As a health worker, what’s my risk from COVID-19?
Health workers are doing it tough on the front line of the pandemic and some have died, but for most the risk of fatal infection is very low, and the risk to older health workers can be mitigated
Last Friday, I finished home quarantine after returning from the USA. The next day, I was working in the COVID-19 isolation unit at an Emergency Department in Melbourne.
Around the world, healthcare workers on the frontline of the COVID-19 crisis are being hailed as heroes, as they work to save lives despite the risk of infection and death.
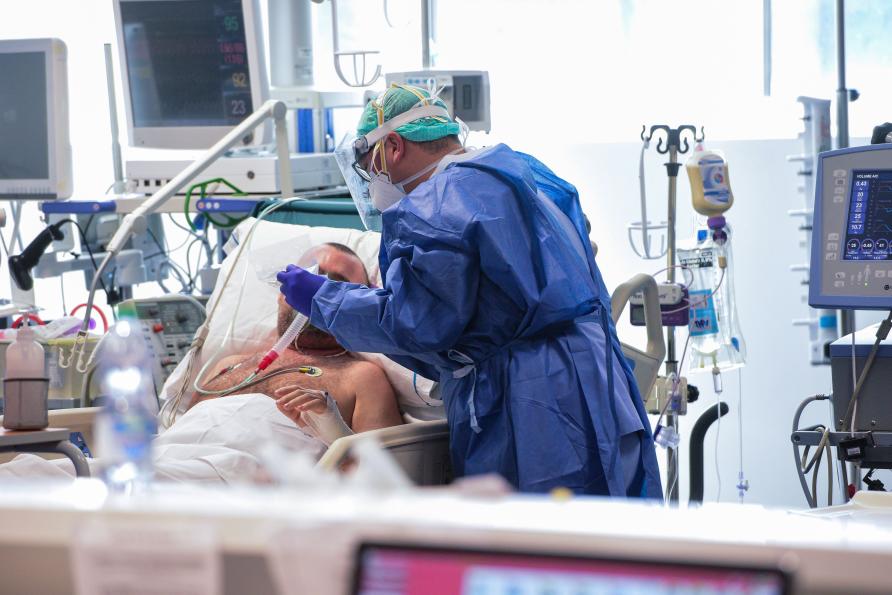
On top of this, many are also working long hours, suffering distress and fatigue, stigma, and even physical and psychological violence.
Health workers are being infected. And some are dying.
So, it was important to me, as a husband and father to three young children, to really understand my risk of death, and the risk that any of my clinical work might pose to my family.

Protecting people with disability during the pandemic
While there is a very real toll on clinicians who are managing and supporting large numbers of people including families and exhausted staff, I think the government and health institutions could more clearly communicate the actual risk of death.
To do this, we need to separate the idea of individual risk from population risk. One person can have an exceedingly small personal risk but still represent a significant population risk.
For example, young health workers need to be protected from infection because of their possible transmission to others within the health system – that is, a population-level threat – but the actual risk of death to the young health worker at an individual level is low.
I am 43.4 years old, which is exactly the same age as the average Australian healthcare worker. But if we’re focusing on the clinical setting of an Emergency Department (ED), I think the average worker would be at least five years younger.

So, what is the risk of death to a 43.4-year-old going to an ED COVID-19 treatment room?
Firstly, I work part-time in a hospital that has an excellent isolation unit and does everything possible to protect the staff from infection – the amount of disposable plastic Personal Protective Equipment (PPE) equipment we go through is astonishing.
Despite these excellent precautions, let’s assume a worst-case scenario that over the next six months 40 to 50 per cent of my colleagues were to become infected. It may sound alarming but how scared should younger health workers like me be?

At-risk Aboriginal women and children forgotten in crisis
The Lancet, a leading medical journal, recently detailed China’s Infection fatality rate (IFR) for 40 to 49-year-olds at 0.161 and it was lower again in Italy.
The accuracy of China’s reporting has recently been called into question by some US economists and politicians. However, the World Health Organisation (WHO) has responded that China has updated their figures as more information becomes available. What this means, is that I am working off the original figures, which may need to be adjusted as more global data becomes available.
China’s health system was ill-prepared, overloaded and caught by surprise by COVID-19. Furthermore, of those who died in China and Italy, many had co-morbidities, and many of their death certificates and cause of death should have been assigned to heart disease or end-stage lung disease, not COVID-19.
It may be then that in Australia, the IFR may actually be around 25 per cent of the rates seen in Wuhan, and more like those in South Korea or Germany, considering our better-prepared system and the greater time we’ve had to plan a response with increased capacity.

The estimated IFR for the average health worker in Australia would be equal to 0.040 per cent (that is, 0.161 per cent x 0.25).
Interestingly, analysis of Italy’s first 73,534 cases revealed 6334 health workers were infected; 11 died and none of them were under the age of 50.
If 50 per cent of 43-year-olds working in ED were to contract COVID-19 then my chance of dying at work becomes 0.02 per cent – or a one in 5,000 chance.

COVID-19 and containment: A dual burden for India
To put that in perspective, I have a similar risk of dying while riding my bike to work over a six-year period.
Importantly, it appears there is virtually no risk of my children (aged two, seven and nine) dying as a result of me bringing the virus home, given the data from 72,314 cases in China where no child under nine died.
On the other hand, if an ED worker is aged 65 years or more, their risk of death from going to work is about 0.2 per cent – or one in 500.
And this is where I do think the word heroic is apt – I know of many older GPs who are coming out of retirement to help with COVID-19 despite statistics out of Italy that show a number of older health workers succumbed to COVID-19.
But there have been news reports of young health workers also dying. This is a result of risk at a population level.
There are 586,342 health workers in Australia with an average age of 43.4, and if one in 5000 died from exposure at work then that is a shocking 119 deaths. So, a low individual risk can result in tragic story across a large population.

What’s more, from a public health system perspective, this is a great concern, as infected health workers cannot go to work for two to three weeks. If we assume that half are going to be infected, each taking at least three weeks off work, that significantly impacts the health system’s ability to respond.
It equates to 6.2 million days of health worker care lost, which could cause a system overload and lost lives of patients due to COVID-19 (and other causes).
So, what can we do in hospitals to help our staff feel safe, avoid unfounded fear and respond to the real risks to individuals?

Coming clean on hand sanitisers
Firstly, we need to publish the age-specific mortality rates from other settings to reassure younger workers that their risk of dying is very low and that if they are infected they have access to high-level medical care.
We also need to reassure staff that the detailed infection control mechanisms, expert care in Australia and system preparedness, means their risk of death is much lower than in some other countries.
Thirdly, for the sake of the public health system, we must undertake interventions to isolate those health workers who have contact with COVID-19 patients while not wearing appropriate PPE, but do so with full pay, accommodation and family support.
We need to consider protecting older staff and those with co-morbidities by placing them in non-clinical areas or in low-risk settings. For example, we could devise rules around which age group can work in the COVID-19 isolation ward. We all have medical colleagues who are older or who have comorbidity and that means they have high risk from this current pandemic.

And finally, we need to mandate hospitals and the government to continue to prioritise the protection of health workers, to minimise their risk and prevent hundreds of deaths.
At a population level, this will help ensure an effective response is maintained in the face of a potential surge in COVID-19 cases.
Any death of a health worker from exposure at work is a tragedy and all reasonable action must be taken to prevent this. However, for me, a young-ish and healthy doctor, I am just doing my job that has a very small associated risk of death.
In a way, I am in a better position than many in Australia who are facing unemployment and financial stress.

How to take care of yourself if you have COVID-19
While it’s important to maintain the public health importance of protecting health workers, we also need to be clear in communicating about individual risk.
We should avoid spreading fear among low-risk health workers, while making sure that those at high risk are protected. Age specific risk also has implications for the response of low and middle income countries, given the average age of health workers is much younger.
In India, for example, a million Accredited Social Health Activists (AHSAs) are the backbone of the primary health system and they are usually aged between 25 to 45.
And finally, our sympathy and charity need to be extended to all Australia’s heroes who are battling the fallout from the COVID-19 response, not just those in healthcare.
Thanks to Dr Malcolm Anderson at the Melbourne Law School, and Dr Damien Brown, Public Health Registrar, Victorian Public Health Medical Training Scheme and University of Melbourne, for their assistance in preparing this article.
Banner: Luis Ascui/Getty Images