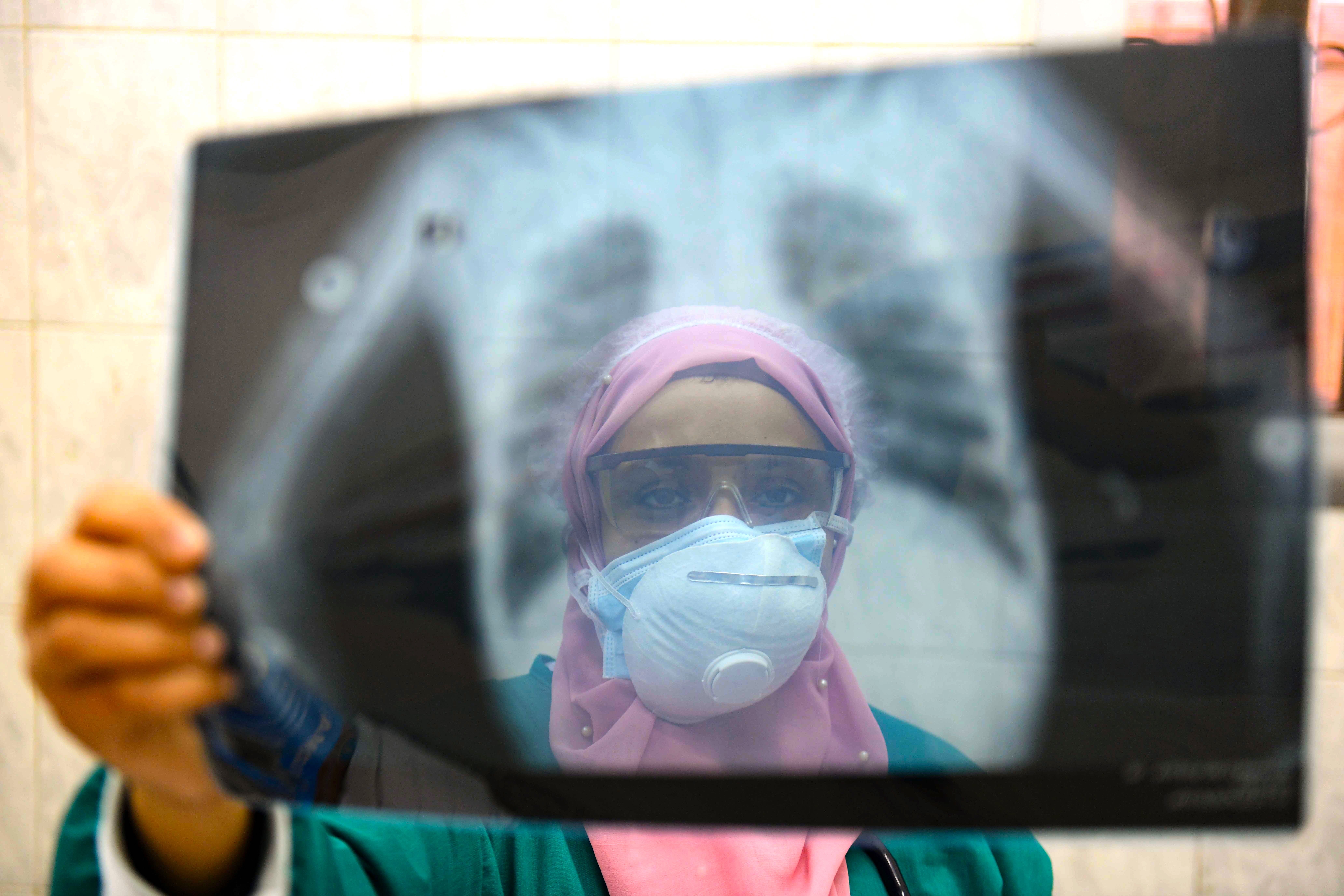
At best, given the influenza experience, my guess is that SARS-CVoV-2 vaccines will be 60 to 70 per cent effective in preventing people developing at least some symptoms, and hopefully better than that when it comes to lowering the instance of hospitalisation and severe disease.
I would be delighted to be wrong on the low side of expectations, but we shall see.
The other big question re vaccines is: how effective will they be in stopping transmission?
Maybe they won’t prevent all infection in the nose, but might they greatly decrease total virus production in the lung and the dangers associated with coughing and aerosol production?
Hopefully antibodies in the blood will prevent the heart, kidney, brain and vascular damage that likely result from viremia.
Right now, we just have to wait until we hear some results from the current Phase 3 trials for those candidate vaccines that are furthest forward.
Banner: Getty Images